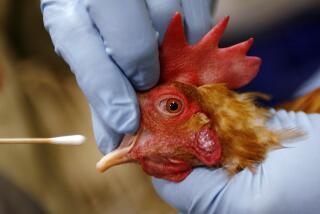
Swine flu virus causing confusion
- Share via
As health officials brace for a new onslaught of illness from the novel H1N1 virus, they remain perplexed by one of the most unusual and unsettling patterns to emerge from this pandemic -- the tendency of the so-called swine flu to strike younger, healthier people.
The initial explanation was that the elderly, who are usually most vulnerable to the flu, have built-in immunity as a result of their exposure more than 50 years ago to ancestors of today’s pandemic strain. But the limits of the theory are becoming more clear. For starters, only a third actually have antibodies to the new H1N1.
“It doesn’t quite look as though it’s the whole story,” said Dr. William Schaffner, chairman of the department of preventive medicine at Vanderbilt University School of Medicine in Nashville.
Further, the flu’s two key genes came directly from pigs and are new to everyone. That means all age groups should be equally vulnerable since no one has encountered the genes before. Yet infants seem to be in less danger than older children and most adults.
Unraveling these mysteries will be crucial to designing a strong defense against this tenacious virus. Tests in animals strongly suggest that H1N1 will be with us for the foreseeable future, supplanting the strains that cause seasonal flu within a year or two.
Understanding the virus’ inner workings will also help scientists prepare for future influenza pandemics.
H1N1’s unorthodox nature became apparent as soon as the virus burst onto the scene in early spring: Most of the earliest cases in the U.S. and Mexico occurred in children rather than the elderly.
In the U.S., half of the people with confirmed H1N1 cases have been 12 or younger, according to the Centers for Disease Control and Prevention. Until July 24, when the CDC stopped counting new cases, 60% of patients whose ages were known were between 5 and 24 years old. An additional 20% were in the 25-to-49 age group. Only 1% of those sickened had reached the age of 65.
Younger people also appear to be getting the most severe cases of pandemic flu. The median age of patients requiring hospitalization is 20, according to the CDC. In fatal cases, the median age is 37.
Those figures are in stark contrast to the seasonal flu, which is most likely to sicken people who are elderly, very young or chronically ill. More than 90% of fatal cases involve senior citizens.
H1N1’s link to 1918
Scientists had theorized that the new H1N1 swine flu descended from the 1918 Spanish flu, an H1N1 strain that killed an estimated 50 million people worldwide. Older people who had been exposed to that virus must have built up immunity that protected them against the new pandemic strain.
But an analysis published last week in the New England Journal of Medicine found H1N1 antibodies in blood samples from only 39 of 115 people born before 1950, a rate of 34%. The results supported a similar analysis released in May.
Over the summer, researchers who tested blood samples from Japan found that few people born after 1918 had antibodies that protected them against the new H1N1. But most of the people over the age of 90 did.
That suggests immunity came only from the initial versions of Spanish flu, not from the myriad offshoots to which most elderly people were exposed. For them, protection came from something else.
“Other components of the immune response no doubt also contribute to reduce disease,” said Jacqueline Katz, chief of immunology and pathogenesis in the CDC’s Influenza Division. But she said that scientists didn’t know what those might be.
Then there’s the matter of the key H and N genes in the new H1N1 virus. Although they have much in common with the corresponding genes from the 1918 strains, both came directly from pigs. No one should have immunity.
Baffled by fatalities
It may turn out that prior experience with H1N1 has very little effect on who will wind up with the most severe cases of swine flu.
Consider this alternative explanation for the unusually young age of H1N1 victims from Dr. Peter Wenger, a professor of preventive medicine and community health at New Jersey Medical School in Newark: Perhaps their more vigorous immune systems are simply mounting stronger challenges to the flu virus.
If bodies overreact and release too many infection-fighting proteins called cytokines, the resulting “cytokine storm” can cause severe inflammation that overwhelms the lungs and respiratory tract. In extreme cases, the reaction can be fatal.
Many scientists have speculated that this kind of calamitous immune response may have been at work in 1918. But the theory is difficult to test.
“The immune system is such a finely modulated system,” he said. “When you start pulling out cells and putting them in test tubes, it gives you some idea, but is it really what happened?”
Though the overall H1N1 fatality rate remained low over the summer during the Southern Hemisphere’s flu season, deaths continued to be concentrated among middle-aged adults.
For example, in New South Wales, Australia’s most populous state, half of the 48 deaths were in people in their 40s and 50s, according to figures from the government’s health department.
Though children and young adults have higher rates of H1N1 infection, the fatal cases are more likely to involve middle-aged adults because they have higher rates of the underlying medical conditions that make H1N1 deadly, such as asthma, diabetes and heart disease, said CDC spokeswoman Artealia Gilliard.
Dr. Harry Greenberg, a professor of microbiology and immunology at Stanford University School of Medicine, said he was puzzled about why H1N1 had caused relatively few deaths in infants and young children considering that they lack the antibodies that appear to be protecting the elderly.
“I don’t have a good explanation to totally account for this,” he said, “except to say it’s early in the data-gathering business.”
--