Getting to the bottom of Zika’s link to microcephaly
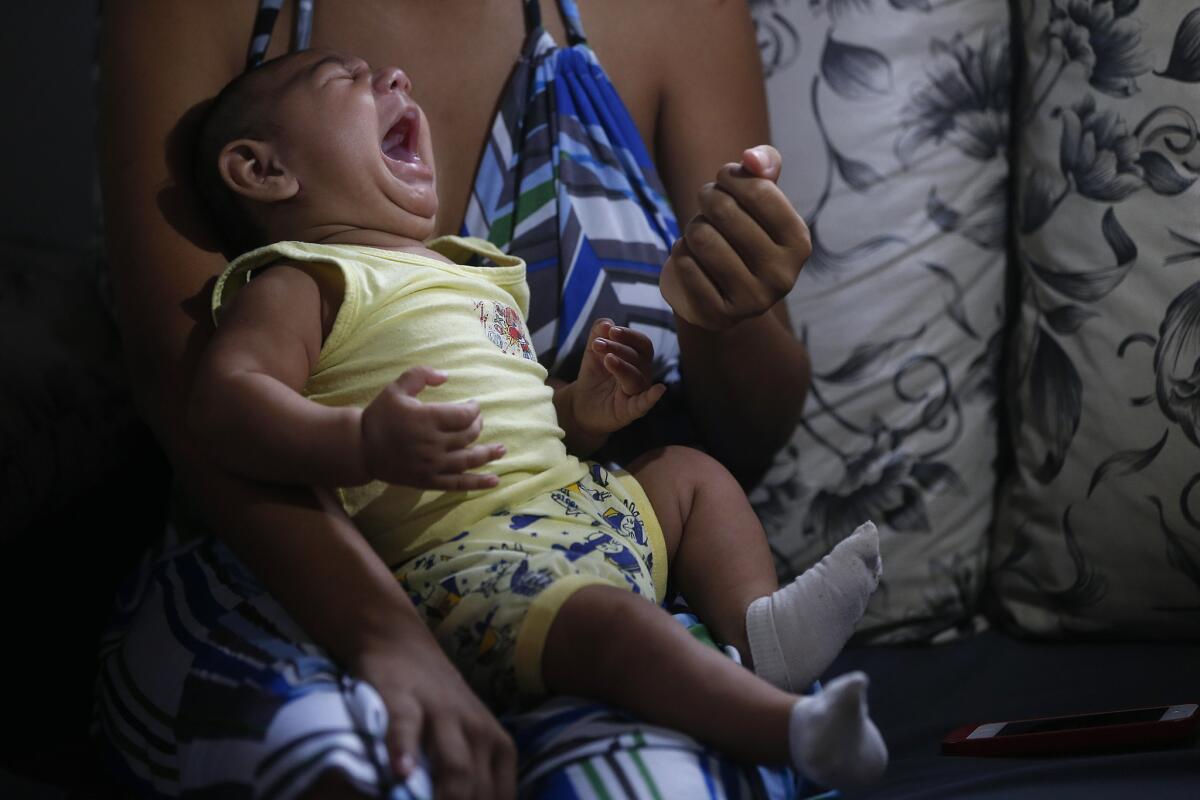
Janine Santos holds her 3-month-old son, who was born with microcephaly in Joao Pessoa, Brazil. U.S. and Brazilian health workers are enrolling mothers in a study aimed at determining whether the Zika virus really is causing a surge in birth defects.
- Share via
A killer is on the loose in the Americas, blamed for dozens of deaths and thousands of critical injuries. Officials have identified a prime suspect that appears to have the means, motive and mosquitoes to carry out its attacks.
The Zika virus has been indicted in Brazil and elsewhere for a mysterious spike in cases of microcephaly, a rare birth defect that can have devastating consequences. The circumstantial evidence is so compelling that Dr. Margaret Chan, head of the World Health Organization, called Zika a threat of “alarming proportions.”
Physicians are on heightened alert, pregnant women are in fear and public health officials are scrambling to contain the virus, which until recently had been considered more of a nuisance than a menace.
But if this were a murder investigation, prosecutors would still have a long way to go to prove that Zika is indeed guilty as charged.
“It’s entirely possible there’s something else going on in Brazil — something unique to the population or environment in which transmission takes place,” said Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases in Bethesda, Md.
It’s entirely possible there’s something else going on in Brazil — something unique to the population or environment in which transmission takes place.
— Dr. Anthony Fauci
There’s certainly good reason to put Zika on the most wanted list: Its fingerprints are at the scene of the crime. The virus was found inside the severely underdeveloped brain of a 29-week-old aborted fetus, according to a report this month in the New England Journal of Medicine. A subsequent study in the medical journal Lancet identified Zika in the amniotic fluid of infected pregnant women carrying microcephalic fetuses.
FULL COVERAGE: Zika virus outbreak
However, some babies born with microcephaly have no apparent link to Zika, and many women who believe they were infected during pregnancy have given birth to healthy babies.
Nailing down Zika’s precise role — if any — in these and other neurological disorders will require hard work by investigators from a wide range of scientific and medical disciplines.
“We’re pretty clear that Zika is causing this,” said Dr. Albert Ko, an infectious disease physician and epidemiologist at Yale University who is helping Brazilian health authorities investigate the outbreak. “But we need to firm those suspicions up.”
::
The virus now at the center of an international public health emergency was first identified in a rhesus monkey living in Uganda’s Zika Forest in 1947. Five years later, it turned up in people in Uganda and Tanzania.
Over the next three decades, the virus spread through equatorial Africa and into Pakistan, Indonesia, Malaysia and other parts of Asia. Even as its footprint grew, human infections remained mild and rare.

Pediatrician Alexia Harrist from the U.S. Centers for Disease Control and Prevention examines Angeline Karolayne in Joao Pessoa, Brazil. U.S. and Brazilian health workers knocked on doors in one of Brazil’s poorest neighborhoods in a bid to enroll mothers in a study of Zika’s possible role in causing birth defects.
Typical symptoms included a rash, red eyes, muscle aches and fever. They appeared to affect a minority of those infected, and they did not last long.
The virus was carried from its home base in Africa in the blood of mosquitoes in the Aedes genus. The insects pick it up by feeding on the blood of infected animals. The virus multiplies in the mosquito’s gut and migrates to the salivary glands, then spreads to a fresh victim when the mosquito takes another meal. (Read: How entomologists are putting Zika-spreading mosquitoses under the microscope.)
This is the same way Aedes mosquitoes spread other viruses, like the one that causes dengue fever. Up to 100 million people around the world become infected with dengue each year, and about 22,000 die as a result, according to the Centers for Disease Control and Prevention.
See the most-read stories in Science this hour >>
The first hint that Zika might pose an meaningful health threat came in 2007, when the virus took hold in the tiny Micronesian island nation of Yap.
Situated about halfway between the Philippines and Guam, the main Yap islands are home to about 7,500 people. In a four-month period in 2007, epidemiologists confirmed 49 active cases of Zika infection and identified another 59 cases of probable infection. Altogether, the experts estimated that between 68% and 88% of Yap citizens over the age of 2 had been infected with the virus, according to a 2009 report in the New England Journal of Medicine.
By 2013, Zika had spread to French Polynesia, where doctors confirmed 383 human cases. Altogether, researchers believe about 11% of the territory’s roughly 275,000 inhabitants were sickened by the virus during a seven-month period, according to the European Center for Disease Prevention and Control.
At the time of the outbreak, doctors identified 42 people who suffered Zika-like symptoms and went on to develop Guillain-Barré syndrome, a mysterious disease in which the immune system attacks the body’s peripheral nervous system. Patients feel tingling and weakness in the legs, arms and upper body; in extreme cases, it can lead to paralysis and become life-threatening. However, health authorities could not say whether the cases were caused by Zika — especially since dengue was circulating in the region at the same time.
Over the next year, local officials turned up a dozen cases of fetuses and infants with cerebral malformations typical of microcephaly, which often results in neurological problems and cognitive deficits. Although none of the women who carried these pregnancies had outward signs of Zika infections, four who were tested had antibodies to a Zika-type virus in their blood. The results suggested a link but were a long way from proving it.
::
Zika may have gained a foothold in Brazil as early as December 2014, when patients in the northeastern state of Pernambuco began reporting a mild skin rash. Similar patients appeared in nearby states in early 2015. By April, doctors reported nearly 7,000 such cases. Among patients who got blood tests, 13% had dengue, according to the WHO.
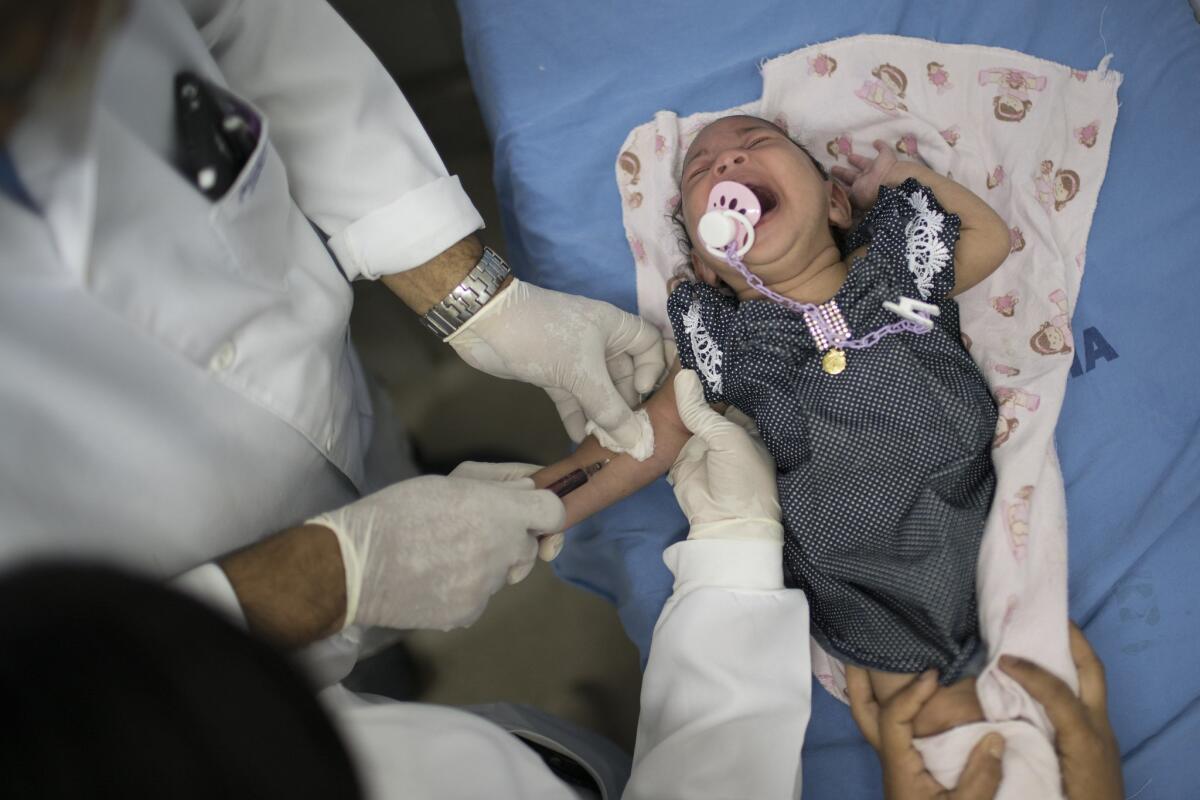
A doctor draws blood from Luana, who was born with microcephaly, at the Oswaldo Cruz Hospital in Recife, Brazil. Brazilian officials still say they believe there’s a sharp increase in cases of microcephaly and strongly suspect the Zika virus as the cause.
It took until April 29 for experts to realize that Zika was circulating in the region as well.
In July, officials confirmed 49 cases of Guillain-Barré in the area. Most of these patients had previously been infected with Zika, dengue or chikungunya. (Read: How epidemiologists are tracking Zika’s spread.)
In Salvador, Brazil’s third largest city, Dr. Manoel Sarno was among the first to report a sudden spike in microcephaly cases. In the space of two weeks in July, the maternal-fetal medicine specialist diagnosed 40 cases of microcephaly in developing fetuses or babies born to his patients. Normally, his practice would see five or six such babies in an entire year.
While the number of miscarriages has not been recorded, Sarno said he has seen a dramatic increase in these as well.
The surge was shocking, Sarno said, and its link to Zika was persuasive: fully 82% of these babies’ mothers recalled having had symptoms typical of Zika infection during their pregnancy, most during their first trimester. Questionnaires aimed at detecting other possible factors — such as alcohol consumption, socioeconomic status and medicines taken — found no other clear patterns, he said.
At least 4,443 suspected and confirmed cases of microcephaly have been tallied to date. Brazil has linked only 41 of those cases to laboratory-confirmed Zika infection in the mother, but the Health Ministry said it presumes most of the mothers of microcephalic babies were infected with the virus.
For now, there are no blood tests that can reliably confirm a past Zika infection. Even if there were, all it would provide epidemiologists is an association with microcephaly, not an explanation for it. (Read: How a diagnostic tool can help trace the spread of Zika.)
Many mothers of affected newborns may have been infected with other viruses in addition to Zika. Viral co-infections can sometimes have synergistic effects, a possibility that scientists will explore.
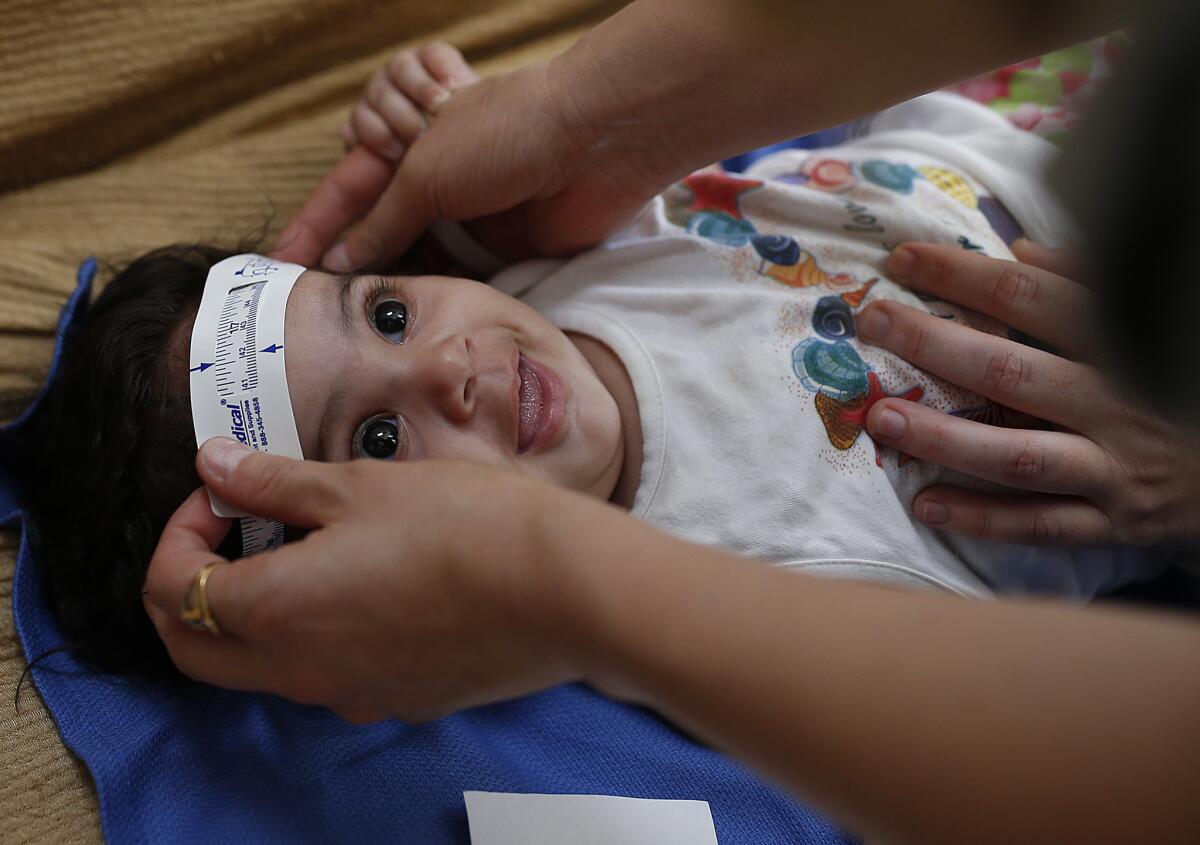
Three-month-old Esther Kamilly has her head measured by Brazilian and U.S. health workers from the U.S. Centers for Disease Control and Prevention at her home in Joao Pessoa, Brazil. The health workers are conducting a study to determine whether the Zika virus is causing babies to be born with a birth defect affecting the brain.
Health officials are also considering the possibility that an environmental toxin bears some responsibility for the microcephaly cases. The Brazilian state of Rio Grande do Sul recently suspended use of pyriproxyfen, a larvicide used to control mosquitoes that was introduced in 2014. Although that timing syncs up with the rise of microcephaly, scientists say the biological process pyriproxyfen disrupts in insects has no analog in humans, so it’s unlikely this particular pesticide played a role.
Another potential scenario is that Brazilian women are more likely to have a genetic variant that increases the risk of microcephaly when they contract Zika during pregnancy.
All of these could be the case, or none.
::
For now, epidemiologists have their hands full trying to nail down some basic facts.
To build a case against Zika, they need to know what the “background rate” of microcephaly in Brazilian babies was before the current spike, and how often those microcephaly cases were linked to infections that can cause birth defects, like cytomegalovirus, rubella and toxoplasmosis. (Read: Key riddles remain about how Zika might lead to microcephaly.)
They also need to know how many pregnant women must be infected with Zika to produce one microcephalic child, as well as the point during pregnancy when infection has to occur.
Another key piece of evidence is the number of microcephalic babies that are born to women with no history of Zika infection.
Unlike many countries now contending with Zika virus infection, Brazil has a well-functioning public health system. But officials there are still unsure how much of the spike in microcephaly is due to increased reporting by doctors and how many cases ought to be ascribed to other infections known to cause fetal brain abnormalities.
Until more evidence is in hand, there will be uncertainty as to whether, how often, and in whom Zika infection causes microcephaly.
“There’s so much that we don’t know, and that we need to know,” Ko said.
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.
MORE SCIENCE NEWS
Five ways scientists are going after the Zika virus
Earliest known medieval Muslim graves are discovered in France
How scientists solved the strange case of the missing asteroids







