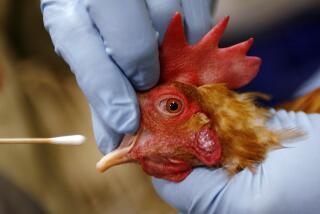
Tracking the swine flu virus
- Share via
The feds were on the phone explaining that a 10-year-old boy had a strain of swine flu no one had ever seen before.
As Dr. Michele Ginsberg listened, her mind flashed back to the days before the AIDS virus had been identified, when people were showing up at emergency rooms in California with a mysterious pneumonia.
Ginsberg, community epidemiology chief for San Diego County, where the boy was from, picked through her reports of unusual deaths, looking for similar cases. Nothing jumped out that April 16. And the county veterinarian didn’t have reports of sick pigs.
Ginsberg’s office called the boy’s mother to see if he had been in contact with pigs or other animals that could transmit flu to humans. If he hadn’t, it was likely that the virus had spread between people -- the last thing an infectious disease expert wants to hear.
“No animal exposure,” Ginsberg wrote in her notebook.
But the boy’s brother had been sick with fever and cough about two weeks earlier.
“Big deal!” Ginsberg added to her notes.
The virus has now traveled to 21 states and 18 countries, infecting more than 700 worldwide and killing about 115, all deaths save one in Mexico. It has riveted flu scientists and public health officials around the world. It appears to be relatively mild, perhaps no more deadly than a typical seasonal flu. But if it infects enough people, even a tiny death rate could add up to more fatalities than would be seen in a normal season -- perhaps many more.
In its early days, though, the virus was just a curious swab in a vial. The boy who had provided it was already better.
No one might ever have learned more about it except that the boy happened to come from a military family, and his sample was among those the Naval Health Research Center in San Diego was collecting as part of a study on a new flu test.
It came back as influenza Type A. Beyond that, the results were confusing. The Navy sent it to two labs in Wisconsin for analysis, but they couldn’t figure it out either.
The tests showed what it wasn’t: the dreaded H5N1 bird flu or either of two well-known strains of seasonal flu. But that did not explain what it was.
A distant cousin
The sample arrived by FedEx at Michael W. Shaw’s laboratory at the Centers for Disease Control and Prevention on April 15.
Inside the package were two vials. In each, a cotton swab floated on a liquid the consistency of an egg white. Shaw and his colleagues bathed the samples in a chemical solution to crack open the virus and expose its genes.
For four hours, a polymerase chain reaction, or PCR, machine copied the virus’ genetic material over and over, slowly revealing its odd genome.
Once he identified it as a swine flu, Shaw printed out a chart that showed how it fit on the family tree of swine flus -- it was out on its own lonely branch, a distant cousin to any other known virus.
“It’s been out there somewhere unnoticed, possibly in people, possibly in animals,” he said.
Six of the virus’ eight genes were from a strain that had circulated among U.S. pigs for more than a decade. But two others looked like those found in pigs from Asia and Europe.
The most likely scenario was that a single pig had been infected by both strains, which reassembled themselves into the new virus, said Richard Webby, an influenza expert at St. Jude Children’s Research Hospital in Memphis, Tenn.
That pig infected other pigs. Then, at some point -- nobody knows when, where or how -- the virus jumped to humans.
It was the scenario that “we’ve been on the lookout for,” Webby said. Any new virus is worrisome, because nobody is likely to have much immunity to it.
Even so, when the CDC identified the virus on April 16, scientists still saw it as more of a curiosity than a threat.
“I didn’t see anything to be alarmed about right then,” Shaw recalled.
That was about to change.
A death in Mexico
A parallel story was unfolding south the U.S. border, though nobody yet had connected the dots. In Mexico, a strange respiratory illness had been going around for at least a month. On April 13, it claimed its first life: that of 39-year-old Adela Gutierrez, a census worker in the city of Oaxaca.
When she had arrived at the hospital four days earlier, gasping for air, doctors suspected SARS, the virus that killed 774 people in Asia and Canada six years ago. She was quarantined after testing positive for a coronavirus, the virus group SARS belongs to. But a second test came back negative.
Tests were positive, though, for Type A influenza -- an unrecognizable strain.
“This case was what really alarmed us,” said Mexican Health Secretary Jose Angel Cordova.
Mexican scientists were not equipped to identify the killer on their own. So on April 17, Dr. Celia Alpuche Aranda, head of Mexico’s national microbiology lab, sent an e-mail to Dr. Frank Plummer in Winnipeg, Canada, describing the outbreak of respiratory illnesses in several Mexican cities.
Plummer, an infectious disease expert at the Public Health Agency of Canada, was at home watching a hockey game. When he saw the message on his BlackBerry, he too thought the unknown pathogen might be SARS, according to a spokesperson for the health agency.
Mexican scientists mailed 53 samples to Plummer’s lab to be tested for SARS and other respiratory illnesses. They included one from Gutierrez, the dead census worker, and 30 from La Gloria, a village in the southern state of Veracruz, where hundreds of people had developed a respiratory illness over the previous month that federal authorities then viewed as nothing more than a bad seasonal flu.
The outbreaks in Mexico had barely registered with U.S. health officials. A CDC timeline indicated that the Mexican government did not inform the agency about the respiratory illnesses until April 12.
Eight days later, the CDC for the first time hypothesized that its new virus might be related to the Mexican cases.
On April 23, the Canadian lab results came in: no SARS, but 17 of the 53 samples were nearly identical to the U.S. virus. One was from a 5-year-old boy from La Gloria: He’d been sick for a week in early April, making him the earliest confirmed case in Mexico.
That night, the Mexican health secretary went on national TV to announce the presence of the disease and to close schools in Mexico City and the adjacent state of Mexico.
Scientists mobilized
As events unfolded, scientists around the world were hankering for a closer look at this new flu virus, H1N1. They got their first chance on Monday, when the National Institutes of Health published the genetic sequence online at https://www.ncbi.nlm.nih.gov /genomes/FLU.
The sequence got more than 10,000 hits in the first 24 hours, said David Lipman, the director of the National Center for Biotechnology Information at the NIH. One gene segment was downloaded 2,000 times.
Peter Palese, an influenza expert at Mt. Sinai Medical Center in New York, searched the genetic letters on one of the genes. He was looking for the code for one amino acid, a telltale marker of both the deadly H5N1 avian flu and the 1918 flu that claimed an estimated 50 million lives worldwide.
To his relief, it wasn’t there.
More good news came when CDC researchers conducted genetic tests on 13 of the virus samples collected in the U.S. All were vulnerable to the common antiviral flu drugs Tamiflu and Relenza, although resistant to two others.
The U.S. government is now mobilizing more scientists to study the new virus.
A thimble-sized vial arrived by mail Wednesday at Ralph Tripp’s laboratory at the University of Georgia. The lab has begun culturing it in eggs and canine kidney cells in preparation for experiments designed to see how easily it spreads among animals.
The lab will start by infecting ferrets by squirting pipettes of the virus into their nostrils and then housing them with uninfected ferrets. More than two dozen pigs are on order for further testing.
Back in Southern California, epidemiologists have been interviewing and swabbing hundreds of people suspected of having the H1N1 flu or of coming into contact with it.
They are still trying to figure out the extent of human-to-human transmission, the trait that first set off alarm bells in Ginsberg’s mind.
Ginsberg still doesn’t know whether the 10-year-old San Diego County boy gave it to other members of his household. Public health nurses collected blood from his parents and sent the samples to CDC; they are waiting to hear back.
“My own feeling is, we’re just recognizing a very small number of people who have been infected,” Ginsberg said. “We learn more every day.”
--
alan.zarembo@latimes.com
Times staff writer Tracy Wilkinson contributed to this report from Oaxaca.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.