Down syndrome screening advised for all pregnancies
- Share via
All pregnant women, regardless of their age, should be offered screening for Down syndrome in their first trimester, according to new practice guidelines issued today by the American College of Obstetricians and Gynecologists.
Noninvasive screening tests developed over the last decade have made it possible to predict the risk of Down syndrome and certain other chromosomal abnormalities with high accuracy.
Those identified as being at risk can then be offered further screening with invasive, and more dangerous, tests such as amniocentesis or chorionic villus sampling, according to the guidelines published in the January issue of the journal Obstetrics & Gynecology.
Invasive tests have previously been offered routinely to women older than 35, who are at the highest risk of bearing affected children. But the risks in older women have been managed so successfully that the largest number of Down syndrome children are now being born to younger women, according to Dr. Edward McCabe of the Mattel Children’s Hospital at UCLA.
The committee that wrote the guidelines recognized “that counseling has been much more effective in the older group, and now it is important to begin looking at younger women,” he said.
The guidelines are already followed in most academic centers, but not in many private practices, especially in those that are small and in rural areas, said Dr. Gautam Chaudhuri, executive chair of the obstetrics department at UCLA’s Geffen School of Medicine.
Down syndrome is caused by the presence of an extra copy of chromosome 21 and is characterized by congenital heart defects and mental retardation.
The risk is low -- about one case for every 1,300 births -- in young women, then increases sharply to one in 350 births beyond age 35 and one in 25 beyond age 45.
The original rationale for screening only older women was that the invasive tests could be dangerous for the fetus, leading to one death in about every 200 examinations. That risk has declined over the last decade, but many women still prefer to avoid it unless there is reason to believe the Down risk is higher, said Dr. Nancy Green, medical director of the March of Dimes, which is focused on preventing birth defects.
Beginning in the 1990s, obstetricians began using assays for three chemicals -- alpha-fetoprotein, unconjugated estriol and human chorionic gonadotropin -- in the mother’s blood stream during the first trimester. This so-called triple test identifies about 70% of Down cases.
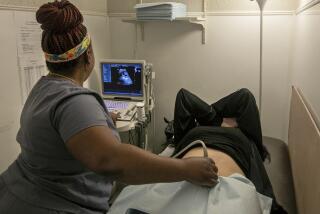
A major breakthrough occurred at the end of the decade with the recognition that an accumulation of fluid in the fetus’ neck is associated with a broad range of chromosomal abnormalities, including Down syndrome. This nuchal translucency can be readily measured by ultrasound.
Major trials in both the United States and the United Kingdom have recently shown that adding ultra sonography for nuchal translucency to the triple test raises the detection rate above 90%.
The new guidelines thus call for all women to be offered a combination of blood and nuchal translucency tests during the first trimester. Those who test positive should then be offered either amniocentesis or chorionic villus sampling during the second trimester.
Appropriate counseling should be offered in all cases, according to the guidelines.
The primary limitation to the guidelines is that many technicians who carry out ultrasound exams have not yet been trained to perform nuchal translucency studies.
To overcome that, the Society for Maternal-Fetal Medicine is organizing training programs to teach the procedure to technicians.