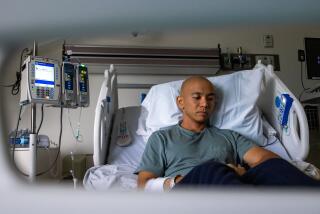
Death by Geography
- Share via
In the world of organ transplantation, location is everything.
After waiting more than a decade for a liver, Jonathan Van Vlack was deteriorating. His gut swelled with fluid, and toxins accumulating in his blood made him forget his own name.
Still, he wasn’t sick enough -- not in New York, where about 2,000 people statewide were vying for the same scarce livers.
“He’s having a very difficult time right now,” his wife, Laura, nervously e-mailed a friend in March 2005. “We really need that liver to come.”
It never did. Van Vlack died in December, on his 53rd birthday.
Frank Evanac was stalled in the same line. By age 53, he had been waiting four years for a liver, and he needed a kidney as well.
After getting a tip at a Fourth of July party, however, he gave up on New York. Without telling his doctors, he moved in with his sister outside Jacksonville, Fla., and joined a new waiting list.
Fourteen days later, a surgeon sewed in his new liver and kidney.
Two very sick men. Two locations. Two fates.
The national transplant system has long prided itself on the principle of fairness: Organs should go to the sickest or those who have suffered the longest.
So sacred is this code that violations forced three transplant programs in California to close in the last seven months: At St. Vincent Medical Center in Los Angeles, the staff took a liver designated for one patient and gave it to another person further down the waiting list. At UC Irvine, viable livers were refused as waiting patients died. At Kaiser Permanente in Northern California, hundreds of kidney patients hastily reassigned to a new program were pushed back in line.
But a far greater inequity is inherent in the U.S. transplant system: When, and sometimes whether, you get an organ depends largely on where you are.
For transplantation purposes, the U.S. is divided into 58 territories, each with its own supply of organs and demand for surgeries. To protect local access to organs, most donated within a territory go to patients waiting there, even if sicker patients are waiting elsewhere.
This design has led to deep disparities, because supply and demand are not evenly spread across the country.
In big cities, for example, social blight boosts disease rates -- and thus the need for organs -- but makes it more difficult to recruit donors. At the same time, transplant centers in less crowded territories are often choosier about who joins their waiting lists. Varying ethnic compositions, car accident rates and the skill of organ recovery agencies all play into whether a territory is flush or deprived.
Sometimes all that separates a wait of years from one of months is a line on a map.
Take the Hudson River. On the New Jersey side, patients much less sick than Van Vlack routinely receive transplants. In Manhattan, patients must reach the brink of death.
The boundaries often defy logic. Even though it has just 28 patients waiting for livers, UC Davis gets first choice of most of the organs recovered in its territory, a circle surrounding Sacramento with a population of 2.4 million people.
It is an island of privilege in a sea of need. The rest of Northern California is a single territory with a population of 11.1 million, with 1,975 people awaiting livers.
These geographic inequities exist for all organs. But the consequences are most dire for liver patients. Kidney patients can survive on dialysis for years, and drugs and artificial devices can help keep heart patients alive.
Without transplants, most patients with liver disease deteriorate until they die.
Evanac was a rare exception. Fewer than 2% of patients are savvy and well off enough to leave town and join waiting lists in other territories.
National regulators acknowledge the disparities but say that at least some are inevitable given a nationwide shortage of organs.
“We think the system is working very well,” said Dr. James Burdick, transplant division director at the U.S. Health Resources and Services Administration. Still, he said, “we think it could be improved.”
It is feasible, at least scientifically, to have another system, one in which livers regularly move across territory lines to the sickest patients. In an ice-cold preservation solution, livers suffer no significant damage in the first 12 hours after harvesting.
But in most cases, nothing forces organ-rich territories to share. As a result, the system has evolved into a collection of self-interested fiefdoms, some blessed, some wanting.
The longest lines for livers are in the territories surrounding New York, Los Angeles and San Francisco, which together account for 30% of the 17,222 people waiting nationwide. UC San Francisco Medical Center has the nation’s longest list, followed by the hospitals of New York University, UCLA and Stanford.
Evanac is a backhoe driver, not a statistician. But he could see the problem.
“If he doesn’t have the parts,” Evanac said of his doctor at NYU, “he can’t put them in.”
Big-city programs are filled with patients like Jonathan Van Vlack.
He joined the waiting list at New York’s Mount Sinai Hospital in 1993, after doctors found his liver was failing. They suspected fatty liver disease, a largely genetic condition.
Van Vlack, a consumer fraud investigator from Woodstock, N.Y., would not need the transplant immediately. He tired easily and sometimes felt numbness in his hands and feet, but he was strong enough to work. It went on like that for a decade.
Patients with liver disease are often able to live normally for years, because the organ has the capacity to regenerate, crisscrossing damage with scar tissue. Eventually, though, the liver stiffens, making it difficult for blood to flow through it. Then problems multiply.
One morning in early 2004, Van Vlack didn’t recognize his two children or Laura, who called an ambulance.
It was the first of many bouts of encephalopathy, which is marked by confusion resulting from ammonia buildup in the blood. At one point, Van Vlack thought he was President Bush.
Even so, there were hundreds of patients in New York deemed sicker than he.
Since 2002, livers have been allocated based on a score derived from three blood serum measurements, and Van Vlack’s score was too low. This policy, which virtually eliminated waiting time as a factor, was aimed at distributing livers on an objective medical basis -- at least within a given territory.
Van Vlack’s swollen abdomen had to be drained regularly. The muscles in his chest, shoulders and legs atrophied.
In the liver, which regulates dozens of blood proteins, filters toxins, produces bile and stores iron and energy, disease strikes as a series of ambushes.
“Jon fell on Thursday night, hit his head and caused a completely detached retina,” his wife wrote in an e-mail to a friend in November 2004.
Soon he stopped working, and he had to give up the weekly consumer column he had written in the local newspaper.
A doctor mentioned that there were other places where the waiting time was shorter. But Van Vlack could not imagine having his transplant anywhere else. The doctors at Mount Sinai knew his case so well.
And he seemed so close: In January 2005, the transplant center called to say a liver was available, so the family piled into a minivan and drove three hours to the hospital amid a blizzard.
Then the doctors canceled the operation. The local blood bank could not supply enough transfusions for his blood type, which contained a rare antibody.
There were more liver offers that year, but the organs were of questionable quality. They had already been turned down by centers elsewhere in the country, and, after careful consideration by Mount Sinai doctors, were deemed too risky for Van Vlack.
Livers vary widely, with the best typically coming from young brain-dead accident victims and the least desirable from donors older than 70. Marginal organs work best in healthier patients and fail at a greater rate in very sick patients like Van Vlack.
Only the patients at the very top of the lists get first offers of pristine organs.
Van Vlack’s family tried everything. A brother considered donating part of his liver, but a biopsy showed signs of fatty liver disease too.
At one point, the hospital arranged a procedure known as a domino transplant. A patient higher on the waiting list would get a new liver from a brain-dead donor, and Van Vlack would get his old organ, which had a defect that in a decade or more would cause neurological problems.
“We were so desperate to get him something,” said Dr. Thomas Schiano, a liver specialist at Mount Sinai.
But the patient inexplicably backed out of his surgery.
Laura tried to ignore the physical signs of Jonathan’s decline.
“When he gets a new liver, I will help him recover,” she wrote in her diary last fall. “We will rebuild our lives together.”
As Van Vlack’s liver scarred and hardened, surrounding vessels burst, causing him to vomit blood. He made at least seven trips to the local emergency room in 2005.
Four days after Christmas, he died of a bacterial infection at Mount Sinai -- one of 61 people on the hospital’s waiting list who did not survive in 2005.
In Van Vlack’s final year, the hospital repeatedly petitioned a review board -- made up of physicians from other New York transplant centers -- to move him up the list. They argued that his bouts of bleeding and other complications were worth extra points on the scoring system ranking liver patients.
All appeals were rejected.
“Difficult case,” one reviewer wrote, “but little to differentiate him from many.”
More than 1,800 of the 6,121 livers transplanted in the United States last year went to patients deemed healthier than Van Vlack, based on a Times analysis of his scores and national transplant data.
A few dozen were just across the Hudson River, at University Hospital in Newark, N.J. Hundreds more were scattered throughout the Deep South and the Midwest or concentrated in tiny pockets of organ prosperity.
How this came to be is a story of demographics, hospital economics and regional politics.
The national system grew out of a 1984 bill sponsored by then-Sen. Al Gore to regulate what had become a free-for-all competition among kidney surgeons. Essentially, they found organs by networking with colleagues and forging alliances with hospitals.
The legislation sought to increase donation, prevent organ trafficking and distribute organs “equitably among transplant recipients according to established medical criteria.”
Most details were left to the United Network for Organ Sharing, a Richmond, Va., nonprofit that won a government contract to set up and run the system.
With the network governed and financed primarily by transplant centers, localism prevailed.
The system’s building blocks were dozens of organ banks, many originally formed by university hospitals to feed their kidney transplant centers. With federal approval, the banks sliced the country into a patchwork of organ territories, some stretching across hundreds of thousands of square miles, others carving up tiny states.
To guarantee each part of the U.S. a supply of organs, the network decided that patients within a territory would be given first dibs on organs collected there, and, in most cases, only leftovers could be offered outside.
The thinking was that supply and demand were functions of population and that each territory could provide for its own.
That reasoning turned out to be flawed.
Car crashes and strokes, the leading precipitators of organ donation, are not uniformly distributed across the country.
In addition, some organ agencies are better than others at finding potential donors and persuading their grieving families to consent. In diverse cities such as Los Angeles and New York, the agencies face heavy mistrust and misunderstanding, particularly from minorities.
Demand also varies widely, with some of the greatest organ failure rates in big cities, largely because of the concentration of poverty, addiction and minority groups prone to certain diseases that cause organ failure.
Although the system was set up for kidney distribution, the shortcomings became apparent as the number of liver programs grew.
In 1983, the year before the organ bill passed, there were just 12 liver transplant centers. Without competition, they could draw organs from around the country.
But as more and more hospitals sought the prestige and profits of transplantation -- the average liver transplant now costs more than $350,000 -- the large urban programs found their organ supplies depleted. Livers increasingly were dispatched to patients at the newer centers in less crowded territories, even as demand rose at already crowded urban centers.
Today there are about 120 liver centers. Although 25 hospitals accounted for half of all liver transplants last year, large programs are vastly outnumbered by smaller well-supplied centers that, together, have come to define -- and defend -- the rules of organ distribution.
“Most of my patients come from the Appalachian Mountains,” with some too poor even to afford telephones, said Dr. Dinesh Ranjan of the University of Kentucky. Without a guaranteed local supply of livers, he said, “they are not going to travel to Boston or L.A. to get a transplant. They are going to stay here and die.”
There is another reason that smaller centers like the current system: It allows them to put high-quality organs into patients before they become extremely ill. That boosts their success rates. Big-city surgeons deride such programs as “boutiques.”
Consider UC Davis, which last year performed just 22 liver transplants. The organs went to one of the healthiest patient pools in the country, according to national statistics. The hospital has fought attempts large and small to institute broader organ sharing. That would force its patients to wait months or years to become as sick as those in San Francisco, with one of the sickest pools in the country. It might force UC Davis out of the liver transplant business.
“We’re trying to survive as a center,” said Dr. Richard Perez, UC Davis’ head of transplantation.
What is good for parts of the system, however, can be bad for the whole.
In the late 1990s, Donna Shalala, then secretary of Health and Human Services, attacked the national transplant system as serving the financial interests of hospitals instead of the needs of patients. She proposed breaking down arbitrary borders to allow more livers to reach the country’s sickest patients.
A rebellion ensued.
Nine states, most of them relatively well supplied with organs, passed laws or resolutions to prevent organs from being exported without first being offered to patients inside state lines.
The federal government had little choice but to back down.
“That fight was so divisive in the late 1990s,” said Dr. Goran Klintmalm, head of transplantation at Baylor University in Texas. “When that fight was over, nobody wanted to touch it again.”
Now the focus is on refining the existing system. For example, there are efforts to encourage more splitting of livers, using part of one lobe for a child and the rest of the organ for an adult. And a six-state region -- from Missouri to Wyoming -- is considering sharing livers more broadly for the sickest patients, said Dr. John Lake, a University of Minnesota transplant surgeon who heads the national organ network’s liver and intestine committee.
“You can look at it one of two ways,” he said. “Let’s ram this down people’s throats, or let’s try to do this more slowly, demonstrating that we are saving more lives with smaller steps.”
In the meantime, the system produces winners and losers.
A Jacksonville hospital saw an opportunity in the inequity -- and so did Frank Evanac.
Evanac walked to his hospital room window, scanning the sky for a helicopter. He knew one was on the way with the liver and kidney he needed so desperately.
“I just hope this thing goes through,” said Evanac, who had been living with his sister for two weeks, waiting for the hospital to call.
He had come to the super-center of liver transplantation. St. Luke’s, a Mayo Clinic hospital, achieved this status by capitalizing on its location, turning the national system’s disparities to its advantage.
Florida has long been flush with organs, thanks to some of the highest donation rates in the country. The state’s organ agencies say they are among the best at tracking down potential donors.
But St. Luke’s has an extra advantage: It is surrounded by territories in which hospitals are extremely choosy about which livers they accept.
The 8-year-old program vacuums up many of the organs the other centers refuse. Last year, its six surgeons procured at least 95 livers from Mississippi, Georgia, South Carolina and Arkansas. Puerto Rico, which has no liver transplant centers, provided 32.
The result is the shortest waiting time in the country -- a median of six weeks, compared with a nationwide figure of a little more than three years. The hospital performed 246 liver transplants in 2005, leading the nation for the second straight year.
There are rarely more than 65 people on the waiting list at a time -- about a sixteenth of the number at UC San Francisco.
More than half the transplants at St. Luke’s last year were for patients from outside Florida. Nine patients came from Massachusetts, eight from California, eight from Colorado and five from New York -- all states with extreme organ shortages.
Potential patients visit Jacksonville for a series of tests and go home to await the results. If accepted into the program, they return to join the waiting list. St. Luke’s requires transplant candidates to be able to get to the hospital within an hour. For the patients scattered through the gated condominium complexes and extended-stay hotels, Jacksonville is the land of plenty.
“If you need an organ, it’s the place to go,” said Evanac, who believes that he contracted hepatitis B in the late 1960s during a weeklong experiment with heroin. His liver and kidneys failed together, leaving him dependent on dialysis and too weak to hold up his Harley-Davidson.
His organs arrived at St. Luke’s on Feb. 21. That evening, a nurse wheeled him into operating room No. 14.
“Are you here for a liver?” a nurse asked, helping him to climb onto a table.
“And a kidney,” he said.
Minutes later, he was sedated.
The organs arrived on ice in clear plastic bags. The surgeon, Dr. Darrin Willingham, reached into a rust-colored solution, pulled out a 3-pound liver and deposited it in a shallow plastic bowl.
He stood over the liver, trimming and stitching protruding veins. “It’s beautiful -- doesn’t look granular, doesn’t look fatty,” he said.
Not every liver looks so good.
Six hours into Evanac’s transplant, the phone rang in the operating room. It was a liver offer for another patient.
Earlier that day, St. Luke’s had turned down the same liver for another patient. Now, because no other center wanted it, Mayo was given a final chance to use it for any patient it wanted -- perhaps somebody healthier further down the list.
As a nurse held the phone to his ear, Willingham called another surgeon, Christopher Hughes, asking for his opinion.
A few minutes later, down the hall, Hughes was peering through a microscope at a biopsy slide.
St. Luke’s hates to turn down a liver, he said, but there were just too many fat cells.
Less-than-ideal organs stand a higher chance of failure. Within a year of their surgeries at St. Luke’s, 8.8% of patients get transplants again -- a rate double the national average.
The hospital can afford to take that chance, Hughes said. In Florida, it is easy to find replacement livers, keeping St. Luke’s survival rate above the national average of 86%.
More patients are on the way. The national organ network recently began requiring hospitals to tell patients that they might get transplants faster by joining multiple waiting lists.
Evanac, who turned 54 in March, is back home in Staten Island now. NYU called his house recently to remind him to come in for blood tests to update his ranking on its waiting list.
His son explained that he was no longer waiting.
Evanac is strong enough to climb onto his backhoe and is planning to get his Harley running again. He is confident enough to allow himself a few cigarettes a day.
In the meantime, there is no end in sight to the national organ shortage. The number of people in need of livers continues to grow, widening the gap between supply and demand.
The competition for organs will only intensify as territories fight to keep local supplies.
Some patients, surgeons said, have managed to escape the system entirely. They have discovered a new a land of plenty -- far from the United States and its rules.
It is advertised on the Internet, the prices are a bargain, and livers are abundant.
China executes several thousand prisoners a year with gunshots to the head, then harvests their organs.
*(BEGIN TEXT OF INFOBOX)
How the System Operates
The U.S. organ allocation system consists of 11 regions, which are broken down into 58 territories. When a liver from a deceased donor becomes available, it is generally offered first for patients of compatible blood type in the territory where it was recovered, starting with the sickest and moving down the list until the organ is accepted.
The order of the list depends on three blood tests used to assign each patient a number, from 6 to 40, known as a MELD score. The higher the score, the sicker the patient. If two patients have the same score, waiting time breaks the tie.
Subpar quality is the main reason doctors turn down livers.
If all the transplant units in a territory refuse a liver, it is offered for outside patients, first in the region, then nationwide.
Some exceptions:
* Although most people needing livers have chronic diseases that cause slow deterioration, some have suffered sudden liver collapse -- for example, from a Tylenol overdose. These patients, who face imminent death, get first choice of livers regionwide. They accounted for 552 of the 6,121 U.S. transplants of livers from cadavers last year.
* If a territory has no patient with a MELD score of at least 15, a liver recovered there is offered first for candidates across the region. This policy, implemented last year, is based on studies showing that in patients with MELD scores of less than 15, the risk of death during surgery is greater than the risk of death from liver failure.
At backlogged centers, patients typically do not receive transplants until they reach MELD scores of 25 or higher.
* Florida, which is divided into four territories, requires that livers be offered statewide before they are offered across the region, which includes five other Southern states and Puerto Rico. Illinois, Minnesota, Wisconsin, Tennessee and Ohio also have rules limiting the flow of livers outside their borders.
* In New York, which has four territories, livers go to the sickest patients statewide. Most are in the New York City area, where four of the state’s five liver transplant units are located.
* Patients younger than 18 get an advantage in priority for organs from other minors.
*
(BEGIN TEXT OF INFOBOX)
Waiting for a liver transplant
The U.S. is divided into 58 transplant territories, each with its own supply of organs from deceased donors and its own demand for transplants. Some territories have non-contiguous portions. In some parts of the country, most patients become very ill before they receive liver transplants. In others, patients spend less time on waiting lists and are still relatively healthy when organs become available for them.
A sample of liver transplant centers:
New York (Mount Sinai Hospital)
% waiting 3 years or more**: 69%
No. on current waiting list**: 471
No. of transplants performed, 2005***: 147
---
Durham, N.C. (Duke University Medical Center)
% waiting 3 years or more**: 59%
No. on current waiting list**: 251
No. of transplants performed, 2005***: 39
---
San Francisco (UCSF Medical Center)
% waiting 3 years or more**: 58%
No. on current waiting list**: 986
No. of transplants performed, 2005***: 143
---
Boston (Massachusetts General Hospital)
% waiting 3 years or more**: 50%
No. on current waiting list**: 212
No. of transplants performed, 2005***: 46
---
Los Angeles (UCLA Medical Center)
% waiting 3 years or more**: 42%
No. on current waiting list**: 661
No. of transplants performed, 2005***: 200
---
Newark, N.J. (University Hospital)
% waiting 3 years or more**: 33%
No. on current waiting list**: 189
No. of transplants performed, 2005***: 87
---
Davis, Calif. (UC Davis Medical Center)
% waiting 3 years or more**: 14%
No. on current waiting list**: 28
No. of transplants performed, 2005***: 22
---
Charleston, S.C. (Medical University of S.C.)
% waiting 3 years or more**: 5%
No. on current waiting list**: 38
No. of transplants performed, 2005***: 45
---
Jacksonville, Fla. (St. Luke’s Hospital)
% waiting 3 years or more**: 3%
No. on current waiting list**: 63
No. of transplants performed, 2005***: 246
---
Indianapolis (Clarian Health-Methodist/IU/Riley)
% waiting 3 years or more**: 1%
No. on current waiting list**: 74
No. of transplants performed, 2005***: 176
---
U.S. total (all centers)
% waiting 3 years or more**: 41%
No. on current waiting list**: 17,222
No. of transplants performed, 2005***: 6,121
---
** As of June 2
*** Does not include transplants from living donors.
Source: United Network for Organ Sharing. Graphics reporting by Alan Zarembo
Descriptors: ORGAN TRANSPLANTS; MEDICAL CARE; GEOGRAPHY; MEDICAL ETHICS
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.