Injectable diabetes medicine drives down weight, too, research finds
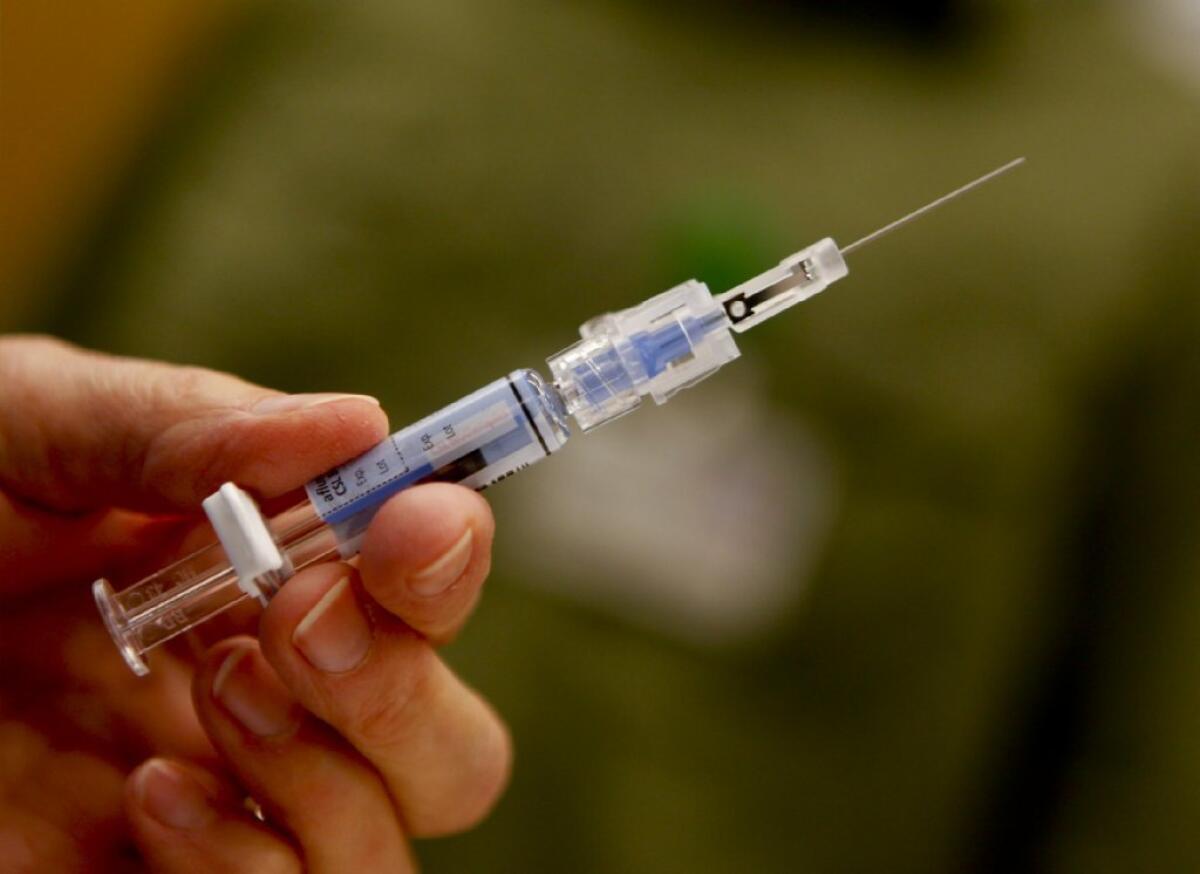
Liraglutide, approved in a lower dose as the diabetes medication Victoza, helped nondiabetic subjects lose more weight, along with diet and exercise, than those taking a placebo, according to new research. The injectable drug’s cost and the fact that it may have to be taken long term could be issues.
- Share via
The diabetes medication liraglutide helped more than twice as many obese subjects in a clinical trial lose 5% of their body weight, and more than three times as many lose a tenth of their body weight, compared with subjects taking a placebo, according to new research.
The drug also appeared to reduce dramatically the risk of developing type-2 diabetes among those taking it. Compared with subjects getting liraglutide, those getting a placebo medication were eight times likelier to be diagnosed with type-2 diabetes during the 12-month trial.
The injectable drug, marketed as Saxenda and produced by Novo Nordisk, was approved last December by the U.S. Food & Drug Administration as a weight-loss drug, partly on the strength of the just-published clinical trial. At a lower dose of its active ingredient, liraglutide (1.8 milligrams vs. 3 millilgrams), Saxenda is marketed as Victoza, a diabetes medication.
Saxenda is the fourth prescription medication to be approved for weight loss by the FDA in the past three years. It joins the drugs Belviq (lorcaserin), Qsymia (a combination of phentermine and topiramate) and Contrave (a combination of naltrexone and bupropion) in the newly fortified arsenal of pharmaceuticals aimed at helping the nation’s 78 million obese adults shed excess weight.
In findings published this week in the New England Journal of Medicine, researchers recruited 3,371 subjects who did not have diabetes but who had a body-mass index of 30 or greater -- classifying them as obese -- or who had a BMI between 27 and 30 (overweight) and had high blood pressure or a worrisome cholesterol profile.
While all got counseling to reduce their caloric intake and increase their physical activity, 2,437 gave themselves once-daily subcutaneous injections of liraglutide, a bioengineered medication that stimulates insulin secretion, slows the emptying of food from the stomach and reduces appetite. Another 1,225 study subjects injected themselves daily with a sham medication.
While 65% of patients getting the placebo medication lost weight, on average 5.7 pounds after a year, of the group that took Saxenda, 92% lost weight, an average of 17.6 pounds after a year.
Among those taking Saxenda, 14.4% lost more than 15% of their body weight (vs. 3.5% of those taking a placebo); 33.1% lost more than 10% of their body weight (vs. 10.6% on placebo); and 63.2% lost at least 5% of their body weight (vs. 27.1% of those on placebo).
Those taking Saxenda also showed greater improvements in metabolic function, blood pressure and cholesterol profiles than did those getting a placebo injection.
“Given previous disappointments with various weight-loss strategies, these are welcome findings,” wrote endocrinologists Elias S. Siraj and Kevin Jon Williams, both of Temple University School of Medicine, in an accompanying editorial.
At the same time, Siraj and Williams wrote, “liraglutide is no cure.”
With a price tag of $1,000 per month, Saxenda’s cost will be a considerable issue, especially as obese patients may need to take liraglutide “indefinitely, like statins,” to maintain their weight loss, wrote Siraj and Williams. In a group of participants who were randomly chosen to discontinue the medication after 56 weeks, the average weight regained in 12 weeks was 6.4 pounds.
In approving Saxenda last December, the FDA also required Novo Nordisk to conduct additional studies to determine whether it increases the risk of breast or thyroid cancers -- both concerns raised in preliminary trials. Siraj and Williams acknowledged both concerns need to be addressed with further research. But they agreed with the authors of the newly published research that higher rates of breast cancers seen in those taking Saxenda were probably the result of improved detection in women who had lost more weight.
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.







