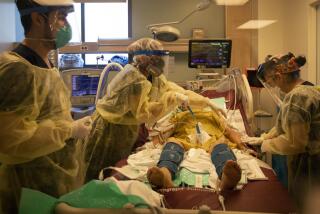
Death rate from cancer now 25% lower than it was 25 years ago, report says
- Share via
In the year to come, an estimated 1,688,780 people in the United States are expected to get a cancer diagnosis, and cancer will claim the lives of a projected 600,920.
That death toll, however grim, represents a death rate from cancer that is 25% lower than it was a quarter-century ago — a drop driven by steady reductions in smoking rates and advances in early detection and treatment. Between 1991 and 2014, that boost in cancer survivorship translates to approximately 2,143,200 fewer cancer deaths than might have been expected if death rates had remained at their peak.
Better treatment protocols and more targeted therapies have driven the most dramatic improvements in the survival of patients with malignancies of the blood and lymph system, says the American Cancer Society’s annual report card on cancer.
In the mid-1970s, patients diagnosed with acute lymphocytic leukemia, for instance, stood a 41% probability of being alive five years later. For patients diagnosed between 2006 and 2012, those survival rates had increased to 71%. For chronic myeloid leukemia, five-year survival rates have increased from a dismal 22% in the mid-1970s to 66%, and new therapies allow most diagnosed before age 65 to achieve near-normal life expectancies.
At the same time, “advances have been slow” in treatment of cancers of the lung and pancreas, the report says, and those malignancies continue to be caught most often when they have reached an advanced stage. Five years after diagnosis, only 8% of pancreatic cancer patients have survived, and 18% of those with lung cancer.
The report also chronicles a relatively recent uptick in both new diagnoses of liver cancer and deaths from that malignancy. The number of new cases of liver cancer has grown by 3% yearly, and liver cancer deaths rose by 3% annually between 2010 and 2014.
Deaths from uterine cancer were also on the rise, increasing by 2% per year in that period.
Men have seen slightly steeper declines than women in cancer deaths — drops of 31% vs. 21% between 1991 and 2014. And despite having cancer death rates that remained 15% higher than that of white Americans in 2014, African Americans have narrowed a long-standing gap.
Over the last three decades, the new report says, the survival rate for all cancers combined five years after diagnosis has increased 20 percentage points among whites, and 24 percentage points among blacks.
The American Cancer Society, which releases the annual survey of cancer trends, credits the Obama administration’s Affordable Care Act, which the incoming Trump administration has vowed to repeal, with improving cancer survival rates in ethnic minorities. In African Americans, and black men especially, cancers have long been discovered later and treated less effectively, a trend that is closely linked to those patients’ lower rates of health insurance and poorer access to healthcare.
Between 2010 and 2015, the Affordable Care Act has shrunk the ranks of the uninsured from 21% to 11% among African Americans, and from 31% to 16% among Latinos.
“These shifts should help to expedite progress in reducing socioeconomic disparities in cancer, as well as other health conditions,” the report says.
The new report continues to tout the role of cancer screening in boosting early detection and treatment of many cancers. But it also reflects a growing willingness among experts and patient organizations to question the value of cancer screening in improving survival rates.
The report cites a tripling of colonoscopy use among adults 50 and older in helping drive down deaths from colorectal cancers. It touts the potential for lung cancer to be diagnosed earlier among current and former smokers with a history of having smoked the equivalent of a pack a day for 30 years or more. (In 2010, fewer than 4% of the 8.7 million Americans eligible for such screening got it.)
At the same time, it notes that decreased PSA testing of men has played a major role in driving down new diagnoses of prostate cancer, and that less aggressive screening for thyroid cancers have greatly reduced new diagnoses of that malignancy. While recommendations for mammographic detection of breast cancer have been scaled back, deaths from breast cancer continue to decline.
Referring to early prostate cancer detection, the authors of the new report wrote “the effect of reduced screening on the occurrence of advanced disease is being watched closely.”
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.
MORE IN SCIENCE
Give peanut-based foods to babies early to prevent allergies, new guidelines say
Less shrinkage: This is your aging brain on the Mediterranean diet
In a first, scientists detect ‘fast radio bursts’ from beyond the Milky Way galaxy