Zika’s link to Guillain-Barre syndrome revealed
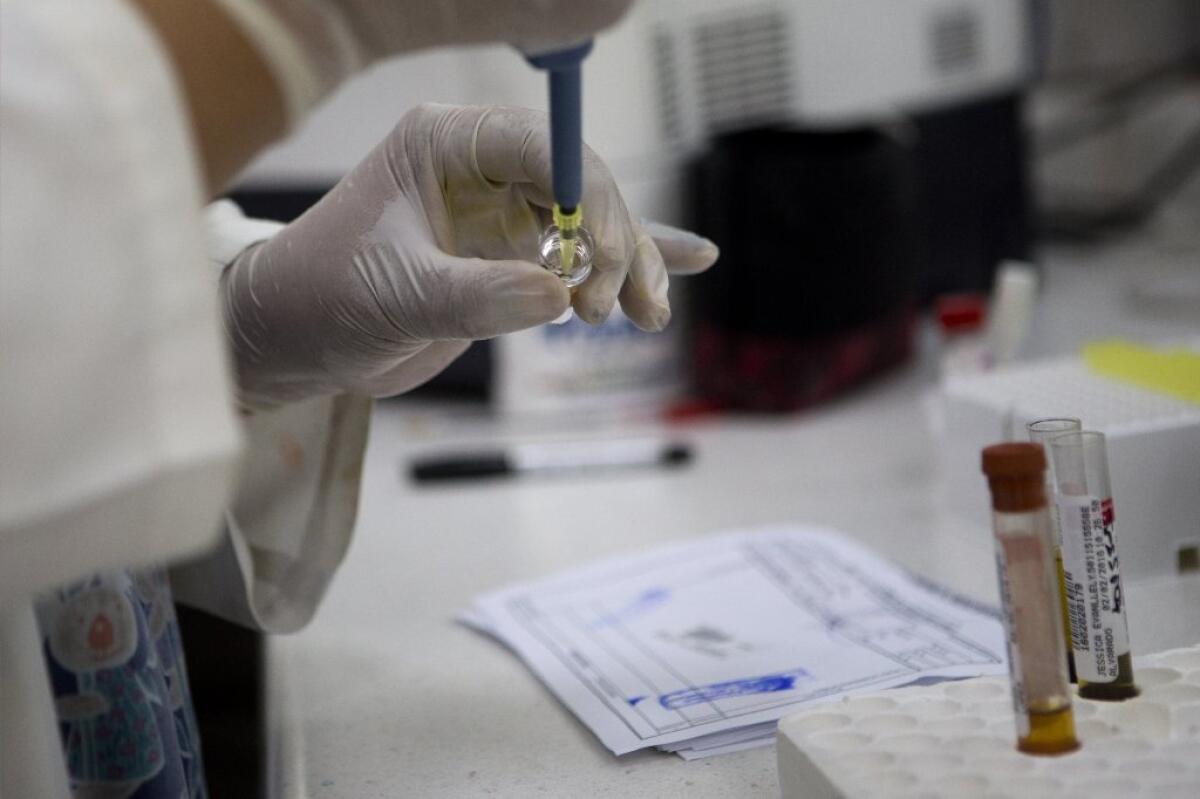
Scientists who went back to blood samples taken during a 2013-2014 outbreak of Zika virus in French Polynesia have found powerful evidence that it causes Guillain-Barre syndrome, a potentially fatal immune system attack on the nervous system.
- Share via
During a seven-month outbreak of Zika virus infection that ended in April 2014, health officials in French Polynesia noticed an uptick in the number of patients showing up at hospitals with a rare but dangerous constellation of symptoms known as Guillain-Barre syndrome.
Typically in the wake of a viral or bacterial infection, patients stricken with Guillain-Barre syndrome suffer a sudden onset of weakness, pain and paralysis in their legs and arms. Occasionally, paralysis progresses to the chest, impairing a patient’s ability to breathe. Even with access to a respirator and intensive care, some 5% of those stricken by Guillain-Barre die.
See the most-read stories in Science this hour >>
The mini-outbreak in that Pacific paradise offered the first ominous hint that the Zika virus is a pathogen capable of causing something more than just red eyes and a brief bout of muscle aches and fever. Just a year later, as it began to circulate across Brazil, came evidence that Zika virus is also linked to microcephaly in newborns exposed while in utero to the virus.
In French Polynesia, the numbers of those affected by Guillain-Barre syndrome have remained a matter of debate, as has the role of Zika-virus infection in causing the rare autoimmune reaction.
Until now.
A study published Monday in the journal Lancet has found substantial evidence that Zika virus infection and Guillain-Barre syndrome are causally linked. The study has also put public health authorities on notice that, as the Zika virus tears across the Americas infecting millions with no immunity, it is likely to claim adult lives and strain hospitals caring for the unlucky few who develop this post-infection complication.
During the Zika outbreak in French Polynesia, scientists estimate that 24 additional cases of Guillain-Barre syndrome would occur for every 100,000 people newly infected with Zika virus.
That’s a substantial increase in the rate at which Guillain-Barre Syndrome is normally seen. A rare response to infection with campylobacter bacteria, influenza or dengue virus, the cluster of symptoms collectively identified as Guillain-Barre syndrome is seen across Europe and North America in one to two of 100,000 people per year.
During the seven-month outbreak in French Polynesia, physicians at a hospital in Papeete, Tahiti diagnosed Guillain-Barre syndrome in 42 patients. To glean what role the Zika virus played in their afflictions, researchers based in France, Scotland and French Polynesia returned to the blood samples of those patients and compared them to two groups of otherwise similar patients in Papeete at the time: a group that entered the hospital with no fever, and a second group of patients who were confirmed to have been infected with Zika virus but who did not develop Guillain-Barre syndrome.
Nearly 9 of 10 of the patients who suffered Guillain-Barre syndrome reported symptoms consistent with Zika virus infection on average six days before seeking treatment at the hospital for their worsening symptoms of weakness, pain and paralysis. Blood tests confirmed that all had been exposed to Zika virus.
By contrast, just 54% of those who came to the hospital without fever had signs of a recent Zika infection.
A large majority of all the patients in the three comparison groups also had had past exposure to the dengue virus. But the presence of antibodies to the Zika virus as well was far more common in those who had Guillain-Barre syndrome.
Among the 42 Guillain-Barre sufferers who arrived at the Centre Hospitalier de Polynesie Francaise, none died. But 38% had to be admitted to the intensive care unit, and 12% required breathing assistance.
Ominously, the scientists deconstructing the French Polynesian outbreak of Zika concluded that the mechanism by which Zika prompts Guillain-Barre syndrome may be different from any seen before. Polynesian patients with Guillain-Barre all had damage to the nerves’ ability to conduct electrical signals, which is typically seen when the immune system attacks the nervous system. But only a few carried certain biological markers that are the hallmark of Guillain-Barre.
That could mean, at least, that Zika prompts the immune system to attack nerves by some other means than have been seen in past cases of Guillain-Barre, the authors wrote. It could also mean that Zika has some more direct role in damaging the nerves, they added.
Study coauthor Arnaud Fontanet of France’s Institut Pasteur said it’s not clear that Zika will leave the same trail of post-infection misery in its wake as it spreads across South and Central America as it did in Polynesia. But he said “high numbers of cases ... might be expected in the coming months” in those countries where Zika is spreading explosively.
“At-risk countries need to be prepared to have adequate intensive care beds capacity to manage patients with Guillain-Barre syndrome,” the authors of the latest study wrote.
Infectious disease epidemiologist Michael Osterholm said the new research offers “a stark warning” that Zika will tax hospitals’ intensive care units as well as pediatric and maternity wards in the coming months.
If the estimates drawn from French Polynesia prove to apply to South and Central America, said Osterholm, the current Zika outbreak could claim lives on a par with the Ebola virus in Africa.
Osterholm, who directs the University of Minnesota’s Center for Infectious Disease Research and Policy, said the new research also suggests that trouble may lie ahead in efforts to develop a Zika vaccine.
Because some vaccines can also prompt Guillain-Barre Syndrome, vaccine developers will need to be on the lookout for that complication as they test their candidates, he said. That will be complicated by the fact that Guillain-Barre is a very rare reaction to vaccines.
“You’re going to have to vaccinate lots and lots of people” to see the signal, Osterholm added.
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.
MORE SCIENCE NEWS
A view of the Milky Way like you’ve never seen before
Porter Ranch leak declared largest methane leak in U.S. history
Pregnant woman in L.A. County who traveled abroad tests positive for Zika virus




