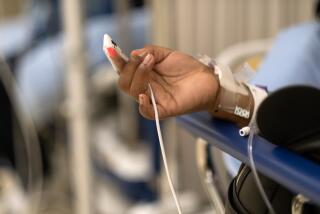
British hospitals struggle to contain deadly infections
- Share via
LONDON — British health authorities have blamed the deaths of at least 90 people on a virulent bacterial infection that swept through three hospitals in south-central England, where patients allegedly were forced to defecate in their beds and wait for hours for clean sheets.
In one of the worst of a growing number of hospital infection outbreaks in Europe, an additional 255 deaths were partially linked to Clostridium difficile bacterium, which is resistant to many disinfectants and can become more deadly if patients are treated with the wrong antibiotics.
Britain has been reeling over the last year with reports of more than 6,300 hospital-based “superbug” infections at its government-run National Health Service facilities. Those cases of Staphylococcus, or staph, infections that are resistant to common antibiotics appear to be leveling off, while the number of C. difficile cases rose by 7% in 2006, to 56,000.
An intestinal bacterium capable of causing fatal diarrhea, C. difficile is worrisome because it can form spores that are difficult to eradicate with all but the most stringent cleaning.
Patients who are prescribed broad-based antibiotics by doctors unaware of their exposure to C. difficile often fall victim to rapidly worsening infection because the bacterium flourishes as competing bacteria in the intestines die.
Prime Minister Gordon Brown last month said Britain’s hospitals would be cleaned “a ward at a time: walls, ceilings, fittings and ventilation shafts . . . disinfected and scrubbed clean.” This week, the government pledged $280 million to help combat C. difficile and $260 million to screen incoming hospital patients for the drug-resistant staph known as MRSA.
Health investigators and patients said the hospitals in the study were beset by nursing shortages. Beds were jammed within a foot of each other, and the administration was preoccupied with meeting budget targets, patients reported.
The daughter of an 87-year-old war veteran who died after being left with soiled sheets and bedsores said her father told her: “What have I done to deserve a place like this?”
“They were taking three hours to change his sheets,” Jackie Nixon, whose complaints helped initiate the commission review, said in a telephone interview.
Hospital officials said they were implementing strict anti-infection procedures, including a $2-million cleaning program and new policies on hygiene and antibiotic use.
“We are very sorry about what happened, and we are determined to continue to reduce levels of the infection locally,” Dr. Malcolm Stewart, the hospital’s medical director, said in a statement. “Our rates [of infection] have dropped dramatically . . . as the result of hard work by our staff.”
Britain’s National Health Service last year had a budget deficit of nearly $1 billion and faced the potential of thousands of layoffs across a system that serves 10 million hospital patients a year.
C. difficile has been linked to outbreaks in Belgium, France, Germany, the Netherlands and Ireland, as well as in North America, but Britain appears to have the largest number of cases, health officials said.
“In most of these [other] countries, they’ve managed to contain it fairly well, but in the U.K., it seems not to have been recognized early enough,” said Ben Duncan, spokesman for the European Center for Disease Prevention and Control in Sweden.
Investigators from the Commission for Healthcare Audit and Inspection, which looked at three state-run hospitals in Kent and Sussex between 2004 and 2006, found that inadequate hygiene, improper use of antibiotics and crowded conditions contributed to the fatalities, among the highest on record.
Whereas C. difficile was “definitely or probably the main cause of death” for 90 of the patients surveyed, most of whom died between October 2005 and September 2006, infection from the bacterium was linked to 345 deaths over two years, the study found.
A total of 1,100 patients contracted the bug at the three hospitals in the period examined by the report. Other health studies have found that the bacterium was an underlying cause of death of 2,074 patients in England and Wales in 2005.
Auditors found doctors improperly prescribed broad-spectrum antibiotics and that hospital wards were too crowded to isolate infected patients.
Overworked nurses complained they didn’t have time to wash their hands or properly clean bedpans or toilets. Patients said they saw “exhausted nurses in despair, with their heads in their hands,” the investigators said.
Nixon said she had to plead with nurses to care for her father, who contracted the C. difficile infection after bowel surgery.
“One time at 7 in the morning he had to go [to the bathroom] and they didn’t have time to bring him a bedpan. They said, ‘Look, you’ll just have to do it in the bed.’ I said, ‘OK, now he needs a linen change.’ ”
“But at 9:30, they said, ‘You must go now, visiting times are over.’ I said, ‘I’m not going until I know he’s been changed, and he’s clean.’ ” But there were no clean sheets yet available, the nurses told her. “They said, ‘You’ll just have to leave it with us.’ ”
--
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.