Anxiety from a false-positive mammogram is real but temporary, study says
- Share via
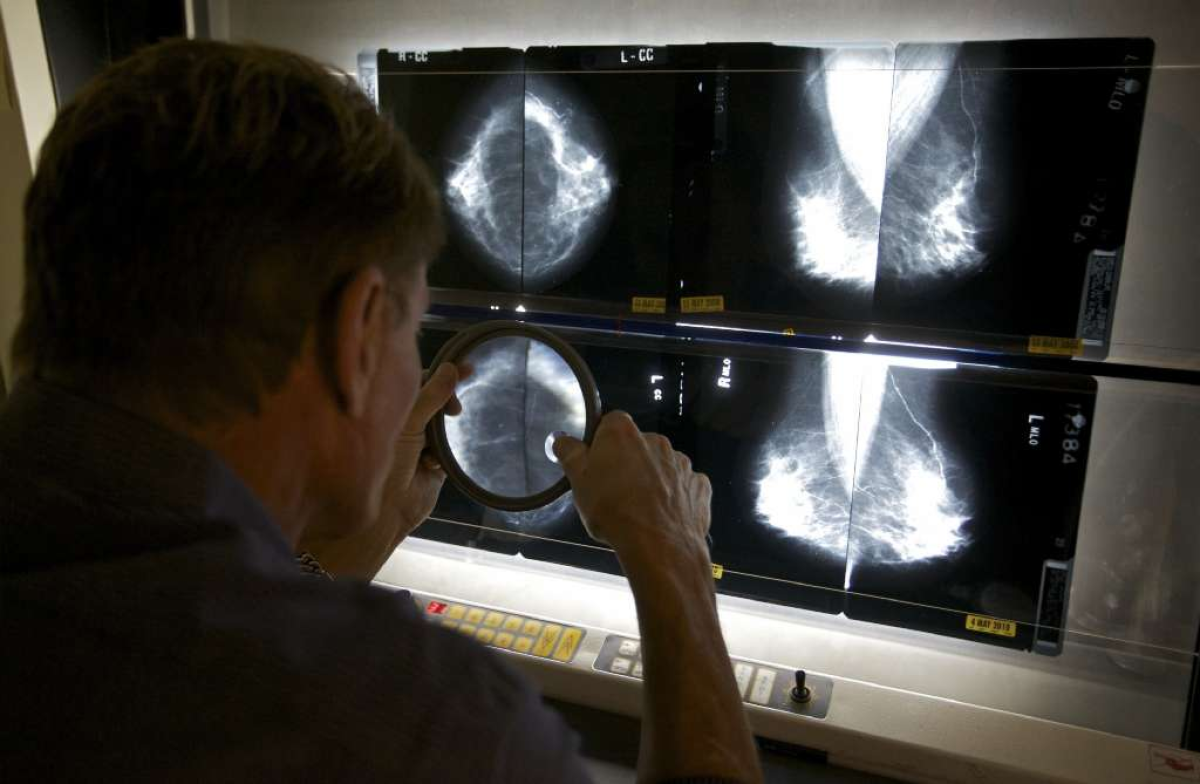
A healthy woman has a routine mammogram to check for signs of breast cancer, and the results aren’t normal. Her doctors run further tests, such as additional imaging or a biopsy. Ultimately, she gets a clean bill of health. But what is the emotional cost of this false-positive result?
This is the question that researchers try to answer in a study published online Monday by JAMA Internal Medicine. The authors examined data from a large clinical trial of digital mammography and concluded that false-positives produced a “significant increase in anxiety,” though it was only temporary.
The researchers focused on 1,028 women – 494 who had a false-positive reading on a mammogram and 534 others of similar age who were tested at the same medical centers but had clean results. None of women was diagnosed with breast cancer.
RELATED: Foods that affect your risk of cancer
All of the women in the study completed questionnaires to assess their general health in the previous four weeks and their anxiety level at the time of their interviews. (The researchers attempted to talk to the women during the period after they were told their initial mammogram was concerning but before they learned there was nothing to worry about. However, some women weren’t reached until after they knew they were out of the woods.) All of the women were also asked about their breast-related medical care in the year after their mammogram.
At baseline and again at their one-year follow-up, women in both groups rated their overall health highly – scoring an average of 0.90 on a scale that ranged from a low of -0.11 to a high of 1.0.
However, women in the false-positive group had higher levels of anxiety. On a scale from 20 (least anxious) to 80 (most anxious), the women who had false-positive mammograms and were interviewed before they had gotten their final results scored a 36, on average; those who were interviewed after they got the all-clear scored an average of 35. By comparison, the women with totally normal mammograms scored 33, on average. The difference for the women with false-positives was statistically significant (that is, too large to be due to chance).
After one year, the average anxiety score among all of the women with false-positive mammograms had dropped to 34, while the scores for the women with normal mammograms remained at 33, according to the study. Not surprisingly, women with false-positive mammograms had more breast-related medical treatment than women with normal mammograms. For instance, 14.6% of of those in the false-positive group had a biopsy, compared with only 1.1% of women with normal mammograms.
Researchers asked all of the women about their anxiety related to their follow-up care and found that 50.6% of those in the false-positive group reported “moderate,” “a lot,” or “extreme” anxiety. The corresponding figure for women with normal mammograms was 15.6%, according to the study.
A commentary that accompanies the study makes the case that the researchers’ choice of survey methods probably underestimated the true anxiety of the women who had false-positive test results.
In particular, neither the anxiety survey nor the overall health survey asked questions specifically related to breast cancer. Other studies that did were “more sensitive in detecting patient distress after mammography with false-positive results,” and they found that the distress lasted for up to three years, the commentary said.
Regardless of their personal anguish (or lack thereof), the overwhelming majority of women in both groups – about 93% – planned to have another mammogram in the next two years, according to the new report. About 60% of women in both groups said they would probably have moderate or worse anxiety if they got a false-positive result in the future. (The figure was slightly higher for those who already had a false-positive test, but the difference wasn’t big enough to be statistically significant.)
MORE: Medicines and machines, inspired by nature
Also, all of the women were highly motivated to avoid false-positive results in the future, with about 83% of women in both groups saying they would be willing to travel up to four hours to get a (hypothetical) advanced type of mammogram that was just as good at catching cancers but had a lower rate of false positives. What’s more, nearly as many women in both groups said if they could choose, they’d rather have a mammogram with fewer false-positives than a mammogram with less breast compression.
“Women are motivated to avoid false-positive mammograms,” concluded the researchers, who were from Dartmouth, the University of Wisconsin, Brown University, the University of North Carolina at Chapel Hill, UC Davis and the Medical University of South Carolina.
In light of this, clinicians must find better ways to talk with their patients about “the reality of false-positive mammograms,” wrote commentary author Dr. Kurt Kroenke of the U.S. Department of Veterans Affairs’ Center for Health Information and Communication in Indianapolis. That’s especially true for patients in their 40s – an age group for which the net benefit of screening mammograms depends greatly on how women feel about harms like anxiety, he wrote.
Other things he advised doctors to do to minimize anxiety for women included expediting their follow-up tests; make sure radiologists have access to a patient’s previous mammograms to improve the accuracy of their reads; and encourage women to get tested every other year instead of annually.
Over a 10-year period, the cumulative probability of getting at least one false-positive result on a screening mammogram is 61.3% for women who get tested annually and 41.6% for women who get tested every other year, Kroenke noted. As a result, a woman’s cumulative risk of getting a biopsy over that period is 7% for those who get annual mammograms and 4.8% for those who get screened every other year, he wrote.
[Updated at 10:02 a.m. PDT, April 22: The American College of Radiology sought to downplay the mental anguish associated with false-positives, reminding everyone that “anxiety regarding inconclusive test results is real and is only natural.” In a statement released Monday, the organization even suggested that by asking women to recall their anxiety, studies of this type could make things worse by prolonging whatever emotional pain they have.
“In terms of benefits vs. harms of breast cancer screening, short term anxiety regarding test results does not equate to dying from breast cancer,” the ACR said in its statement. “The proven benefits of breast cancer screening far outweigh any harm. According to National Cancer Institute data, since mammography screening became widespread in the mid-1980s, the U.S. breast cancer death rate, unchanged for the previous 50 years, has dropped more than 30 percent.”
While screening deserves much of the credit, many experts also attribute the sharp decline to improvements in breast cancer treatment during that period. That’s one of the reasons why the U.S. Preventive Services Task Force recommends that women at average risk for breast cancer continue to get screening mammograms, though less often.]
If you’re interested in the latest scientific and medical studies, you like the things I write about. Follow me on Twitter and “like” Los Angeles Times Science & Health on Facebook.







