Shaking Up Heart Therapy
- Share via
It doesn’t look like a good activity for someone with a bad heart.
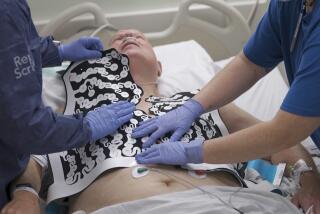
First, you’re strapped to a table, fitted into a pair of inflatable pants and wired up to an EKG machine. Then, for about an hour, every time your heart beats the pants inflate, squeezing your legs, shaking your body and making a lot of noise.
The procedure is called external counterpulsation (ECP) and is one of cardiology’s hottest, albeit unproved, new treatments. Proponents believe it may be a low-tech route to what was once believed impossible: stimulating the heart to grow new blood vessels.
“This therapy was laughed at by cardiologists for years. It’s like something out of a Rube Goldberg cartoon,” said Jarry Oken, chief of medicine at Howard County General Hospital in Maryland.
The treatment typically consists of 35 hourlong sessions, stretched over seven weeks. In 1999, Medicare decided to cover the procedure, and the number of people undergoing it has risen sharply. This year, about 4,000 people will have ECP, about double the number in 2000. The treatment costs $5,000 to $8,000, depending on who’s paying.
More than 200 sites now perform ECP. A setup costs about $200,000. Sales doubled last year at the manufacturer with the biggest market share, Vasomedical, of Westbury, N.Y., according to a company spokesman.
ECP’s intended for people with coronary heart disease who have exhausted conventional therapy: Bypass surgery has been done (or can’t be done), angioplasty isn’t possible and medicines aren’t enough to quell the chest pain.
To understand how it works, it helps to know a little about the mechanics of the heart.
Since the heart muscle is constantly working, it has a big demand for oxygen-rich blood. That comes from two vessels, the coronary arteries, which branch off the aorta immediately after that hose-sized vessel exits the heart.
Paradoxically, most of the blood flow into the coronaries occurs between beats, when the heart is relaxed. During that pause--it lasts less than one second--the aorta, which is literally bulging with blood, relaxes, and in so doing propels blood into the arbor of branches coming off it.
ECP increases coronary blood flow by raising the pressure in the aorta during the pause between beats. At the instant the pause begins, the pneumatic pants inflate--first around the calves, then the thighs, then the buttocks. At the instant the heart starts to contract, the pants deflate.
The procedure squeezes more blood into the coronary arteries. This makes many people with coronary artery disease feel better, but it apparently does more than that. The higher pressure--about twice the normal level between beats--appears to initiate a cascade of changes in the cells lining the coronary arteries.
The changes are similar to what happens with aggressive physical training, and in fact ECP may be the closest thing to passive exercise. One of the results is increased secretion of vascular endothelial growth factor (VEGF), a hormone that stimulates blood vessel growth, or angiogenesis.
Whatever it is, Barbara Mendenhall thinks it works.
Mendenhall, 65, is a retired teacher in Columbia, Md., whose coronary artery disease isn’t amenable to surgery. Midway through a treatment--four one-hour sessions a week, for seven weeks--she proclaimed ECP a success.
“I’m not as tired,” she said. “Whereas before I could only do one strenuous thing a day, now I can do two or three. I just feel better.”
She spoke over a relentless sound of chuff-poof, chuff-poof as the air bladders in the ECP pants inflated and deflated. Every round shook her body. When she laughed and her pulse rate sped up, so did the pants. The effect, originally scary and disconcerting, no longer bothers her.
“I look like I’m in a straitjacket, but I’m really quite comfortable,” she said. “Sometimes I go to sleep.”
Oken cites a case from 2000 demonstrating another application of the therapy.
A 61-year-old man who’d had two bypass operations and several angioplasties still experienced chest pain. During tests the doctors saw a coronary vessel that could potentially be widened with angioplasty. However, there wasn’t an adequate “collateral” system of blood vessels that could feed the heart muscle if a calamity occurred and angioplasty closed off the vessel rather than opened it.
Oken advised against the procedure, and suggested the man try ECP instead. He got two seven-week courses. The therapy reduced but didn’t eliminate his chest pain.
The growth of new collateral blood vessels was dramatic, Oken said. The risks of angioplasty seemed reasonable after the ECP therapy, and the man underwent the procedure. Now, he walks two miles a day, and though he occasionally gets chest pain with extreme exertion, he feels far better.
Many such anecdotes surround ECP. Proving that the therapy stimulates vessel growth is another matter. Only one randomized controlled trial--the best way to judge effectiveness--has been done. It showed that people getting a 35-session course of ECP were able to exercise longer, and had fewer episodes of chest pain, than people who got a “sham,” or fake, form of the procedure. The study didn’t examine patients for signs of angiogenesis.