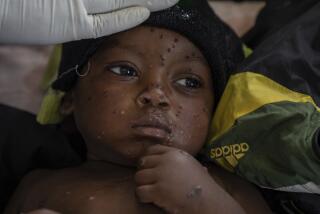
Malaria’s sting spreads as temperatures rise
- Share via
THANGATHI, KENYA -- The boy was feverish, vomiting, and wouldn’t eat. His mother rushed him to a village clinic, suspecting measles, typhoid or one of the other usual childhood ailments found in Kenya’s central highlands.
Instead, the doctor diagnosed a disease she knew little about: malaria.
Though it is Africa’s biggest killer, malaria has always been a regional blight. In the secluded coffee-farming villages around Mt. Kenya, malaria was rare, something other people had to worry about, in the sun-baked west or along the steamy coast.
“When I was growing up, we never heard of malaria,” said Charity Njuki, 31, whose 2-year-old son, Eric, recently contracted the mosquito-borne parasite that causes the disease. Her older children, ages 14 and 10, hadn’t had it. “I was really surprised.”
The emergence of malaria makes Thangathi, a tiny town about 60 miles north of Nairobi, one of the new fronts in the global struggle with a changing climate, as villagers here grapple with the effects of rising temperatures.
Industrialized nations, including the United States and China, account for the vast majority of carbon dioxide emissions blamed for warming the planet, but poorer countries, particularly in Africa, are the most vulnerable to its effects, experts say.
Worldwide temperatures rose 1.3 degrees Fahrenheit during the last 100 years, but recent studies suggest temperatures in Africa are climbing faster. In Kenya’s western highlands, maximum annual temperatures over the last 20 years are up about 1.8 degrees, according to Kenya’s Centre for Global Health Research.
Fifteen years ago, malaria couldn’t reach Thangathi, perched at nearly 6,000 feet amid steep, coffee-covered mountains. The 1970 national atlas declared the region “malaria-free,” thanks to cool weather year-round, with temperatures often dipping below 65 degrees -- too cold for the strains of anopheles mosquito that carry malaria.
Today, however, malaria beats AIDS, stomach parasites and skin infections as a cause of illness here, said Peter Mbugua, regional medical officer for Nyeri district, which includes Thangathi. Since 2001, his malaria caseload has nearly doubled, reaching 206,369 last year; the disease’s prevalence in the region is now second only to pneumonia.
“The situation changed very quickly,” Mbugua said. “Malaria became a concern all of a sudden.”
A noticeable warming
In Thangathi, most residents are unaware of the international concerns over global warming, but many say they have noticed subtle weather changes over the last generation.
Thanks to increased sunshine, corn seems to grow faster, maturing in three months rather than four. Last summer, temperatures were so high that the flowers on passion fruit trees burned.
David Gachanja, 42, who grew up in Thangathi and runs a private clinic, recalled his parents bundling him in a sweater and coat during the cold, wet month of June. This June, he sent his children to school in light jackets and short pants, thanks to temperatures in the mid-70s.
“It’s ever-hot,” said Boniface Maina, the local tribal chief. He said the region was experiencing other weather changes, such as longer rainy seasons and occasional showers during traditionally dry months.
At the government health dispensary in Thangathi, that has meant a steady rise in malaria cases. Clinic officials are uncertain about the exact number because they lack a simple blood test, available in many other parts of the country, that can confirm the disease in less than half a hour. The private clinic nearby has the test, but most villagers can’t afford the 70 cents it costs.
In the early 1990s, if a local doctor came across a case of malaria, it almost always involved a person who had traveled to the lowlands. But in recent years, scientists and health officials have repeatedly confirmed that anopheles mosquitoes are working their way up the slopes of Mt. Kenya, thriving at higher altitudes than ever before.
Willis Akhwale, head of Kenya’s Anti-Malaria Control Division, cited a number of factors for the emergence of malaria in the central highlands, including higher temperatures, increased mobility of the population and land-use changes, such as channeling of rivers and irrigating crops, which can create stagnant pools where mosquitoes breed.
Mosquito biology
But scientists say climate change is the root of the problem, because without higher temperatures, mosquitoes could not thrive.
“It’s a simple issue of mosquito biology,” said Andrew Githeko, a biologist at the government-run Kenya Medical Research Institute. “They are driven by temperature.”
Anopheles mosquitoes live an average of only 21 days, and at a temperature of 65 degrees or lower, it takes the malaria parasite 56 days to mature, Githeko said. In short, the bugs die before they can become contagious. But at 72 degrees or higher, the parasite’s cycle is reduced to less than three weeks, increasing chances of transmission.
At a national level, antimalarial efforts are still directed at coastal and western provinces, the regions that account for the bulk of Kenya’s malaria infections -- 12 million to 15 million cases a year and 34,000 deaths. But Akhwale said the spread of malaria to the central highlands was a growing concern, helping to increase the number of Kenyans “at risk” for malaria to 24 million from 20 million in 2000. Kenya’s population is nearly 37 million.
“In the past, we could ignore areas like central highlands,” Akhwale said. “Not anymore.”
Preventive efforts
Population Services International, a Washington-based nonprofit, last year made a sweep through the highlands, including Thangathi, conducting malaria-prevention seminars and selling low-cost mosquito nets. It was the first and only antimalarial campaign anyone here can remember.
Last year was also the first time Mbugua ordered mandatory antimalarial drugs for pregnant women. This year, he hopes to find money for spraying insecticide at schools, particularly in August, peak malaria season.
He and other experts worry that the lack of awareness and increased exposure to malaria could lead to epidemics, such as one last year at a local girl’s high school in which nearly 300 students fell ill in two weeks, Mbugua said. Officials, who linked the outbreak to poor water drainage behind the dormitory, put the entire student body on antimalarial treatment as a precaution and temporarily canceled classes.
“People in the highlands have not developed an immunity to malaria as they have in other parts of the country where malaria is more common, so the intensity of the malaria outbreaks is much higher,” said Shem Wandiga, a University of Nairobi chemistry professor who has studied the links between malaria incidence and rising temperatures.
Given the lack of experience, treatment in the highlands is often based on trial and error.
Glassy-eyed and sluggish, Alex Maina, 5, sat on his mother’s lap as Margaret Gichuki, a doctor at Thangathi’s government clinic, placed a thermometer under his armpit.
“This child was here two days ago, but now he’s back with vomiting, diarrhea and hotness of the body,” Gichuki said. “It’s most likely malaria.” If the drugs she prescribes don’t work, she said, she’ll try something else.
Lack of awareness
Among villagers, there’s also confusion about the disease and how to prevent it. Some falsely believe malaria is transmitted by mango trees or fermented porridge. Others think it can drive a person insane.
“Nowadays people are thinking that every headache they get is malaria,” said Gachanja, who runs the private clinic.
Such errors can be fatal, he said, even though malaria is treatable and the antimalarial drug Coartem is widely available in Kenya.
Recently, one of Gachanja’s patients waited too long before seeking treatment. The 55-year-old woman developed anemia and died, he said.
Many villagers are still unfamiliar with methods to protect themselves, such as clearing brush, eliminating pools of stagnant water, avoiding mosquito-prone areas at dusk and sleeping under treated nets.
Charity Njuki, whose son Eric recovered from his bout with malaria, said she suspected mosquitoes were laying eggs in a large water tank the family built next to the house about 10 years ago. But there are no plans to move the tank or spray around it.
Asked what she might do to protect her family from malaria, she mentioned receiving one of the mosquito nets from Population Services last year. But she said she hadn’t used it and thought it might be with her husband in Nairobi, where he works during the week.
With peak malaria season approaching, her son sleeps without a net.
“You think I should bring it back?” she asked. “I don’t want to go through this again. The boy suffered so much. We’re just not used to dealing with malaria here.”
edmund.sanders@latimes.com