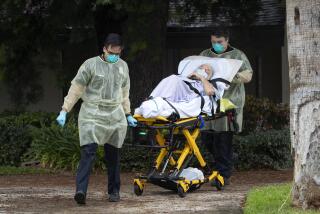
ERs fail as the nation’s ‘safety net’
- Share via
The long waits that government inspectors say endanger emergency room patients at Harbor-UCLA Medical Center can also be found in backlogged hospitals across the country, according to emergency care experts who have been trying for years to draw attention to the nation’s overloaded safety net.
“Overcrowding in our emergency departments is a national crisis,” said Dr. Linda Lawrence, president of the American College of Emergency Physicians, an advocacy group based in Washington D.C. “We no longer have the capacity to serve as the safety net for society.”
The group surveyed 1,000 emergency care physicians in September and found that one in five knew of a patient who had died because of having to wait too long for care, Lawrence said.
The death of an emergency room patient in December at Harbor-UCLA prompted California health officials, acting on behalf of the U.S. Centers for Medicare and Medicaid Services, to inspect the L.A. County hospital. William Harold Jones Jr., 56, was admitted to the emergency room on Dec. 22 but left the hospital before treatment was finished. His absence went unnoticed for hours before he was found dead on a sidewalk across the street.
County officials released a statement earlier this week that said they expected Harbor-UCLA to be cited for placing patients in “immediate jeopardy.”
Harbor-UCLA is the third hospital owned by Los Angeles County to undergo federal scrutiny in recent months for emergency room deaths.
“When somebody dies or somebody walks out the door and drops dead or a kid dies in the back of an ambulance, the typical press reaction is find the nurse, find the doctor, and crucify them,” said Dr. Arthur Kellermann, professor and chairman of emergency medicine at Emory University School of Medicine in Atlanta. “UCLA-Harbor . . . [has] been operating right on the edge in terms of volume of care for years. There’s just not any room left. This is the death spiral of American medicine, if we don’t figure out what to do.”
Report after report has laid out the crisis.
A review of 90,000 emergency room visits nationwide from 1997 to 2004 found that one in four heart attack patients waited almost an hour after arriving in a hospital emergency room before receiving care. Heart attack patients waited 150% longer for care by the end of the study period, or 20 minutes on average, up from eight minutes in 1997, according to the Harvard Medical School study published last month in the journal Health Affairs.
The National Institute of Medicine, an arm of the National Academies of Science, warned in a 2006 report that hospital-based emergency care was at a breaking point because of increasing demand and dwindling numbers of both emergency rooms and hospital beds.
The declining number of inpatient beds matters because emergency patients who need to be admitted for further treatment end up “boarding” in the emergency room -- often on gurneys in hallways -- until a hospital bed becomes available. Indeed, boarding is the key driver of the emergency room crowding crisis, the report said, taking up space and attention needed to treat the next emergency and leading to backlogged waiting rooms.
The gridlock is exacerbated by a chronic, nationwide nursing shortage and a dearth of specialists willing to be on call for emergencies, as well as by an aging population with increasingly serious medical needs.
The growing number of people without medical insurance also contributes because the lack of reimbursement, along with ever-shrinking payments from both public and private insurers, has turned many emergency rooms into money-losers and driven some hospitals out of the emergency-care business. Federal law requires hospital emergency rooms to treat patients regardless of their ability to pay.
The crisis is especially acute in Los Angeles County. In the South Los Angeles area alone, six emergency rooms -- which accounted for 100,000 emergency room visits a year -- have closed since 2003. Five were at private hospitals and one was at the county-owned Martin Luther King Jr.-Harbor Hospital in Willowbrook, which was cited last year in the death of a woman who writhed in pain for 45 minutes on the floor of the emergency room lobby without receiving medical attention. The county closed all but the outpatient clinics and urgent care center at King-Harbor in August after the hospital failed multiple inspections and lost federal funding.
“What we have is a persistent erosion of ER services, predominantly private, and that creates increasing pressure on every other hospital that runs an emergency room,” said Dr. Bruce Chernof, L.A. County’s director of county health services. Although his department “can do some things to mitigate the problem,” he said, “this is part of a larger issue across the county.”
County health officials are expected to report on Harbor-UCLA’s waiting times and triage system to county supervisors Tuesday and propose a plan to correct any weaknesses.
Lark Galloway-Gilliam, executive director of Community Health Councils, a health advocacy group, agrees that all hospitals are strained but believes that there’s more to the county’s problems than that.
“A lot of it has to do with management and oversight,” she said, echoing critics who have long advocated that the county hand off hospital oversight to an independent authority. County supervisors “do not have the skills or the time to protect patient care when resources are so scarce.”
She also said that the county brought on much of the current overcrowding, first by closing county-run clinics and more recently by shuttering King-Drew.
“We now see patients getting sicker and going to ERs, and the ERs don’t have the capacity to deal with this volume and level of illness,” she said. “People get overlooked, and people die.”
The county has not yet offered a plan to reopen Martin Luther King Jr.-Harbor Hospital. Chernof said Friday that negotiations with private operators are “active.”
Meanwhile, federal regulators have threatened to pull funding from the county-owned Olive View-UCLA Medical Center in Sylmar after government inspectors said the center failed to provide prompt medical screening for three emergency room patients last October. One of the patients, a 33-year-old man, had arrived at the emergency room experiencing chest pains. He never received a test to check if his heart was functioning properly. More than three hours after he came in, he collapsed and died of a heart attack.
The overcrowding is not expected to get better in the short term, even as the county prepares to move its flagship hospital, Los Angeles County-USC Medical Center, to a new facility in Boyle Heights as early as June. In 2002, the hospital was staffed to handle 750 beds; nursing shortages have reduced that to 650 beds. The new hospital is licensed for 600 beds.
“It’s going to reduce our flexibility,” said Dr. Stephanie Hall, chief medical officer of the Los Angeles County-USC Healthcare Network. “It will be a challenge for the system to provide care.”
Dr. Brian Johnston, an emergency room physician who has been practicing in Los Angeles for more than 30 years, criticized county supervisors for the decision to license fewer beds.
“I understand they don’t have a budget for it, but I also know they have a legal obligation to provide the services,” Johnston said. “The system is stretched beyond belief.”
Long-term solutions are years away. A long-awaited expansion of the Harbor-UCLA emergency room won’t be completed until 2011 at the earliest, said Carol Meyer, director of governmental affairs at the county’s Health Services Department. And building new facilities is expensive, costing $2 million per bed, Meyer said.
Recent attempts to raise revenue for emergency departments and health services have failed. In 2006, California voters rejected a $2.60-per-pack tax hike on cigarettes that would have funded expanded health services.
And in January, state senators killed a $14.9-billion healthcare reform package that would have arranged for medical insurance for nearly all Californians. If that effort had passed, Meyer said, Los Angeles County health services could have received an additional $200 million a year for its healthcare system, which would have been an 8% boost to its budget.
“The ER crisis has been going on for years,” said Emory University’s Kellermann. “What does it take to get our society and our government, state and federal, to focus on this?”
ron.lin@latimes.com
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.