Weight-loss surgery may reduce depression in some patients, study suggests
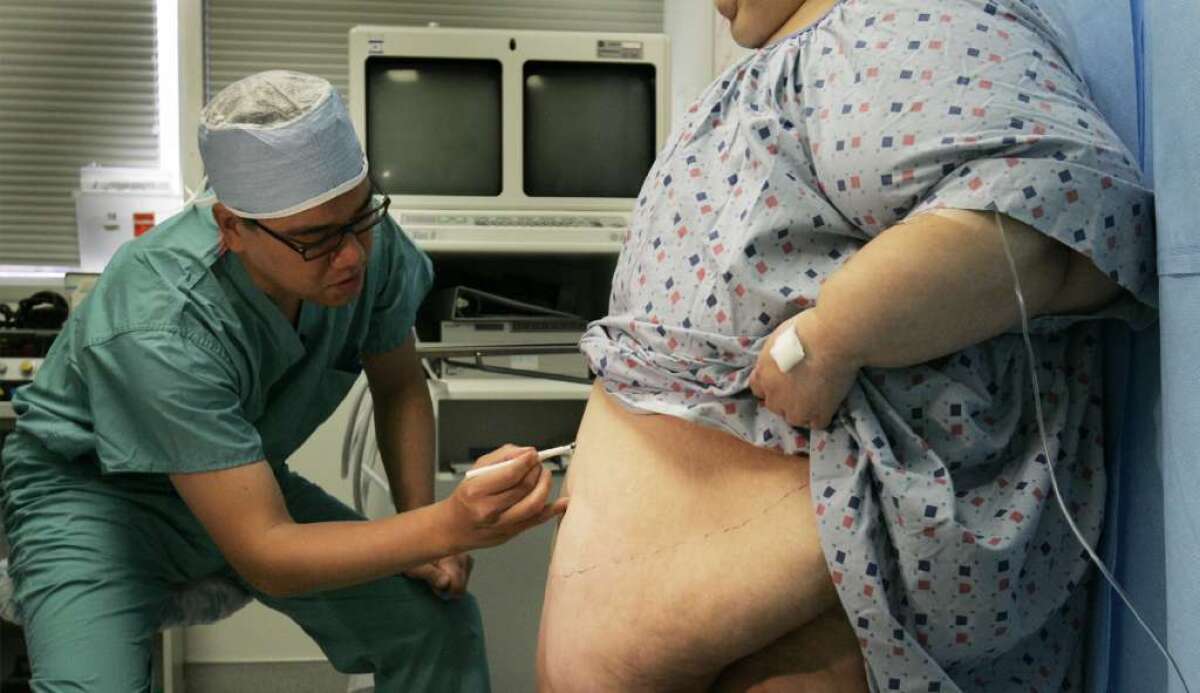
Dr. Carson Liu outlines skin flap on a patient just before removing over 48 pounds of skin and fat in a lap–band surgery in 2006. The patient had weighed over 500 pounds. A new study examines the link between bariatric surgery and mental health.
- Share via
For some severely obese patients, a new study hints that bariatric surgery might potentially do good for both body and mind. Patients seeking and undergoing such weight-loss procedures were more likely to suffer from depression and binge-eating than the general population -- but those with depression often saw their mental health improve after surgery, a new UCLA-led paper shows.
The findings, published this week in JAMA, don’t establish a causal link between bariatric surgery and improved mental health. But they do reveal a surprising relationship that will have to be further probed by more research, scientists said.
“Although our results should not be interpreted as indicating that surgery is a treatment for depression, severely obese patients with depression may gain psychological benefits in addition to the physical benefits already associated with surgery,” the study authors wrote.
Bariatric surgery comprises a variety of different procedures, including the gastric bypass or a gastric band, that are used to help often severely obese people lose weight. Mental health is often linked in some form to these procedures -- insurance companies typically require patients to get a mental health evaluation before they can get approval to undergo the surgery.
Join the conversation on Facebook >>
But although the link between mental health and bariatric surgery has been studied before, it’s usually been done by individual institutions rather than on a larger scale, said Dr. Aaron Dawes, a surgical resident at the David Geffen School of Medicine at UCLA and the study’s lead author.
“I think most physicians would understand or not be surprised by the idea that mental health conditions are more prevalent in this population of patients,” Dawes said. “What we didn’t really know was how prevalent they were.”
To get at that relationship, the researchers performed a meta-analysis, culling data from 68 papers. Fifty-nine of them, involving some 65,363 patients, looked at the prevalence of mental health conditions before the operation; 27 of them, involving 50,182 patients, looked at the link between mental health conditions before the study and the outcomes afterward.
NEWSLETTER: Get the day’s top headlines from Times Editor Davan Maharaj >>
The researchers found that patients who were about to undergo bariatric surgery had rates of depression (19%) and binge-eating disorder (17%) that were both more than twice as high as they were in the general population (about 8% and 1% to 5%, respectively). Overall, 23% of patients had symptoms of at least one mood disorder.
But that higher rate of some mental health conditions didn’t seem to affect the outcomes; researchers found essentially no significant difference in weight loss between those with and without pre-surgery depression a year after the surgery.
“I think there’s a general idea that mental health conditions might preclude patients from having bariatric surgery, because they’re either not very good surgical candidates or they won’t stand to benefit,” Dawes said. “We didn’t find that in the evidence. We really found no strong evidence that suggests that mental health conditions limit the weight loss after surgery.”
On top of that, the researchers discovered that having bariatric surgery seemed to be linked with lower rates of depression after the procedure.
“We were pretty surprised to find a somewhat dramatic drop in both the incidence of depression and the severity of the depressive symptoms after the operation,” Dawes said.
This study can’t determine exactly why this relationship seems to exist, he added. Probing the causes behind it will be up to future study.
But the findings offer an intriguing hint that perhaps, for some patients with severe obesity, certain mental health conditions might be treated as part of the physical disease rather than a separate, often stigmatized, confounder.
“It may help us think about mental health conditions in this population kind of like physical health conditions, in that they may be obesity-related comorbidities,” Dawes said. “So just as we see diabetes or sleep apnea improve, to the extent that some of these conditions are really driven by the obesity, the surgery may improve some of the mental conditions as well.”
Follow @aminawrite on Twitter for more science news and “like” Los Angeles Times Science & Health on Facebook.
MORE SCIENCE NEWS
Why coming clean is better than ‘hiding’ on job applications and dating sites
Breast cancer screening recommendations clarify science but muddy political waters
Better treatment for breast cancer hasn’t boosted the benefit of mammograms, study says







