American Cancer Society abandons ‘one size fits all’ advice on mammograms
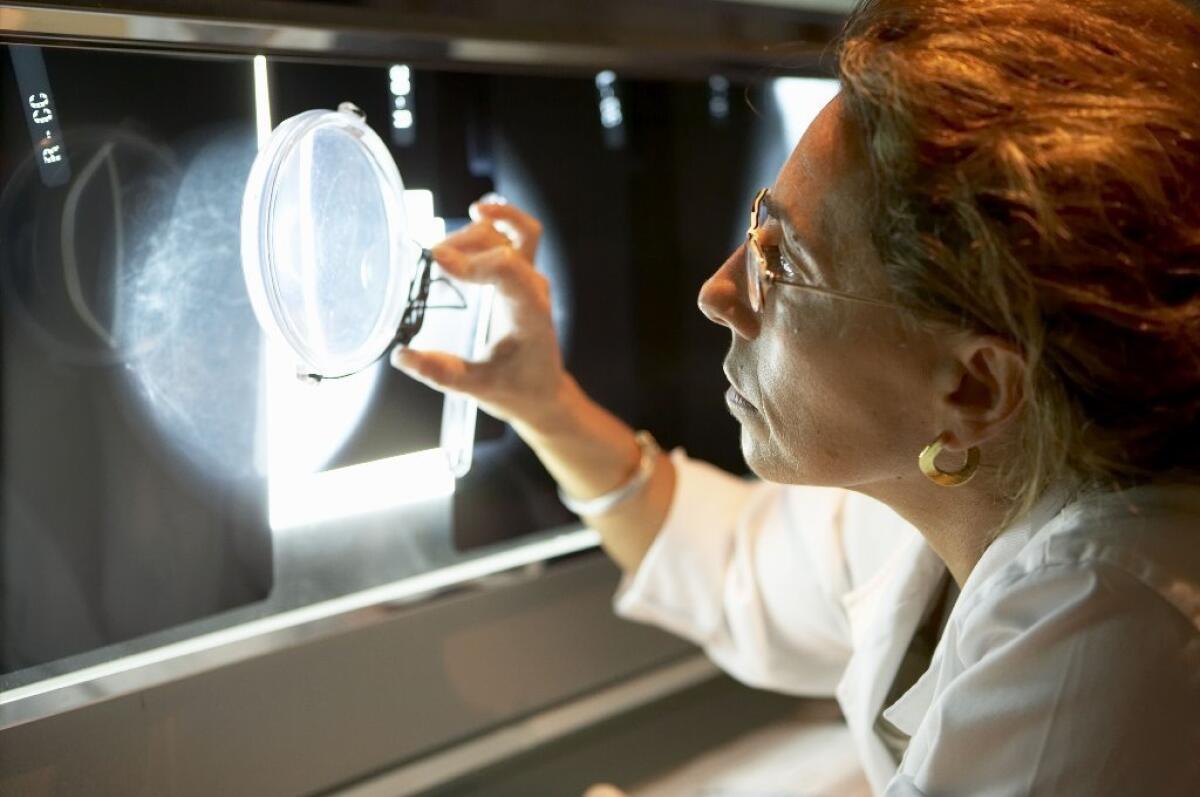
New breast cancer screening guidelines from the American Cancer Society advise most women to start getting mammograms by the time they’re 45.
- Share via
After a thorough review of the benefits and limitations of mammograms, the nation’s top cancer-fighting organization is advising women that they can wait until they are 45 years old to start using the tests to screen for breast cancer.
New guidelines from the American Cancer Society also assure women that they can have fewer mammograms over the course of their lives.
The guidelines, published in Wednesday’s edition of the Journal of the American Medical Assn., are designed for women who are in good health and have no reason to suspect their risk of developing breast cancer is above average. The findings represent a departure from the group’s previous recommendation that all women with an average risk of breast cancer get annual mammograms starting at age 40.
Although the American Cancer Society still endorses that course for women who prefer it, the group acknowledged that some women favor a less-aggressive approach to breast cancer screening. If so, it said, they can delay their first mammogram until they are 45 and wait two years between screenings starting at age 55 without fear that doing so will put their health in jeopardy.
Either way, regular mammograms should continue as long as women have a life expectancy of at least 10 years and are good candidates for breast cancer treatment, the guidelines say.
“We moved away from a one-size-fits-all approach to something that is more personalized or individualized,” said Dr. Kevin Oeffinger, director of the cancer survivorship program at Memorial Sloan-Kettering Cancer Center in New York and lead author of the guidelines.
The coming decade will see medicine become more tailored to a patient’s particular biology, genetics and environmental influences, Oeffinger said, and “this is a step in that direction.”
The new recommendations bring the American Cancer Society into closer alignment with the U.S. Preventive Services Task Force, an independent panel of experts convened by the federal Agency for Healthcare Research and Quality.
The task force touched off an emotional debate about mammograms with its 2009 recommendation that women at average risk for breast cancer be screened only once every two years, primarily between the ages of 50 and 74. Screening may begin at age 40 if women so choose after discussing the pros and cons with their doctors, it said.
“There is substantial agreement now,” said Dr. Albert Siu, who heads the task force. “Both of these guidelines indicate that the mammogram is a good test, although it’s not perfect.”
Nearly 232,000 American women will be diagnosed with breast cancer this year, and more than 40,000 will die of it, according to the National Cancer Institute. About 1 in 8 women will be diagnosed with the disease at some point in their lives, the NCI says.
Mammograms save lives by finding cancers that can be cured if caught at an early, treatable stage. But they also find tumors that are not destined to become dangerous if left alone, as well as tumors that can’t be stopped by surgery, radiation, chemotherapy or other drugs.
The problem is that lots of these tumors look the same on a mammogram, so doctors wind up treating them all. That leads to a certain amount of unnecessary care, which doctors call overtreatment.
Many recent studies have weighed the benefits of identifying dangerous but treatable cancers against the harm of overtreatment. In general, they have found that the younger the woman, the greater the chance that the benefits of early detection will be small while the harms of overtreatment will be large.
For instance, evidence from randomized clinical trials suggests that for women in their 40s and 50s, screening mammograms reduce the risk of dying of breast cancer by a modest 15%. That means 85% of the women in this age group who die of breast cancer would succumb to the disease regardless of whether they had a mammogram.
More mammograms also mean more false positives, which means women have to return for a second mammogram or perhaps a needle biopsy. Those additional tests can cause anxiety that should not be taken lightly, experts say.
Some women see all this as a good reason to cut back on mammograms. Other women would rather accept the risk of potentially unnecessary treatment to maximize the chance that a mammogram would make a lifesaving discovery. Both decisions are reasonable, Oeffinger said. In his own family, he said, he has one sister who is sticking with annual mammograms and one sister who has scaled back.
“We don’t want to make people feel wrong or guilty if they opt not to” get a mammogram every year, he said. “We support a woman going to a healthcare provider and having a discussion and making an informed decision.”
That type of thinking mirrors an overall shift in medicine toward tailoring care for each patient based on his or her values and needs, said Dr. Patricia Ganz, director of the Center for Cancer Prevention and Control Research at UCLA’s Jonsson Comprehensive Cancer Center.
“We can’t do cookie-cutter medicine,” she said.
The new guidelines are based on fresh information gleaned from studies of women who took different approaches to screening and were tracked to see how they fared. Earlier advice was based on randomized clinical trials — which are usually favored — but those trials were conducted 20 to 30 years ago with “outmoded technology,” Oeffinger said. (Randomized trials can’t be done today because mammograms have become the standard of care, and it would be unethical to ask women to skip them for the sake of a study.)
In a twist, the American Cancer Society opted to examine the data in five-year age increments instead of the usual 10.
“A lot happens in 10 years,” Oeffinger said.
What the experts realized was that when it comes to the risk of being diagnosed with breast cancer, the risk of dying of the disease and the degree to which mammograms help prevent those deaths, women between the ages of 45 and 49 have more in common with women in their early 50s than with women in their early 40s. That’s why annual mammograms should begin no later than age 45, Oeffinger said.
The value of annual mammograms dips around age 55, when menopause and other age-related factors cause breast cancer tumors to grow more slowly. Women who opt to be screened only once every two years can still get most of the benefit of annual mammograms while reducing their risk of false positives and overtreatment, Oeffinger said.
The most radical change in the new guidelines is that the American Cancer Society no longer recommends that doctors perform clinical breast exams on patients. Previously, the ACS endorsed the tests once every three years for women in their 20s and 30s, then annually from age 40 onward.
“There is simply no data to suggest that a breast exam by a healthcare provider, in addition to a mammogram, adds any benefit,” Oeffinger said. However, he added, “there is evidence that it increases the false-positive rate.”
Instead of spending five or six minutes checking for lumps, the ACS now advises doctors to use that time to talk with patients about when and how often to get a mammogram.
“We live in a zero-sum world,” he said. “If you have something you’re doing that hasn’t been shown to be beneficial, why not spend time talking about risk?”
Ganz and other oncologists said they were skeptical about this advice.
“If you’re doing a good physical exam, it’s pretty hard not to examine the breast,” she said.
Dr. Therese Bevers, medical director of the Cancer Prevention Center at the University of Texas MD Anderson Cancer Center in Houston, said this was just one reason why the new guidelines are “complicated and confusing.”
“If a woman wants to begin at age 40 and continue annually, there’s nothing in here that says they can’t,” said Bevers, who chairs the National Comprehensive Cancer Network’s guideline panel on breast cancer screening and diagnosis. That’s exactly what she and her colleagues at MD Anderson will continue to recommend to their patients — especially since women in their early 40s have more years of life to gain by averting a premature death, she said.
Rather than fight over the best age to begin screening or how often mammograms should be repeated, the medical community should focus more on making sure that all women have access to the life-saving test, Oeffinger said.
“Nearly 1 out of 3 women age 55 and over aren’t getting mammograms at all,” he said.
Improving the quality of mammogram readings also would benefit women more than arguing about which set of guidelines is best, Ganz said. In some countries, every mammogram is read by two radiologists who specialize in breast imaging; in the U.S., it may be read by a radiologist with no special training in breast imaging, she said.
On the whole, though, she praised the new guidelines for recognizing that mammograms are valuable but imperfect.
“Every woman who was diagnosed by a screening mammogram thinks it saved her life, and every woman who had a cancer missed thinks it was a rotten test,” Ganz said. “We have to be balanced and see that it’s one tool, and that we need better tools.”
Follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.
MORE FROM SCIENCE
Our ancestors were just as sleep-deprived as we are, scientists say
Study finds plastic debris and man-made fibers in fish sold in markets
Underwater fossils on shrunken Bahamian island hold key to Ice Age extinctions







