For face transplant recipients, some of the healing is psychological

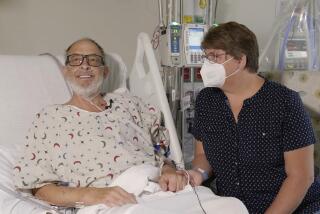
Richard Norris, right, shows friend Andrew Kahle how to load line into a fly fishing rod at Norris’ home in Hillsville, Va. Norris, whose face was disfigured by a gunshot, received a face transplant in 2012.
- Share via
What comes with a new face?
For roughly 30 patients across the globe who have received face transplants, the answer is both very simple and complex: A new face brings a measure of normalcy after years of living with the unrelenting social cataclysm of disfigurement.
For patients like Patrick Hardison, whose precedent-setting transplant was unveiled in New York this week, normalcy meant shopping at Macy’s without enduring the hushed remarks and quickly-averted stares of strangers. It meant touching his new chin and feeling sprouts of stubble for the first time in 14 years. It meant looking his teenage daughter in the eye, offering a familiar nod of reassurance, and wiping tears from his new face. It meant going to a sandwich shop with an old friend and wrapping his mouth around a gyro.
But a new face exacts certain costs as well, experts said this week. When physicians surgically attach a deceased donor’s skin and facial features to a recipient’s disfigured head, that patient takes on a lifelong risk that the new tissue, which powerfully attracts the immune system’s attention, will be attacked and rejected. A handful of patients have died after getting new faces.
Other burdens are far more subtle. In most cases, transplant recipients also feel a deep responsibility for a donor’s legacy. Sometimes this includes a relationship with a bereaved family.
“This is a huge psychological shift,” said medical ethicist Jennifer Blumenthal-Barby of Baylor College of Medicine in Houston, who has examined the ramifications of facial transplantation. Candidates for such surgery “have to be pretty psychologically robust to get through this,” she added.
What doesn’t come with a new face? An identity crisis, experts said.
“It’s not to say it won’t happen, but how these patients are going to integrate this new identity hasn’t been that big an issue,” said Dr. Mark Ehrenreich, a University of Maryland psychiatrist who was part of a facial transplantation team there in 2012. Scales that measure patients’ quality of life, self-image and social confidence “have shown people do remarkably better” after surgery than they did before, Ehrenreich added.
Given the central role that the face plays in forming a human being’s sense of self, that may come as a surprise. But Richard Lee Norris, the transplant recipient in that 2012 case, says it’s really pretty simple.
Norris explained that the obliteration of a person’s social identity comes with the trauma that necessitated the transplant in the first place. After that, he said, any face that doesn’t provoke stares provides identity enough for a person to build on.
“I went from looking really, really disfigured to looking normal again. I was immediately connected to my face,” said Norris, now 41 and a student living in New Orleans with his girlfriend.
When he looks at his face in the mirror, he said, “I see myself.”
Published case studies on transplant recipients suggest that only once has psychological rejection complicated the transplant of a prominent external feature. In 2001, hand transplant recipient Clint Hallam asked that his new hand be removed after failing to feel it was his own.
Transplant teams across the globe took a key lesson from the case of Hallam’s psychological rejection: that mental health professionals are an essential component of a transplant program.
Their role is particularly crucial in facial transplants, where trauma, social withdrawal and issues of identity play such a clear role. Psychiatrists, psychologists and social workers are key to selecting patients who are psychologically resilient. These mental health experts also help shape patients’ expectations and prepare them for a long and complex recovery.
Dr. Eduardo D. Rodriguez, whose team at New York University’s Langone Medical Center gave Hardison his new face, said last week that tending to his psychological health has been key to the procedure’s success.
“You can see he’s happy with it. It’s his face, as he says,” Rodriguez told reporters as he discussed the Mississippi firefighter whose original face essentially dissolved under a molten helmet in 2011.
“There are a lot of scars that we still have to deal with, and there’s a lot of anguish that we have to deal with, and we’re helping him,” Rodriguez said. “We’ll continue to support him.”
Like all transplant patients, Hardison can expect to spend the rest of his life on anti-rejection drugs to suppress his body’s natural response to his new face, which his immune system recognizes as foreign.
The medications come with an array of punishing side effects beyond the ever-present threat of infection. Transplant recipients face the lifelong prospect of anemia, arthritis, sleep difficulties, nausea, headache, tremors and mood swings, as well as weakened bones and the cardiovascular risk that comes with having high blood pressure and high cholesterol.
Those risks are not unique to people who get new faces: all solid organ recipients must take them. But they do pose a unique ethical quandary for people like Norris and Hardison.
Unlike patients for whom an organ transplant is a lifesaving necessity, no patient undergoing facial transplant would die without the surgery. On the contrary, Rodriguez said, candidates must be healthy enough to withstand a procedure that has resulted in death for at least four patients and, in Hardison’s case, required 26 hours under anesthesia.
For an essentially healthy patient to undertake the risk of both surgery and of a lifetime of anti-rejection drugs, “all of the procedure’s potential psychosocial benefits have to be weighed against these harms,” Blumenthal-Barby said. There’s also the risk that a new face won’t bring future happiness.
For Norris, the ethical conundrum was easy to resolve.
“It is a lifesaving operation, depending on how you define ‘living,’” said Norris, who became disfigured in a gun accident. “If you live as a recluse and deal with disgusting comments every day, that’s really not a life.”
NEWSLETTER: Get essential California headlines delivered daily >>
Finally, transplant recipients like Norris and Hardison become the stewards of a uniquely personal gift — the face of a person who has died. With that comes a remarkable responsibility and relationships unlike any other.
Hardison’s new face has forged a powerful psychological bond between him and a 26-year-old New York artist named David Rodebaugh, who was declared brain dead after a bicycle accident. In a video produced by Langone Medical Center, Hardison — speaking before Rodebaugh’s accident — expressed his faith that God had “an angel out there for me somewhere.”
“He’s going to call him home one day and hopefully when that day comes, that family is strong,” Hardison said in the video. “Because I cannot imagine losing somebody at a young age and then having to be asked to give what they’re asking them to give.”
Hardison’s prayers were answered when Rodebaugh’s mother, Nancy, agreed to allow her son’s face (as well as several of his organs) to be harvested for transplantation.
Later, she asked if Hardison’s family “is ready to have a grandmother in their lives.”
Ehrenreich, the psychiatrist, said that for some transplant recipients, such recognition forges not only gratitude, but “a bit of pressure to live up to what you’ve been given.” For patients that have struggled with trauma and depression, that can be a tall order.
For some transplant patients, the need to find meaning in a donor’s gift can prompt a remarkable search for kinship, Blumenthal-Barby said. She cited the common observation that transplant recipients take pains to find meaningful similarities with a donor. Many observe post-surgical changes that they attribute to the influence of the organ donor, such as a new interest or a sudden taste for certain foods.
“Medically, that doesn’t make sense,” Blumenthal-Barby said. But for patients, such changes may be a powerful acknowledgment of an obligation, and a way to honor it.
Maybe, she said, those impulses are “an expression of deep gratitude: to let that person live on in you, to maybe even change you a little bit.”
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.
ALSO
Why the FDA doesn’t want you to say ‘GMO’
NIH says it will retire all remaining research chimpanzees
Scientists spy two - or maybe three - planets in the process of being born