In IVF, success rate for frozen donor eggs lags behind use of fresh eggs

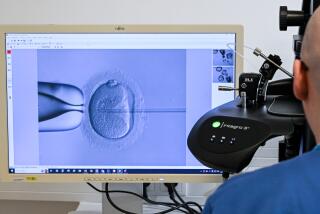
An embryologist tranfers an unfertilized egg from a culture dish into a manipulation dish, where it will be fertilized. A new study finds that in vitro fertilization attempts involving frozen donor eggs were somewhat less successful than attempts using fresh eggs.
- Share via
Hundreds of babies born in the U.S. got their start as eggs donated by women and then frozen until they could be thawed and joined with sperm in a fertility clinic. A new study offers evidence that frozen eggs work well for in vitro fertilization — though slightly less well than fresh donor eggs.
Researchers examined data from 380 fertility clinics that reported their successes and failures in 2013 to the Society for Assisted Reproductive Technology. Those clinics represented 81% of all fertility clinics operating in the U.S. that year, and they performed 92% of all IVF cycles, the researchers wrote.
The researchers, from the Center for Human Reproduction in New York, counted 11,148 IVF cycles involving donated eggs (or oocytes) in 2013, the most recent year for which statistics were available. Of those, 2,227 — or 20% — used eggs that had been frozen (or cryopreserved).
The live birth rate per IVF cycle was 43.2% for women who used embryos derived from once-frozen eggs, slightly less than the 49.6% live birth rate for women whose embryos were created from fresh eggs, researchers found.
The difference was greater when the researchers calculated the number of live births per embryo transferred. This time, the live birth rate was 47.1% for women who had used frozen eggs and 56.1% for those who had used fresh eggs, according to the study.
On average, women who used fresh eggs had 1.7 embryos transferred per IVF cycle, compared with 1.6 embryos for women who used once-frozen eggs, the researchers found.
The results were published Tuesday in the Journal of the American Medical Assn.
Though fertility clinics routinely freeze embryos, they began freezing eggs more recently. Only in 2013 did the American Society for Reproductive Medicine declare that egg-freezing no longer was “experimental,” according to the JAMA report. (The idea of freezing sperm goes back to the 1880s, and women have been using it to get pregnant since 1953, according to this fascinating history of the technology from the California Cryobank.)
Freezing eggs makes in vitro fertilization much more convenient for patients and doctors because the egg donor and the recipient don’t need to have their cycles synced. It also has the potential to make IVF less expensive because eggs retrieved from a single donor can be shared more easily among several women. “However, the added convenience and lower cycle costs must be balanced against the lower live birth rates with use of cryopreserved oocytes,” the study authors wrote.
Since the data from the Society for Assisted Reproductive Technology did not include personal information about the women using in vitro fertilization, the researchers couldn’t make adjustments for the patients’ age, the cause of their infertility or how often they had tried IVF. Nor could they tell what stage the embryo was at the time it was transferred to the uterus. These and other factors might be responsible for some of the difference in using fresh and frozen eggs, the researchers wrote.
It’s not clear why frozen eggs would fare less well than their fresh counterparts. There may be something about the freezing and thawing process that degrades or otherwise harms the eggs, the study authors wrote. Another possibility is that women who use frozen eggs use less of them, so they wind up having fewer viable embryos from which to choose, they said.
The results offer the first side-by-side comparison of fresh and frozen eggs, according to the researchers. But it shouldn’t be the last; “additional studies” are needed, they wrote.
Follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.