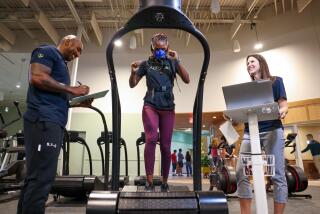Why ‘wellness’ program scams cost employers and harm employees
- Share via
Perhaps the most popular fad at large today in the employee health benefit world is the “wellness” program.
We wrote last month about how some big employers may be using these programs--which include incentives for smoking cessation and weight loss along with mandates for annual checkups and preventative disease screenings--may be aimed more at saving companies money than at promoting better health. The goal is to charge higher premiums for workers who don’t participate, or who fail to meet wellness milestones.
Now there’s more evidence that the programs don’t save companies money--even when the higher premiums are factored in. In fact, according to a study published on the Health Affairs blog, they cost companies money. The most shocking, not to say surprising, showing in the article by healthcare consultants Al Lewis and Vik Khanna and healthcare management expert Shana Montrose is that most of the claims for cost savings from these programs come from the firms hawking the programs, often using bogus comparisons and surveys that haven’t been peer-reviewed.
Some are designed in a way that makes it impossible to determine if the supposed savings in healthcare expenses are the result of wellness incentives or other features. Others fail to make clear that the greatest savings from wellness campaigns come from small subsets of employees with costly chronic diseases, such as diabetes--and those savings might be captured just as well by targeted disease management programs that are cheaper and less broadly coercive.
The researchers also observe that the supposed savings in hospitalization costs for wellness-sensitive diseases--say those related to obesity--are typically outweighed by the expenses companies incur for annual physicals and unnecessary screenings demanded by the wellness scheme. These costs and benefits are difficult for company HR departments to compile, so they rely on data provided by their wellness consultants--not exactly the most objective source.
“There is no clinical evidence...that three pillars of workplace wellness—annual workplace screenings and/or annual checkups for all employees (and sometimes spouses), and incentivized weight loss—are cost-effective,” the authors state.
Some may do more harm than good. “The benefits of annual screening (as all wellness programs require) may not exceed the harms of potential false positives or of over-diagnosis and overtreatment.... Likewise, most literature finds that annual checkups confer no net health benefit for the asymptomatic non-diagnosed population.”
Another issue: Some programs may provide incentives for unhealthy behavior. Those tied to weight loss at two consecutive weigh-ins “may encourage overeating before the first weigh-in and crash-dieting before the second, both of which are unhealthy.”
Despite these emerging data, the Kaiser Family Foundation has calculated that more than half of all companies with more than 200 workers offer health screening programs; 8% of those offer an incentive to participate or a penalty for refusing.
The issue has begun to surface in court: The Equal Employment Opportunity Commission has challenged an incentive program imposed by Honeywell International on its employees as coercive.
A federal judge ruled against the EEOC last month, but Lewis, Khanna and Montrose suggest that the evidence is so flimsy that these programs pay their way that they may be vulnerable to further legal challenge. They say the right course for employers is to stop taking the financial benefits of “wellness” schemes as a given, and “demand that their vendors and consultants answer open questions about their programs.”
As you might expect, workplace wellness is a hot issue in the medical field. For a good series of posts on the topic, see Austin Frakt and Aaron Carroll here.
Keep up to date with the Economy Hub. Follow @hiltzikm on Twitter, see our Facebook page, or email mhiltzik@latimes.com.
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.