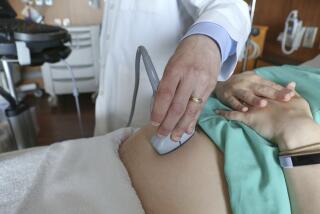
Voice mail a blessing and a curse for doctor
- Share via
9 a.m.: “Doctora, it’s Señora H. I’m at the walk-in clinic, but they say I will get whichever doctor is available. I’d rather see you. Please call me.”
10 a.m.: “Doctora, por favor, call me. I don’t want to wait so many hours to see some random doctor. Maybe you can squeeze me in?”
11 a.m.: “It’s Señora H. Por favor, call me. I don’t want to wait at walk-in.”
Noon: “I don’t want to see another doctor. Only you. Call me.”
Voice mail is both a blessing and a curse. When we were first given voice mail in our clinic, it was a revolution. Previously, our patients had to hope for the best with front-desk phones staffed by overworked and often impatient clerks who answered only intermittently. Now our patients could actually reach their doctors, and this link was crucial to their health.
But sometimes voice mail is a ball and chain, as it seemed now, at half past noon, having just arrived in my office after spending the morning in another part of the hospital. My first patient wasn’t scheduled until 1 p.m., but I’d skipped lunch and arrived early because I needed to leave exactly at 5 p.m. The baby sitter who normally met my kids at the bus was away, so being late was not an option.
I replayed Señora H.’s messages, trying to keep the mixed feelings at bay. I know how miserable it is to wait at a walk-in clinic and how much better it is to see one’s own doctor.
“Do the right thing” is the mantra that is distilled from the Hippocratic oath. The right thing would be to pluck the woman’s chart from the walk-in bin and add it to my own schedule. It would speed things up for her. It would be better medicine.
But I hesitated. I hesitated because I knew I couldn’t stay late. I hesitated because I suspect that Señora H. takes advantage of my voice mail, calling me on an almost weekly basis, with every message stated as an emergency. I hesitated because accommodating her would reward her for her constant phone calls. But I hesitated mainly because this would reward “the system.”
The system works because doctors in our clinic overwhelmingly choose to “do the right thing.” When our patients can’t get a soon-enough appointment, we overbook them to our schedules. When it’s hard to get a cardiology appointment, we get on the phone and pull strings. When an urgent form needs to be filled out, a prior approval needs to be called in or an appeal letter needs to be written, we always say yes.
Voice mail simply increases the number of tasks for the doctor to fit in.
I am proud of that ethic, proud that my colleagues can be reliably counted on to “do the right thing.” This is what we teach our students, and this is the basic essence of professionalism. However, it takes its toll.
It’s not as though the administration gives doctors an extra hour each day to handle all these requests and extra patients. It’s simply expected that each doctor will somehow manage it. In practice, it means doctors work through lunch and always leave late.
The fallout, though, is that these requests start to feel like personal attacks. Señora H’s messages feel like a direct assault on my time. The cold calculus is that minutes given to her will be time taken away from my other patients and from my children at the end of the day. It is a horrible feeling on all ends.
This, I am convinced, is at the root of the primary-care crisis. It’s hard to imagine a lawyer routinely carving out extra, non-billed hours. Yet it’s the unquestioned assumption for doctors. As it chips away at their lives, the tensions rise.
I almost wish I hadn’t listened to my voice mail. If I hadn’t known of Señora H’s request, I wouldn’t be in this dilemma. With a heavy heart, I proceed as though I hadn’t received her message. I try to assuage my guilt by reminding myself that the walk-in clinic exists for patients like her who need an urgent appointment.
The afternoon is brisk, and as usual there isn’t a moment to spare. I work steadily, glad that I am able to do a reasonably thorough job with all my scheduled patients. Each time the phone rings I check the number to see if it’s Señora H, not sure if I’d actually have the guts to let it pass to voice mail. Luckily, she doesn’t call.
I finish my last chart with just enough time to dash to the bus stop. I check the computer and see that Señora H has been taken care of by a colleague in the walk-in clinic. I debate whether to call her now, worried that once I get on the phone with her I won’t be able to get off.
“Do the right thing” runs through my head. I can postpone returning her call, but I can’t ignore it altogether. I dial her number and feel guilty at my relief that her voice mail picks up. I leave a message apologizing for not being able to see her and say that I hope she is feeling better. I sign off with my standard end-phrase — “Call me if things don’t get better” — hoping that this won’t be engendering more work in the future.
I sprint to the bus stop and arrive just as the yellow school bus is pulling in. I am overjoyed to be there when my children come spilling noisily out of the bus, but I can’t shake the feeling that I’ve been derelict in my clinical duty. I know what I did was OK — by the book, at least. Señora H was not left without medical care, she was merely inconvenienced. Nevertheless, it doesn’t sit right with me. We’re supposed to go the extra mile. But I can’t deny that it makes the job more onerous.
One by one, my colleagues are dropping out. They are switching from the bottomless pit of outpatient medicine to the controlled environment of inpatient medicine. Inpatients are sicker, but there are regulations that limit the number of patients who can be admitted to a single team. No such rule exists for doctors who work in outpatient medicine.
Primary-care doctors are supposed to be the linchpins of the medical system and the key elements of proposed reforms. But the linchpins are creaking. Every doctor I know wants to “do the right thing,” but if the system continues to rely on individual compromises and personal sacrifices, then it can’t ultimately succeed.
Danielle Ofri is an internist in New York City. Her newest book is “Medicine in Translation: Journeys With My Patients.” She can be reached at author@danielleofri.com.