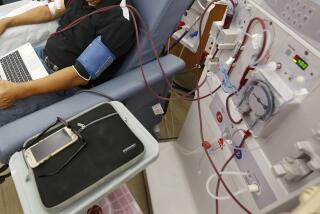
Is there a cost to kidney donation? Yes, but ... says study
- Share via
For the roughly 6,000 people each year who give up a kidney to someone in need of a transplant in the United States, a new study finds that generosity may come at a price: a roughly tenfold increased risk of kidney failure in the 15 years following their donation.
That increased risk, however, tells only half the story -- and not, depending on how you look at things, the more important half.
In the 15 years after he or she goes under the knife, a live kidney donor has a 0.3% likelihood of developing end-stage kidney disease requiring chronic dialysis or a transplant, researchers from Johns Hopkins University have found. While that is higher than the .04% probability he or she would have had as a nondonor, the fact is that kidney failure remains a highly improbable outcome.
The study, published Tuesday in the Journal of the American Medical Assn., is the first to assess both the absolute risk a kidney donor faces after the operation and the added risk he or she incurs as a result of it. It comes at a time when the gap between those needing a kidney transplant and the availability of the organs is vast: About 93,000 Americans are in line awaiting an available kidney, and most will wait at least five years before a kidney from a deceased donor becomes available.
Living donors -- relatives, friends and increasingly strangers -- are narrowing that gap. In 2011, 42.5% of kidney transplants came from living donors, with more than 31,000 such procedures performed in over 100 countries. And while donors are told the loss of a kidney cannot be without risk, they haven’t had many hard facts to guide them in their decision. Now, they do.
“The extra risk they’re taking from donating a kidney was very low,” said Johns Hopkins University transplant surgeon Dorry L. Segev, who led researchers in reviewing the records of all 96,217 people who donated a kidney for transplantation in the United States between April 1994 and November 2011. “It’s actually very reassuring,” he added.
Crucial to this finding is the fact that kidney donors are not only unusually generous: They are also, as a group, unusually healthy. Compared with the U.S. population at large, they start with a much smaller risk of going on to develop kidney disease.
When you take their chance of developing end-stage kidney disease and multiply it by 10, said Segev, “the result is still a very low number.”
To demonstrate how kidney donors might have fared had they not made their gift, the researchers created a comparison group of nondonors from a large national survey of Americans’ health and nutrition. They drew from that database 20,024 men and women with health status and habits very similar to those of donors. And then they tracked those donors for 15 years to see how many developed kidney disease that required ongoing dialysis, placed a donor on a transplant waiting list, or resulted in a transplant.
“Potential donors, if they go through the screening process and are deemed appropriate, are among the healthiest of people walking the planet,” said Dr. Gabriel Danovitch, who heads UCLA’s kidney and pancreas transplant program. But since many donors are directly related to the transplant patient, some may harbor hard-to-detect genetic or familial risk factors, he said. And a fraction of those may go on to develop kidney disease as well.
Danovitch, who was not involved in the current study, says he does not believe the new information will put off would-be donors.
“When it’s done right and best practices are followed, the risks of donation are balanced -- overbalanced if anything -- against the benefit the donor gets from seeing the recipient do well and improving his or her own sense of having done well,” Danovitch said.
In the roughly 30 years he has been performing kidney transplants, Danovitch said, he has rarely seen donors who express regrets -- even if they go on to develop kidney disease themselves. After “thousands and thousands” of transplants, Danovitch reckoned that he saw perhaps five donors who went on to need transplants.
“The halo effect of being a kidney donor is the gain these patients get for the finite, but real -- and small -- additional risk they take upon themselves,” he said.
Now that physicians have hard numbers to offer would-be donors, they should expect that some, at least, will see the increased risk they face and waver, says Dr. Scott D. Halpern, a transplantation bioethicist at Perelman School of Medicine at the University of Pennsylvania.
“People are notoriously bad” at weighing an increased risk of an unwanted outcome against a very low probability it will ever happen, Halpern said. “It’s a normal bias of human decision making.”
If they are to help prospective donors make the right decisions for themselves, said Halpern, transplant surgeons will need to give these individuals a short course in absolute and relative risk, and cast the new numbers in their proper context. That will mean asking would-be donors to focus not just how much likelier they are to get sick if they donate, but how low that probability was to begin with.
Journal of the American Medical