The next step in fetal diagnosis
- Share via
Within a few years, a pregnant woman may be able to have a simple blood test to determine whether the child she is carrying is afflicted with a number of serious genetic disorders -- Down syndrome, cystic fibrosis and Tay-Sachs disease among them.
Three studies published or presented this month demonstrate how fetal DNA can be isolated from the mother’s blood and checked for genetic abnormalities. A test based on such technology eventually could replace amniocentesis and chorionic villus sampling -- invasive tests that examine fetal DNA but carry a small risk of miscarriage.
Such a test could also ignite new research into how some disorders might be treated in utero, says Dr. Kenneth Moise, a professor of obstetrics and gynecology at Baylor College of Medicine in Houston.
“This is a new age of being able to diagnose fetal genetic problems by doing a blood test of the mother,” he says. “The beauty of this whole thing is we can do it at eight to 10 weeks of pregnancy.”
Researchers have long known that fetal cells circulate in a mother’s blood, and scientists have tried vigorously to develop a prenatal genetic test by isolating those cells. However, the fetal cells are so scarce, Moise says, that “it was like looking for a needle in a haystack.”
Moreover, because such cells can remain in a mother’s blood for many years, doctors couldn’t be sure if the cells were from the fetus or an earlier pregnancy.
About 10 years ago, however, new studies revealed that fetal DNA -- packets of genetic code from a developing fetus but not whole fetal cells -- could also be found in a pregnant woman’s blood. The discovery of this material, called free fetal DNA, launched new efforts to isolate the genetic material.
Meanwhile, the ability to analyze fetal DNA was boosted by knowledge gleaned from the human genome project, an effort to map the human genetic code.
As a result of these advances, scientists can now run tests to search for single nucleotide polymorphisms, tiny variations in the DNA sequence that can be used to distinguish a woman’s DNA from that of the fetus.
In research presented last week at the annual meeting of the Society for Maternal-Fetal Medicine, researchers at a San Diego company called Sequenom Inc. showed they can routinely detect fetal DNA in a pregnant woman’s blood in the first trimester.
This month, researchers published a paper in the Lancet detailing a technique to detect Down syndrome using maternal blood. The test was accurate in 58 of 60 cases. One case of Down syndrome was not identified, and one normal sample was incorrectly identified.
“The purpose of our study was to prove this technology can work,” says Dr. Ravinder Dhallan, chairman and chief executive of Ravgen Inc., a Columbia, Md., firm working on a noninvasive test.
And in a study published this month in Nature Medicine, scientists from the Chinese University of Hong Kong used the Sequenom technology to correctly diagnose Down syndrome in nine of 10 samples. Among 57 women carrying normal fetuses, two samples were misidentified as abnormal.
The technology has not been perfected, but preliminary research published this month suggests that the noninvasive blood test for Down syndrome could detect it with accuracy similar to the screening tests now offered.
How screenings work now
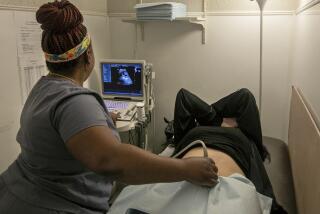
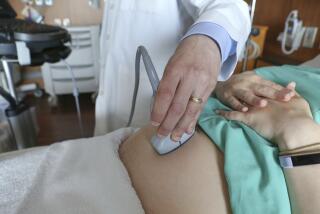
Currently, pregnant women can undergo Down syndrome screening during the first trimester with an ultrasound exam and a blood test to measure specific maternal hormones associated with Down syndrome. Screening tests do not diagnose a disorder but indicate a high risk for it. The current combination of blood test and ultrasound produces a 5% rate of false positive results -- meaning the test suggests Down syndrome when the disorder is not actually present. The test misses about 10% of Down syndrome cases.
If the screening is positive, the pregnant woman is offered the option of having amniocentesis or chorionic villus sampling, both of which use needles inserted into the womb to extract fetal DNA for analysis. These tests are considered nearly 100% accurate. But about one in every 200 to 500 patients will suffer a miscarriage.
“Even with a 5% false-positive rate, that’s about 150,000 women in the United States who are told they have a positive result,” Dhallan says. “That creates a fair amount of panic in patients. They are faced with a very real but scary decision about whether they should have invasive testing.”
None of the noninvasive techniques for detecting Down syndrome -- the condition for which invasive tests are most commonly performed -- are near 100% accurate, which will be required if a blood test is to replace invasive tests.
But within three to five years, by most estimates, the technology could emerge as a screening test for the condition. And, as accuracy improves, it could become the standard method to diagnose Down syndrome and other fetal disorders.
“The requirement, of course, is that the noninvasive test is as accurate as the one that is invasive,” says Dr. Michael Katz, senior vice president for research and global programs at the March of Dimes. “Definitely, this is promising.”
Detecting Rh disease
Sequenom plans to introduce a maternal blood test this year that would detect Rhesus, or Rh, disease in the fetus. Rh disease occurs when the mother’s blood is incompatible with that of her fetus. Babies with Rh disease can be stillborn or suffer serious health consequences, such as anemia. Women at risk for having an Rh baby often undergo amniocentesis to determine the baby’s blood type.
Leslie Williamson, 38, is pregnant with her fourth child and has had amniocentesis 20 times to monitor her babies for Rh disease.
“I tell people, I’ve done amniocentesis so many times I probably could do my own,” says Williamson, of Temple, Texas. “But each time I was so scared.”
The blood test would analyze fetal blood type before amniocentesis or any treatment for Rh disease is required, says Moise, a consultant for Sequenom. Eventually, a blood test should suffice to diagnose any number of genetic disorders such as congenital adrenal hyperplasia, a genetic defect of the adrenal glands affecting the production of critical hormones; beta thalassemia, which causes severe anemia; muscular dystrophy and others. The goal, many researchers say, is to identify disorders early and devise methods to treat the baby in utero.
“Early diagnosis is the key to advancing treatments for genetic disorders,” says Harry Stylli, president and chief executive of Sequenom. “Without early tests, it’s difficult to develop any treatment.”