What urine reveals about obesity
- Share via
Let’s face it: Obesity’s not hard to diagnose. It’s easily done with a scale, a tape measure and (if you don’t want to do the math yourself), a body-mass index (BMI) calculator. Or you could go old-school, and use your eyes.
So, when scientists set out to explore “biomarkers” for obesity -- in this case, measurable chemical by-products in urine -- they had more in mind than finding an easier way to diagnose the condition. The undertaking was meant to glean insight on the links between obesity and the many ills that often come with it, from type-2 diabetes and heart disease to gall bladder disease and arthritis.
Better insight on those connections could lead to more effective prevention strategies, and to treatments that break the bonds between obesity and disease. A panel of obesity biomarkers might be able to identify people at risk of obesity, or to warn people who are thin that they are vulnerable to developing metabolic disorders or other diseases linked to obesity.
Their findings were published Wednesday in the journal Science Translational Medicine.
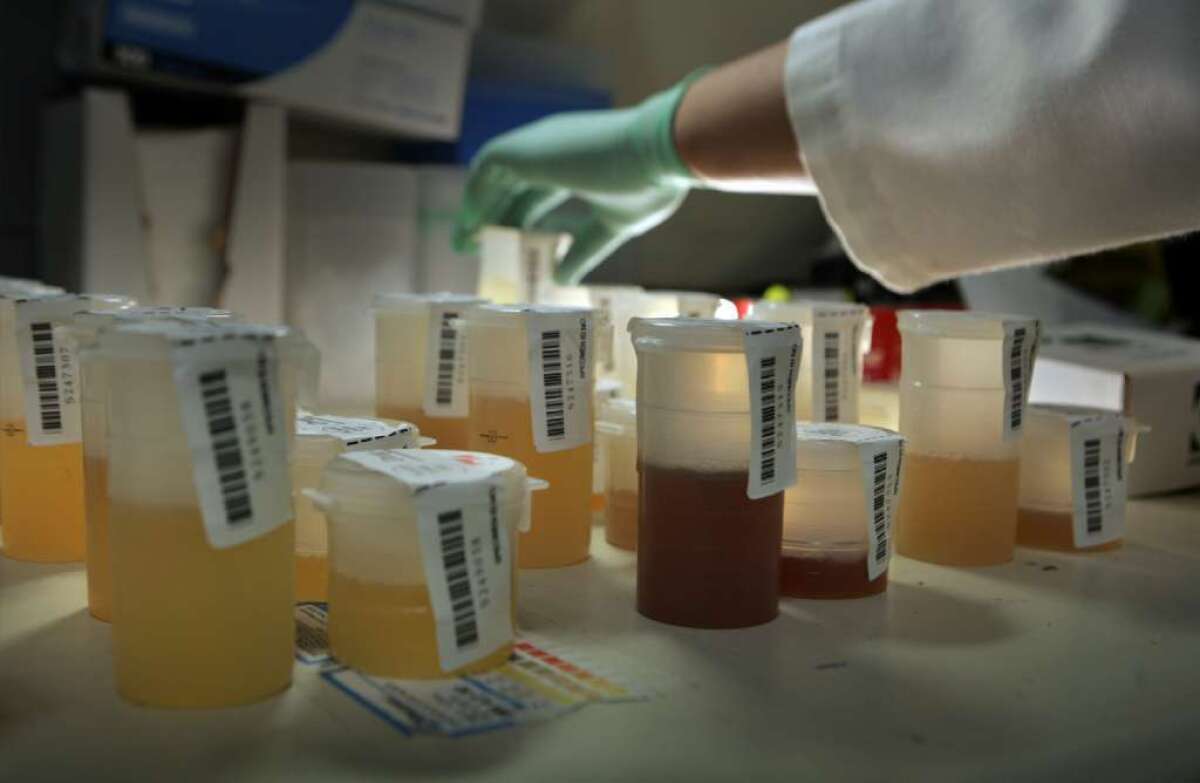
To glean that insight, researchers sifted through the urine samples of 2,195 men and women (ages 40 to 59) who ranged across the weight spectrum for the telltale metabolites of obesity. In all, they found 29 chemical metabolites -- the by-products of physiological processes that proceed unseen inside the body -- whose levels variously rose and fell with people’s BMI.
The result is a “network map” which could serve as a “metabolic signature” for the modern obesity epidemic, the authors said. To the uninitiated, the network map looks like an air traffic controller’s worst nightmare: a tangle of hundreds of chemicals that interact with one another in myriad ways. But to those devising ways to protect the obese from the health consequences of their condition, any of those overlapping nodes could contain the secret passageway to success.
Among the most notable metabolites they found linked to obesity were those produced by bacteria that colonize the gut, the latest in a flurry of research findings that implicate the gut’s microbiome to in obesity and metabolic disease. Other metabolites suggest that the skeletal muscle of obese people uses energy differently than does that of people of normal healthy weight.
“Our findings reveal multiple connections between many metabolic compartments and pathways,” the authors wrote, “and provide possible starting points for new approaches to prevention and treatment, for example, functional microbiome modulation and stimulation of skeletal muscle mitochondrial metabolism.”
Follow me on Twitter @LATMelissaHealy and “like” Los Angeles Times Science & Health on Facebook.


