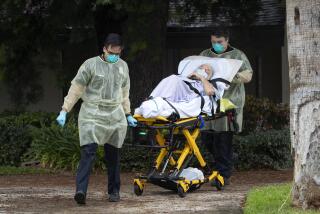
U.S. Joins Probe of Nursing Home Deaths
- Share via
WASHINGTON — Federal investigators have joined a Louisiana inquiry into nursing home deaths during Hurricane Katrina, as the government begins considering stronger requirements to protect patients in healthcare facilities during natural disasters.
Industry officials say the deaths were tragic exceptions in chaotic circumstances under which most facilities carried out their duties, some of them heroically.
The inspector general’s office in the Department of Health and Human Services said it was assisting the investigation of 34 deaths at St. Rita’s Nursing Home in St. Bernard Parish. State authorities have charged the owners of the home with 34 counts of negligent homicide for allegedly ignoring requests to evacuate.
“This office is tremendously concerned about the possible abuse and neglect of hospital patients and nursing home residents,” Inspector General Daniel R. Levinson wrote to Sen. Charles E. Grassley (R-Iowa) in a letter released Thursday. Grassley has also asked for a Justice Department investigation.
Separately, officials of Health and Human Services -- which, through Medicare and Medicaid, is the nation’s largest payer for hospital and nursing home care -- said they would consider a broad range of actions to prevent such deaths in the future.
“I think only Rip Van Winkle would be able to ignore the wake-up call that Hurricane Katrina offers with regard to emergency preparedness,” Thomas Hamilton, director of the department’s office that sets standards for healthcare facilities, said in an interview.
“It is worth looking at the current requirements and asking ourselves, in light of the experience with Hurricane Katrina, with an entire healthcare system going down: Are there better protections that could be put in place for that kind of phenomenon?”
Responsibility for oversight of healthcare facilities is shared by state and federal agencies as well as independent professional organizations that issue accreditation. Washington generally plays a secondary role to state regulators.
In the St. Rita’s inquiry, federal investigators will be examining whether the nursing home fulfilled its duty under Medicaid regulations. Possible penalties include barring the owners from billing Medicaid and Medicare, which is tantamount to exile from the healthcare marketplace.
Federal regulations require nursing homes to have an evacuation plan tailored to local conditions, to train their staffs and to periodically practice the plan. Nursing homes say they often have to bear the cost of the evacuations themselves, which can run into tens of thousands of dollars. But the government says that many have insurance to cover such situations, and that Medicare also helps pay ambulance costs for residents.
The department’s review will be broad, Hamilton said. Prior to Katrina, disaster plans did not generally envision the prolonged collapse of a community’s public service infrastructure. Hospitals did not count on being marooned for days with no effective way to call for help.
“Emergency communications is clearly one of the areas that requires improvement,” Hamilton said.
“The weakness of many emergency plans is the assumption that communications will still be in place.”
Other areas that the department will examine include mutual support plans among healthcare facilities, and ways to ensure that evacuation plans and other protective measures are carried out in an emergency, Hamilton said.
The nursing home industry said it supported the government’s efforts to investigate what went wrong in New Orleans, but officials said most facilities met and even exceeded their responsibilities.
“We had a number of caregivers who lost everything, but stayed with their facility when it evacuated and kept caring for patients,” said Donna Doneski, spokeswoman for the American Health Care Assn., which represents for-profit homes.
“We are as eager as everybody else to see what the facts are in these cases,” said Lauren Shaham of the American Assn. of Homes and Services for the Aging, which represents nonprofit homes.
Shaham said most of her group’s members in the New Orleans area had evacuation agreements with nursing homes out of Katrina’s path. She said one owner wrote a check for $28,000 to a hotel until he found a home that could take his patients. Another home paid $25,000 to evacuate 171 people on buses.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.