Exercising drives down risk for 13 cancers, research shows
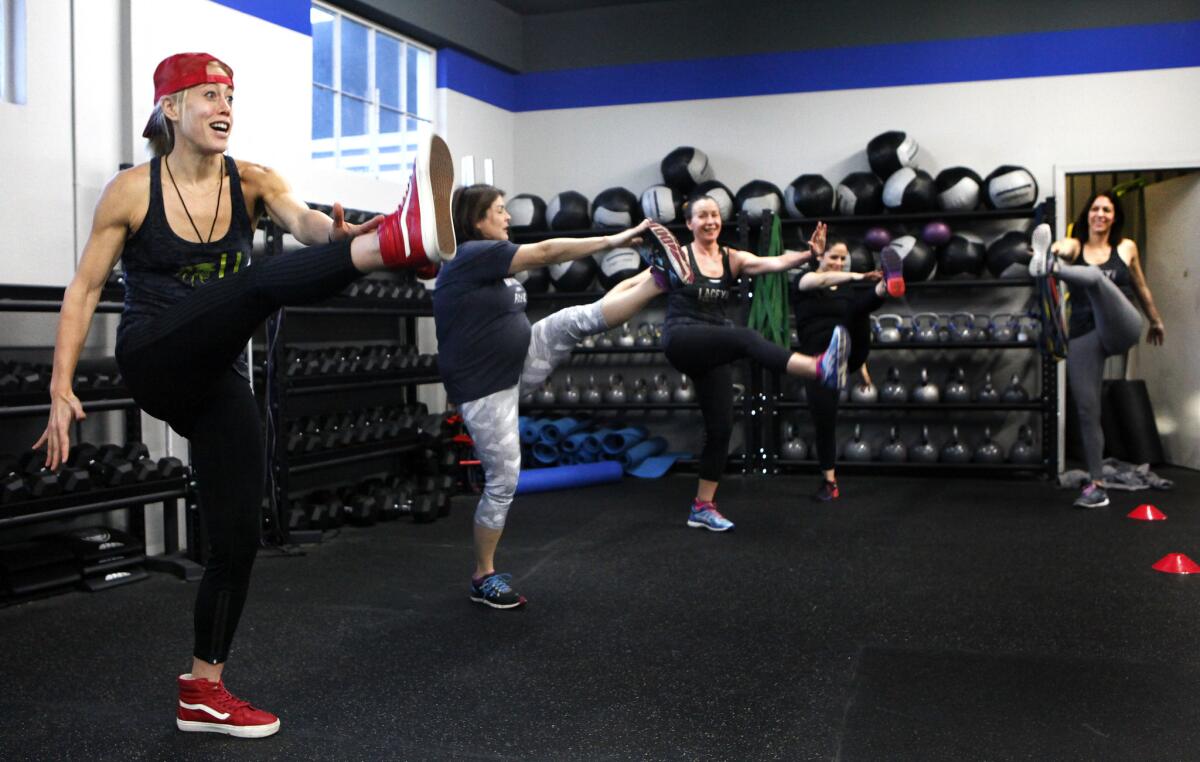
Fitness trainer Lacey Stone, left, leads a boot camp class in Los Angeles in 2015. Researchers have found that high levels of exercise drive down the average risk for developing many kinds of cancers.
- Share via
In addition to protecting hearts, preserving memory and lifting moods, exercise is a powerful cancer-preventive, says new research. Physical activity worked to drive down rates of a broad array of cancers even among smokers, former smokers, and the overweight and obese.
But to get those benefits, researchers concluded, more is better.
In a massive effort to aggregate what’s known about cancer and exercise, researchers calculated that compared with people who reported spending the least time in “leisure-time physical activity,” those who got the most moderate to intense exercise reduced their risk of developing seven kinds of cancer by at least 20%.
See the most-read stories in Science this hour >>
These exercisers were 42% less likely than those who got little to no exercise to develop esophageal adenocarcinoma. They were 27% less likely to develop liver cancer, 26% less likely to develop lung cancer and 23% less likely to develop kidney cancer. Their rates of gastric cardia and endometrial cancers were 22% and 21% lower, respectively, than were those of non-exercisers. And the most frequent exercisers drove their rates of myeloid leukemia down by 20%.
Those who worked out most saw their rates of six types of cancer drop by 10% to 20% compared with those who reported the least exercise. Their rates of myeloma, colon and head and neck cancers were 17%, 16% and 15% lower, respectively. They were 13% less likely to develop cancers of the rectum or bladder and 10% less likely to develop breast cancer.
The researchers called the cancer-reducing power of exercise “suggestive” for cancers of the gall bladder and small intestine and for non-Hodgkin’s lymphoma.
The new research, published online Monday in the journal JAMA Internal Medicine, reflects the collective findings of 12 large U.S. and European research studies in which close to 1.5 million participants reported how much and how often they exercised. Participants were tracked for anywhere from nine to 21 years, and cancer diagnoses were noted.
Participants in seven of the 12 studies included in the analysis reported their physical activity in a variety of ways. But the authors of the current research sought to standardize those and rank them in duration and intensity, giving participants a score between zero and 100.
The median — the point at which 50% did more exercise and 50% did less — was the rough equivalent of 150 minutes of moderate-intensity activity, such as walking, per week. On average, cancer rates fell as exercise levels increased, and the robust reductions reported reflect a comparison between those who got the most weekly exercise and those who got the least.
Against the backdrop of rising rates of smoking- and obesity-related cancers throughout the world, the findings “support promoting physical activity as a key component of population wide cancer-prevention and control efforts,” the authors wrote.
The findings of the new analysis strongly suggest that exercise’s effect on cancer is not solely a function of weight loss, since even overweight and obese participants who were very active saw their risk of developing most cancers reduced. Only for cancers of the liver, gastric cardia and endometrium did the cancer-preventing power of exercise disappear when researchers took into account participants’ overweight or obese status.
In physicians’ offices, the authors noted, the findings suggest that patients who smoke or carry too much extra weight should hear not only that they should quit and lose weight, but that exercise can help reduce their odds of developing cancer.
Only prostate and malignant melanoma appeared to occur more commonly in frequent exercisers than in those who exercised the least — both surprising findings in light of past research. But researchers wrote that increases in exercisers’ rates of prostate cancer (5%) and malignant melanoma (23%) are readily explained. The modest rise in prostate cancers likely reflects the fact that health-conscious men are both more likely to exercise and to be screened for prostate cancer. The more dramatic increase in malignant skin cancer likely reflects that people who exercise the most have a far higher exposure to the sun’s rays than do those who exercise least, they wrote.
The American Cancer Society’s Alpa V. Patel, a co-author of the new study, said that researchers have long had solid evidence that exercise reduces the risk of three of the most common cancers: those of the breast, colon and endometrium. The jury was still very much out beyond that though. So discovery that high physical activity levels are linked to reductions in 10 additional cancers shows that exercise “has far-reaching value for cancer prevention,” Patel added.
In an invited commentary published alongside the new study, epidemiologists from Emery University and the University of North Carolina noted that the analysis leaves some crucial questions for future research, including how, why and how much exercise works to reduce cancer risk.
The factors that drive cancers are many and complex, and they include a range of hormonal, metabolic and immunity-related factors that are nudged in various directions by exercise. Untangling how exercise might (and might not) alter those, wrote the epidemiologists, “should be a high research priority,” both because it could lead to better advice for patients and better ways to treat and prevent cancers.
In addition, they wrote, future research will need to suss out “the exact timing, intensity and dose of physical activity required for cancer risk reduction.” Is lifelong physical activity essential, or can a middle-aged couch potato still reduce her risk by lacing up her sneakers and hitting the gym? At what duration or intensity level do the cancer-prevention benefits of exercise begin to tail off? Just how much of exercise’s benefit is a reward for weight-management and how much can be had even when an obese patient fails to lose any weight?
Such questions “highlight the additional research needed to improve cancer risk-reduction strategies,” wrote Lauren E. McCullough, Katherine M. McClain and Marilie D. Gammon.
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.
MORE SCIENCE NEWS
Want to hold on to important memories? Hit the hay for some deep sleep
Despite autism fears, here’s why pregnant women should keep taking their prenatal vitamins
Butchered remains of 14,550-year-old mastodon in Florida fills in picture of earliest Americans




