Idea of Paying Blood Donors Gains
- Share via
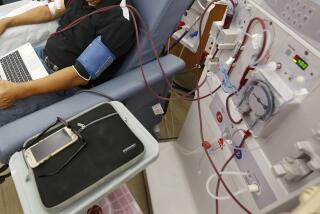
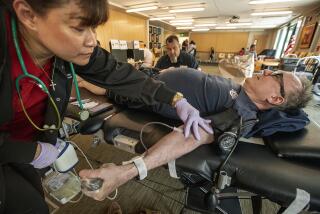
A sustained national blood shortage is forcing some hospitals and blood banks to ask: Should we pay our blood donors?
A minority of blood bankers and doctors see “donor incentive programs” as the most practical response to dwindling blood supplies. Even some longtime supporters of the American Red Cross, which is adamantly opposed to paying donors, are raising the possibility.
“In order to provide an adequate blood supply, this modest incentive might make it worth people’s while to come in and donate,” said Dr. Janice Nelson, a board member for a regional branch of the Red Cross and director of the Los Angeles County-USC Medical Center Blood Bank.
“Now that we’re seeing the shortages and increased demands, I think it’s one thing that we’ve got to look at--the money.”
Many ethicists and health officials blanch at the prospect, saying it could compromise the safety of the blood supply. Citing medical research on the question, they argue that paying donors would encourage them to lie about their medical or behavioral history, making it more likely for infectious diseases to enter the supply.
“The safest blood donor is the volunteer donor that donates for altruistic reasons,” said Jackie Fredrick, a senior vice president with the American Red Cross.
Proponents of for-pay programs counter that today’s blood testing is so advanced--screening for everything from hepatitis to HIV--that the blood supply would not be compromised.
These proponents say donors now get “incentives” one way or another, be it paid time off work, tickets to cultural events or smaller gifts, such as ice cream coupons.
“The definition of ‘paid’ is very imprecise and frankly unscientific,” said Dr. Ron Strauss, medical director of the DeGowin Blood Center at the University of Iowa. “How one cash is OK and how one cash is not OK doesn’t make any sense to me.”
The Food and Drug Administration defines “paid” as anything readily transferable to cash. The agency requires that paid donations be labeled as such.
Some experts fear that viruses and infectious diseases yet undetected could creep into the blood supply just as HIV did in the early 1980s. Meanwhile, they say, keeping an all-volunteer donor pool provides an extra layer of safety.
“Clearly, the experience with the AIDS epidemic has created an environment in which . . . blood bankers tend to bend way over backward to do almost anything they can think of to improve the safety [of the blood supply],” said Dr. Jeffrey C. McCullough, editor of Transfusion magazine and professor of laboratory medicine at the University of Minnesota.
It is almost unheard of in the United States for blood banks to pay donors for red blood cells--but several agencies, including the blood center at the University Iowa; the Mayo Clinic in Rochester, Minn.; and Sherman Oaks-based HemaCare Corp., say they have safe and successful paid-donor programs for platelets, the cells that cause blood clotting.
Part of the argument for compensating platelet donors is that the donation process is much more arduous and time-consuming than for red blood cells, and that the platelet shortage is even more severe.
In California, a debate has erupted over the HemaCare for-pay platelet program. The small for-profit company is seeking a permanent exemption from a state law that bans for-pay blood donations. The Red Cross and all other blood banks in the state are adamantly opposed.
HemaCare, which supplies about 30% of Southern California’s platelets, pays $50 for each platelet donation gathered from its pool of 550 donors. Company officials point out that not a single infectious disease has been transmitted from its paid platelet donor program in its 22-year history.
Legislators say last year’s Assembly Health Committee hearings on the topic were heated and emotional, for both the lobbyists and the lawmakers. Ultimately, the Legislature allowed HemaCare to continue paying platelet donors until December 2002 and deferred action on a permanent exemption.
Assemblywoman Helen Thomson (D-Davis), who sat on the Health Committee and is now its chair, voted in favor of allowing for-pay platelet programs. For now, HemaCare’s is the only one in the state.
“I find it a little frustrating that the blood banks would so actively oppose the payment for platelet collection and say that all blood products ought to be voluntary when we have a problem in California of getting enough blood voluntarily, and secondly, when they themselves offer prizes and tickets and T-shirts for providing blood,” Thomson said.
HemaCare vows to keep fighting, but if its lobbying efforts do not produce a successful bill next year, its operation will likely be shut down.
While the debate rages on, experts in the blood industry are struggling to find a middle ground. McCullough, who once held a senior vice presidency with the Red Cross, sees both sides of the issue.
As the shortage worsens, he said, “You could maybe visualize a point where you . . . determine that the the risks of not having the blood are greater than the risks associated with changing the system.”
At the very least, McCullough said, the idea should be aired. “There hasn’t been a thoughtful open discussion about this for decades, and I think it would be useful.”
*
Times health writer Charles Ornstein contributed to this story.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.