Twice as many U.S. smokers should be screened for lung cancer, expert panel says
- Share via
A U.S. health panel wants to increase the number of Americans offered yearly scans for lung cancer by opening the screening to those who smoke less heavily.
Lung cancer is the nation’s top cancer killer, causing more than 135,000 deaths each year. Smoking is the chief cause and quitting the best protection.
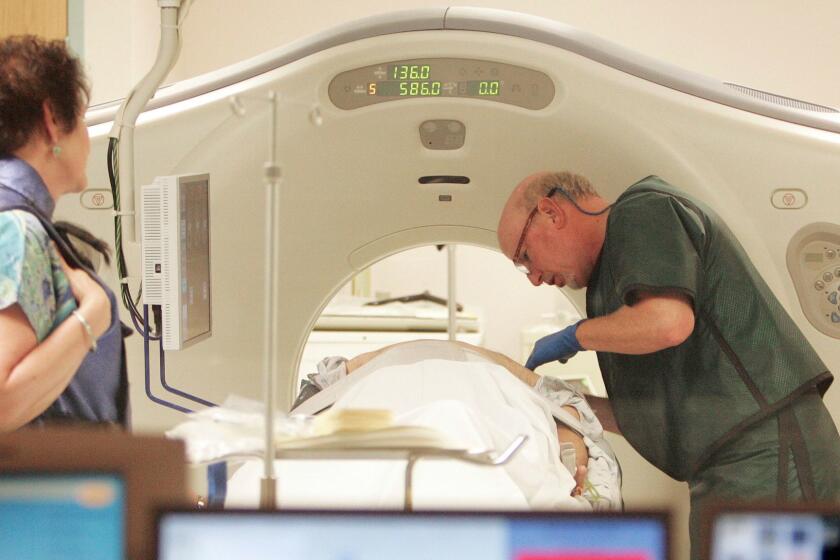
Usually, lung cancer is diagnosed too late for a good chance at survival. But research shows that annual low-dose CT scans, a type of X-ray, can reduce the risk of death when offered to certain people.
In 2013, the U.S. Preventive Services Task Force said current or former smokers who’d gone through a pack of cigarettes a day for 30 years, or an equivalent amount, qualified for the screening starting at age 55.
Now in draft recommendations released Tuesday, the task force says it’s time to expand screening to those who’ve smoked less — 20 pack-years — and to start a little sooner, at age 50. The proposed change comes after a newer study has found those people are about as likely to benefit as older people who smoke heavily.
If finalized, the new recommendations would make about 15 million Americans eligible for screening, nearly double today’s number, said task force member Dr. Michael Barry of Massachusetts General Hospital.
Importantly, more women and Black Americans would qualify, he said.
New research estimates that in a single year, some 5,000 lung cancer deaths might be averted if some former smokers who don’t currently qualify for lung-cancer screening were to get a computed tomography scan capable of detecting malignancy.
Lung cancer screening is complicated — not every hospital is equipped to offer it — and few of those eligible today receive it, just 6%, according to one study the task force cited. In contrast, 60% to 80% of those eligible for breast, colon or cervical cancer screening get checked.
One reason: When lung cancer screening finds an abnormality, people may need invasive testing to tell if it’s really a tumor. Occasionally, those lung biopsies can cause serious, even fatal, complications, said Dr. Otis Brawley of Johns Hopkins University, a cancer expert not involved with the task force.
Still, Brawley welcomed the expanded eligibility because younger smokers and those who smoke more lightly should have lungs in good enough shape to get the benefit of screening without as much risk.
“You’re recruiting healthier smokers, people who you’re more likely to be able to surgically intervene and do something,” he said. “They are moving toward a population where the bad things are less likely to happen.”
The proposal is open for public comment through Aug. 3. If finalized, the screening would be available to the expanded group of smokers without a co-pay, just as it is today for people who meet the criteria.