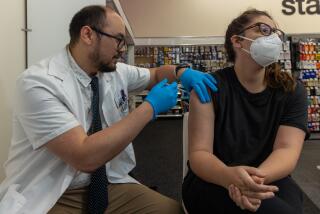
While COVID raged, another deadly threat was on the rise in hospitals
- Share via
As COVID-19 began to rip through California, hospitals were deluged with sickened patients. Medical staff struggled to manage the onslaught.
Amid the new threat of the coronavirus, an old one was also quietly on the rise: More people have suffered severe sepsis in California hospitals in recent years — including a troubling surge in patients who got sepsis inside the hospital itself, state data show.
Sepsis happens when the body tries to fight off an infection and ends up jeopardizing itself. Chemicals and proteins released by the body to combat an infection can injure healthy cells as well as infected ones and cause inflammation, leaky blood vessels and blood clots, according to the National Institutes of Health.
It is a perilous condition that can end up damaging tissues and triggering organ failure. Across the country, sepsis kills more people annually than breast cancer, HIV/AIDS and opioid overdoses combined, said Dr. Kedar Mate, president and chief executive of the Institute for Healthcare Improvement.
“Sepsis is a leading cause of death in hospitals. It’s been true for a long time — and it’s become even more true during the pandemic,” Mate said.
The bulk of sepsis cases begin outside hospitals, but people are also at risk of getting sepsis while hospitalized for other illnesses or medical procedures. And that danger grew during the pandemic, according to state data: In California, the number of “hospital-acquired” cases of severe sepsis rose more than 46% between 2019 and 2021.
Experts say the pandemic exacerbated a persistent threat for patients, faulting both the dangers of the coronavirus itself and the stresses that hospitals have faced during the pandemic. The rise in sepsis in California came as hospital-acquired infections increased across the country — a problem that worsened during surges in COVID-19 hospitalizations, researchers have found.
“This setback can and must be temporary,” said Lindsey Lastinger, a health scientist in the Centers for Disease Control and Prevention’s Division of Healthcare Quality Promotion.
Physicians describe sepsis as hard to spot and easy to treat in its earliest stages, but harder to treat by the time it becomes evident. It can show up in a range of ways, and detecting it is complicated by the fact that its symptoms — which can include confusion, shortness of breath, clammy skin and fever — are not unique to sepsis.
There’s no “gold standard test to say that you have sepsis or not,” said Dr. Santhi Kumar, interim chief of pulmonology, critical care and sleep medicine at Keck Medicine of USC. “It’s a constellation of symptoms.”
Christopher Lin, 28, endured excruciating pain and a broiling fever of 102.9 degrees at home before heading to the Kaiser Permanente Los Angeles Medical Center. It was October 2020, and the hospital looked “surreal,” Lin said, with a tent set up outside and chairs spaced sparsely in the waiting room.
His fever raised concerns about COVID-19, but Lin tested negative. At one point at the emergency department his blood pressure abruptly dropped, Lin said, and “it felt like my soul had left my body.”
Lin, who suffered sepsis in connection with a bacterial infection, isn’t sure where he first got infected. Days before he went to the hospital, he had undergone a quick procedure at urgent care to drain a painful abscess on his chest, and got the gauze changed by a nurse the following day, he said. Such outpatient procedures aren’t included in state data on hospital-acquired sepsis.
Someone with sepsis might have a high temperature or a low one, a heart rate that has sped or slowed, a breathing rate that is high or low.
It can result from bacteria, fungal infections, viruses or even parasites — “and the challenge is that when someone walks into the emergency department with a fever, we don’t know which of those four things they have,” said Dr. Karin Molander, an emergency medicine physician and past board chair of Sepsis Alliance. Treatment can vary depending on what is driving the infection that spurred sepsis, but antibiotics are common because many cases are tied to bacterial infections.
The pandemic piled on the risks: A coronavirus infection can itself lead to sepsis, and the virus also ushered more elderly and medically vulnerable people into hospitals who are at higher risk for the dangerous condition, experts said. Nearly 40% of severe sepsis patients who died in California hospitals in 2021 were diagnosed with COVID-19, according to state data. Some COVID-19 patients were hospitalized for weeks at a time, ramping up their risk of other complications that can lead to sepsis.
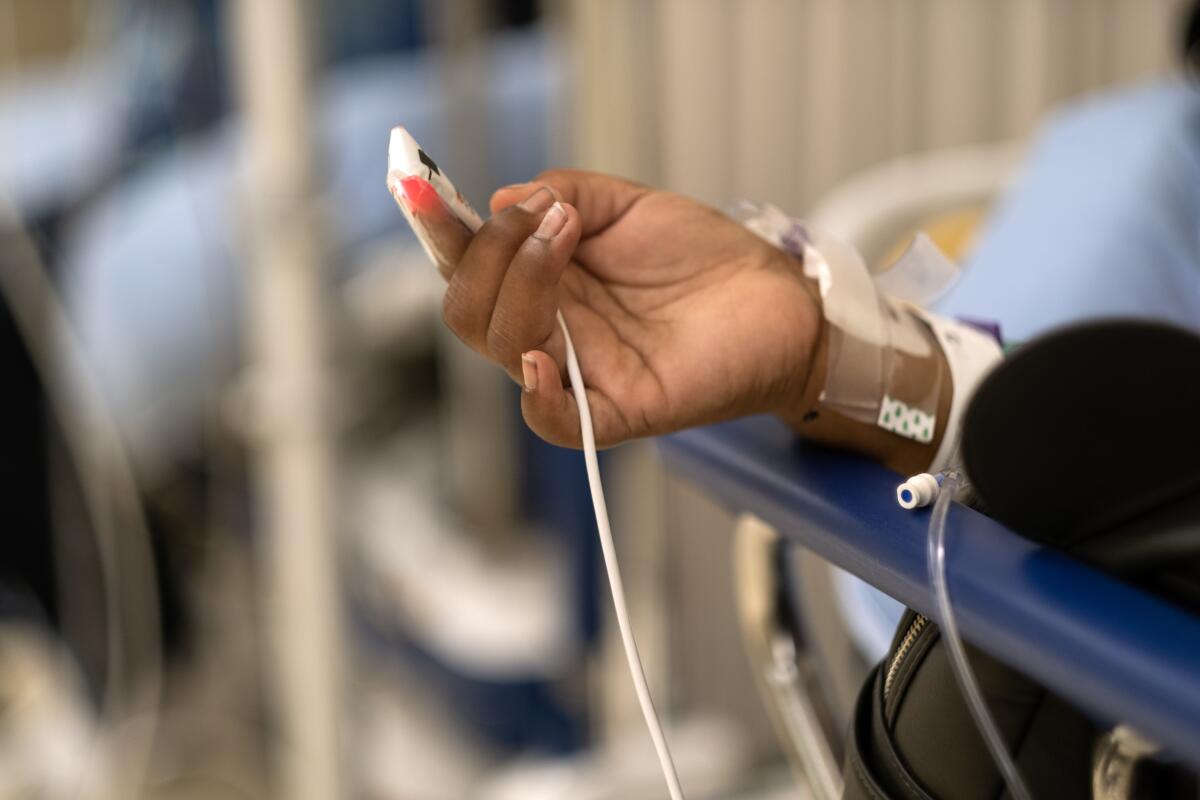
“The longer you’re in the hospital, the more things happen to you,” said Dr. Maita Kuvhenguhwa, an attending physician in infectious disease at MLK Community Healthcare. “You’re immobilized, so you have a risk of developing pressure ulcers” — not just on the backside, but potentially on the face under an oxygen device — “and the wound can get infected.”
“Lines, tubes, being here a long time — all put them at risk for infection,” Kuvhenguhwa said.
Experts said the pandemic may have also pulled away attention from other kinds of infection control, as staff were strained and hospital routines were disrupted. California, which is unusual nationwide in mandating minimum ratios for nurse staffing, allowed some hospitals to relax those requirements amid the pandemic.
Nurses juggling more patients might not check and clean patients’ mouths as often to help prevent bacterial infections, Kumar said. Mate said that hospitalized patients might not get their catheters changed as often amid staff shortages, which can increase the risk of urinary tract infections.
Hospitals might have brought in traveling nurses to help plug the gaps, but “if they don’t know the same systems, it’s going to be harder for them to follow the same processes” to deter infections, said Catherine Cohen, a policy researcher with the Rand Corp.
Armando Nahum, one of the founding members of Patients for Patient Safety U.S., said that pandemic restrictions on hospital visitors may have also worsened the problem, preventing family members from being able to spot that a relative was acting unusually and raise concerns.
Molander echoed that point, saying that it’s important for patients to have someone who knows them well and might be able to alert doctors, “My mom has dementia, but she’s normally very talkative.”
Sepsis has been a long-standing battle for hospitals: One-third of people who die in U.S. hospitals had sepsis during their hospitalization, according to research cited by the CDC. But Mate argued that sepsis deaths can be reduced significantly “with the right actions that we know how to take.”
In Pennsylvania and New Jersey, Jefferson Health began rolling out a new effort to combat sepsis in the fall of 2021, just before the initial Omicron wave began to hit hospitals.
Its system includes predictive modeling that uses information from electronic medical records to alert clinicians that someone might be suffering from sepsis. It also set up a “standardized workflow” for sepsis patients so that crucial steps such as prescribing antibiotics happen as quickly as possible, hospital officials said.
The goal was to lessen the mental burden on doctors and nurses pulled in many directions, said Dr. Patricia Henwood, its chief clinical officer. “Clinicians across the country are strained, and we don’t necessarily need better clinicians — we need better systems,” she said.
Jefferson Health credits the new system with helping to reduce deaths from severe sepsis by 15% in a year.
In New York state, uproar over the death of 12-year-old Rory Staunton led to new requirements for hospitals to adopt protocols to rapidly identify and treat sepsis and report data to the state. State officials said the effort saved more than 16,000 lives between 2015 and 2019, and researchers found greater reductions in sepsis deaths in New York than in states without such requirements.
If your child gets sick, he said, “you shouldn’t have to wonder if the hospital on the right has sepsis protocols and the one on the left doesn’t,” said Ciaran Staunton, who co-founded the organization End Sepsis after the death of his son. His group welcomed the news when federal agencies were recently directed to develop “hospital quality measures” for sepsis.
Such a move could face opposition. Robert Imhoff, president and chief executive of the Hospital Quality Institute — an affiliate of the California Hospital Assn. — contended that expanding the kind of requirements in effect in New York was unnecessary.
“I don’t think hospitals need to be mandated to provide safe, quality care,” Imhoff said.
State data show that severe sepsis — including cases originating both outside and inside hospitals — has been on the rise in California over the last decade, but Molander said the long-term increase may be tied to changes in reporting requirements that led to more cases being tracked. California has yet to release new data on severe sepsis acquired in hospitals last year, and is not expected to do so until this fall.
For Lin, surviving sepsis left him determined to make sure that the word gets out about sepsis — and not just in English. In the hospital, he had struggled to explain what was happening to his mother, who speaks Cantonese. After recovering, Lin worked with local officials to get materials from Sepsis Alliance translated into Chinese.
“I can’t imagine if it were my parents in the hospital,” he said, “going through what I was going through.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.