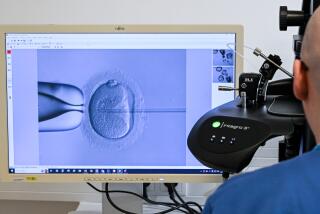
Fertility: a very private practice
- Share via
When the identity of Nadya Suleman’s fertility doctor was made public this week, the Internet lit up with angry commentary.
Many called for Dr. Michael Kamrava to be stripped of his medical license -- or worse -- for providing the fertility treatments that led to Suleman’s 14 children, including last month’s octuplets.
Rosalind Saxton had a different reaction.
“If anything, this incident has increased my confidence in the doctor,” said the 41-year-old, who has been preparing to do in vitro fertilization with Kamrava since three other doctors turned her down, telling her to lose weight first.
Suleman “was successful,” she said. “That would give anybody confidence.”
Saxton’s view contrasts sharply with that of fertility experts, who consider any pregnancy resulting in more than twins to be a poor outcome because of the danger it poses to the mother and babies.
Her view points to a key problem in fertility medicine: Treatment is a private bargain between doctor and patient, insulated from the outside world.
It escapes the scrutiny of insurance companies because most patients pay out of pocket. And it escapes government regulation largely because policymakers have been uncomfortable treading into the minefield of reproductive rights.
That makes the field ripe for periodic scandal and controversy: The 66-year-old woman who delivers twins, the doctor who steals eggs, the unwanted embryos in deep-freeze limbo.
The interests of fertility doctors and patients can converge with disturbing and even disastrous consequences that extend far beyond the people directly involved.
Patients, especially those with limited resources, may push for extreme treatments. And doctors, striving to succeed in a highly competitive field, may push the boundaries of good medical practice.
Children of “high-order” multiple births -- triplets and beyond -- usually arrive prematurely and are more likely to have developmental problems and disabilities.
Society can wind up bearing the cost, as in the case of Suleman’s octuplets, whose care may be covered by Medi-Cal -- the state health plan for the poor -- and could cost taxpayers millions.
Kirk O. Hanson, an ethicist at Santa Clara University, said Suleman’s case raises the issue of who should be allowed to have children and how many.
“We are loath to let the government have a say in this,” he said, “but an incident like this inevitably forces us to ask whether in vitro fertilization should be regulated.”
Suleman, 33, whose other six children are also products of in vitro fertilization, or IVF, receives food stamps. She told NBC news that in her most recent fertility treatment, she wanted all six of her remaining frozen embryos to be transferred into her to maximize her chance of another pregnancy.
Numerous fertility doctors said that so many embryos should never have been used for a woman her age. Professional guidelines suggest a maximum of two.
But all six embryos took, and two are thought to have split, bringing the number of fetuses to eight. She declined to undergo a procedure to reduce the number, which doctors often recommend in pregnancies involving three or more fetuses.
As news of the octuplets’ birth led to public outcry, the Medical Board of California announced it had launched an investigation into the case.
Before the octuplets brought him unwanted prominence, Kamrava sought attention as a pioneer in his field.
On his website, on television and in interviews on local Persian radio, he promoted unconventional fertility methods that he said would boost the chances that embryos would take.
In fact, he was a small player in the crowded field of fertility medicine in Southern California. His success rate was among the lowest in the country, according to statistics collected by the federal government. In the last five years for which data is available, only 30 of the 355 IVF procedures he performed resulted in live births.
At the same time, he was using more embryos per try than the vast majority of clinics nationwide, according to the statistics. Outside experts said the numbers suggested problems with his laboratory.
But there was little to hold him -- or any fertility doctor -- to account, beyond professional guidelines and the statistical reports required by the federal government documenting pregnancy and birth rates.
The Centers for Disease Control and Prevention posts the reports on its website and in a book published yearly. Eight percent of the nation’s 464 clinics don’t report their numbers, and there is no penalty for the lapse.
Other countries take a stricter approach. In Europe, laws limit the number of embryos that can be used in a single procedure. National healthcare typically covers a certain number of IVF treatments, taking the pressure off doctors to achieve success on their first try. Birth rates are generally lower, but so are rates of multiple births.
The U.S. fertility industry has long resisted calls for more regulation, arguing instead for a system of self-monitoring that focuses on helping struggling clinics improve their outcomes.
“Laws tend to interfere with the flexibility needed to treat patients on an individual basis,” said Dr. Michael Feinman, a Tarzana fertility specialist. He worried that “one doctor’s irresponsible behavior may bring restrictive legislation down on the rest of us.”
The laissez-faire approach has persisted despite ethical debates and scandal. A notable example occurred at UC Irvine, where in the mid-1990s a team of fertility doctors was found to be stealing eggs and embryos from patients and using them to impregnate other women. Two of the doctors are now fugitives in Latin America.
As reproductive technology has advanced, new controversies have arisen. Sexagenarians can now become pregnant, but not without serious risks to them and their babies.
At the same time, the procedures are becoming more accessible to everyone. With ads for discount IVF treatment abounding on the Internet and some clinics offering payment plans, fertility treatment is no longer just the realm of the rich. Poor childless patients bring shoe boxes stuffed with cash.
“We see patients who save up the money,” said Dr. Bruce Kovacs, a USC maternal fetal medicine specialist. Medi-Cal doesn’t cover IVF, which typically costs $15,000, but “once you are pregnant, the state pays the rest,” Kovacs said.
Despite the ethical quandaries, fertility industry leaders say their self-regulation generally works. The rates of triplets and other higher-order multiples fell from 7% of all IVF births in 1996 to 2% in 2006. The average number of embryos used in each procedure has also been decreasing.
Still, some experts say the numbers are too high.
Statistics show that some doctors vastly exceed the guidelines of the American Society of Reproductive Medicine, which recommends that most women under 35 receive one embryo, or two at most.
In 629 cases during 2005 -- a tiny fraction of the more than 35,000 treatments for women under 35 -- the patients received at least five embryos, according to a recent analysis by the CDC. Nearly 8% of the deliveries for those patients involved triplets or more.
Doctors who acknowledge exceeding the guidelines often say their patients are more difficult to treat -- a factor not included in the statistics.
To some patients, all that matters are success rates. They use the CDC data like Consumer Reports. And that can put pressure on doctors to use more embryos per procedure.
“What has evolved is a culture to achieve high pregnancy rates,” said Dr. Mark Hornstein, a reproductive endocrinologist at Harvard.
Patients are often willing to try anything, despite the risks.
“You’re just kind of like, ‘Let’s try the most aggressive treatment and do what we can and deal with it,” said Yasmin Thadani, 41, a former patient of Kamrava who did not become pregnant through IVF but later conceived naturally.
Some doctors operate under the principle that the customer is usually right.
“The sole custodian for the embryos are the father and mother,” said Dr. Hisham Greiss of the Midwest Fertility Center in Downers Grove, Ill. “If she is on the table and says put them all in, I have no choice.”
Greiss said he especially sympathizes with patients who have mortgaged their homes to pay for the procedure and want to transfer more embryos to increase their odds of success on the first attempt.
“This is the dilemma,” he said. “We always have this problem.”
When he can’t dissuade patients, Greiss has them sign a waiver accepting the risks.
For his patients under 35 in 2006, four of his clinic’s 29 births were triplets -- a rate nearly seven times the national average. Greiss said all four mothers were patients with low odds of conceiving. Each had insisted on three embryos, and they all took.
“I consider a triplet birth a failure,” he said.
--
Times staff writers Jessica Garrison and Kimi Yoshino contributed to this report.
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.