Newer types of birth control pills confirmed to raise blood clot risk
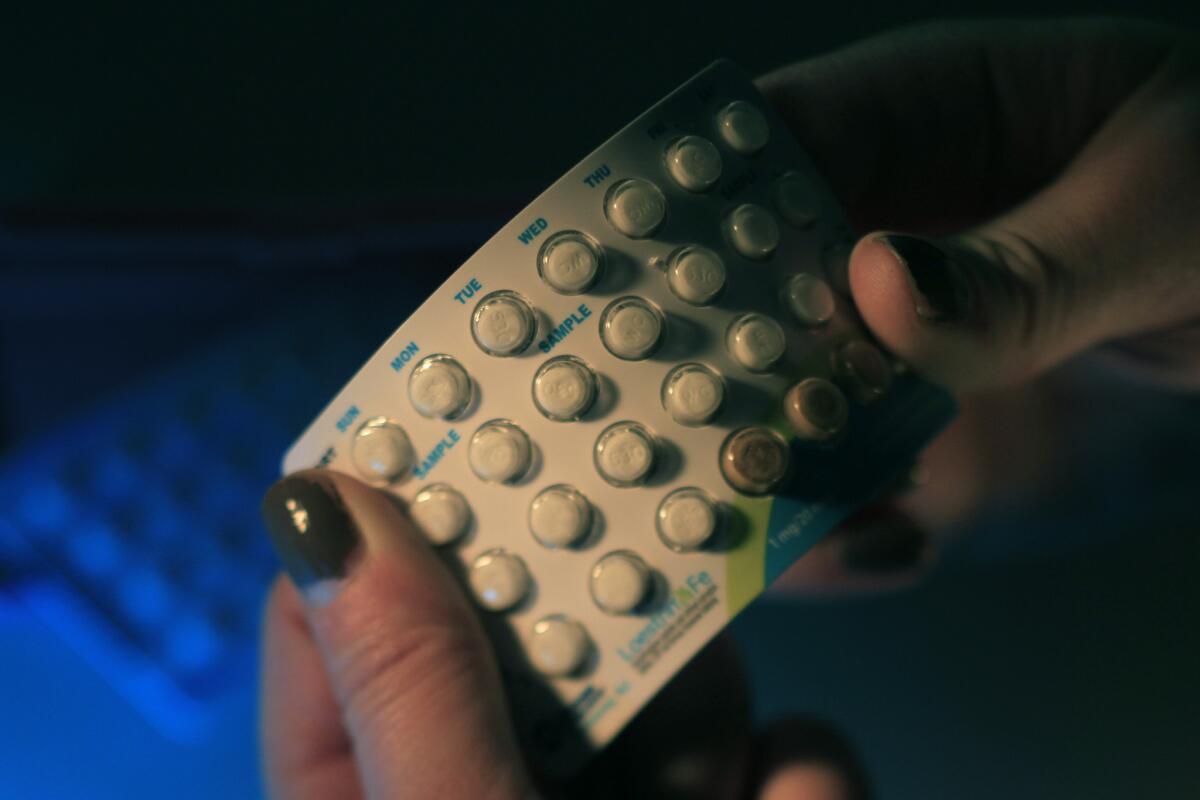
A study of birth control pills showed that those containing newer hormone formulations were associated with a higher risk of blood clotting than older types.
- Share via
Women who take newer types of birth control pills face a higher risk of developing blood clots than women who take older types, researchers said Tuesday, providing what some called “clarifying” evidence that more modern contraceptives designed as safer options may in fact pose more risk than earlier formulations.
Poring over two medical records databases to study more than 50,000 15- to 49-year-old women in Britain, University of Nottingham researcher Yana Vinogradova and colleagues found, as researchers have known for decades, that women who took combined oral contraceptives (formulations that include versions of two hormones, estrogen and progestin) had a higher risk of developing venous thromboembolisms -- dangerous blood clots -- than women who don’t take the pill.
------------
FOR THE RECORD
1:17 p.m.: An earlier version of this article identified an author of this study as Yama Vinogradova. Her name is Yana Vinogradova.
------------
But when the team broke out the data by medication and controlled for other risk factors, they also discovered that certain versions of the birth control pill were associated with higher risk than others. Medications using the synthetic hormones drospirenone (found in Yasmin), desogestrel (found in Kariva and Mircette) and other newer formulations were associated with about a 1.5 to 1.8 times higher risk than older drugs containing synthetic hormones such as levonorgestrel.
The team’s study, published Tuesday in the journal the BMJ, confirms past findings, said Susan Jick, an epidemiologist at the Boston University School of Public Health who wrote an editorial accompanying the report.
“The results provide compelling evidence that these newer oral contraceptives are associated with a higher risk of venous thromboembolism than older options,” wrote Jick, who was not involved in the research but whose Boston Collaborative Drug Surveillance Program has conducted similar analyses in the past.
Around the world, Vinogradova and her coauthors wrote, close to 10% of women of childbearing age use oral contraceptives -- a number that grows to 18% of women in developed countries. The risk of developing blood clots for such women, who are generally healthy, is low but real.
According to Jick, drug makers were attempting to create safer pills when they started using the newer synthetic hormones like drospirenone. “There were all these reasons one would think they should have been safer,” she said in an interview. “And yet they weren’t.”
Confirming the increased risk, however, has been difficult, Jick added, because different studies have been conducted in different ways -- with some methodologies masking the medications’ effects. The new report in BMJ addressed some of the lingering contradictions by analyzing the data through a number of approaches.
For instance, Jick explained, the team broke out statistics for women who were prescribed anti-clotting medications and for women who didn’t have other risk factors for clots: subsets that were more likely to represent true cases of contraceptive-related venous thromboembolism.
In such cases, the association between newer contraceptive use and clotting risk strengthened, providing further indication that the effects the team identified were real.
“People should know that the risk is there,” Jick said.
For more on science and health, follow me on Twitter: @LATerynbrown







