FDA approves Amgen cholesterol-lowering drug Repatha for some patients
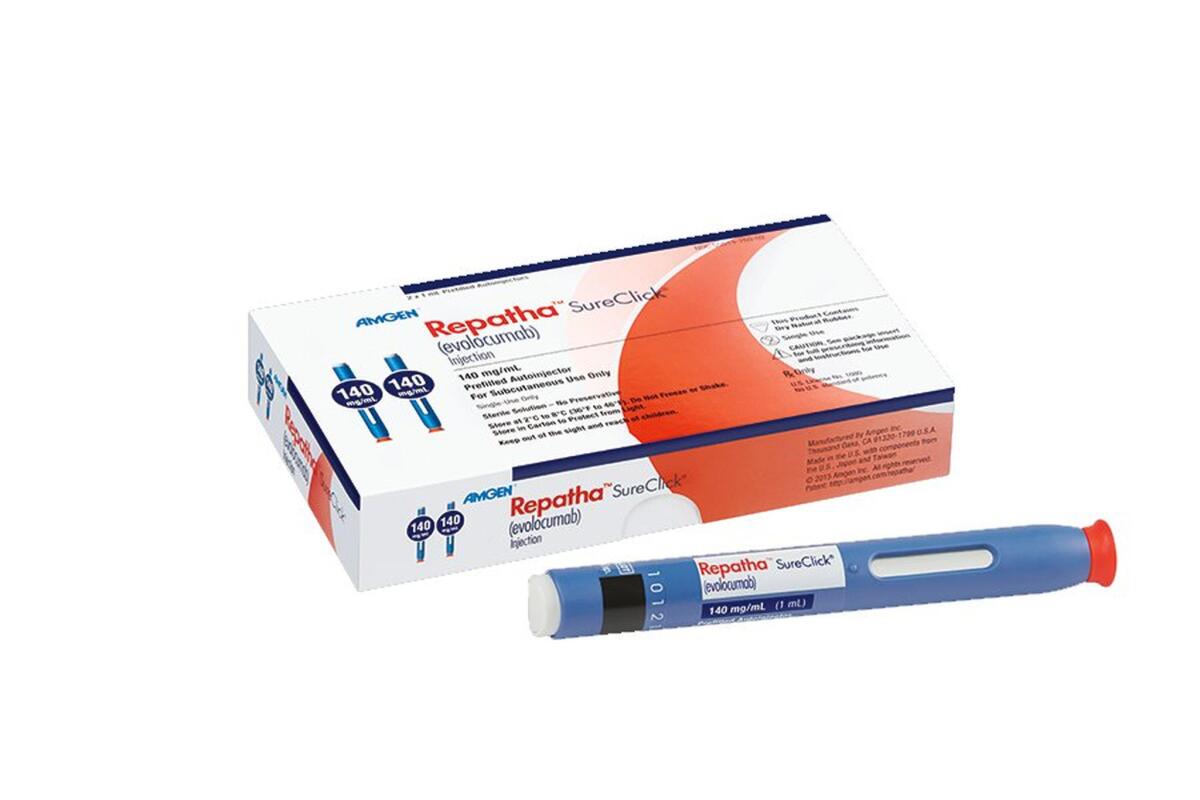
Amgen has big hopes for cholesterol drug Repatha, which one analyst estimated could reach $4 billion per year in annual sales.
- Share via
The government’s approval of a new drug to lower cholesterol could mean billions of dollars for Thousand Oaks biotech giant Amgen — and spark a new round of debate over the thousands of dollars it will cost patients and their insurers.
The Food and Drug Administration’s approval Thursday of Repatha — an alternative for millions of patients who get no help from widely prescribed statins — is expected to meet resistance from health insurers and pharmacy-benefit managers over those cost concerns. The drugmaker said Repatha would start with a list price of $14,100 for a year’s worth of treatment.
Developed by Amgen’s scientists, it is the second in a new class of drugs that lower cholesterol by blocking a protein called PCSK9 that interferes with the body’s ability to remove LDL, so-called bad cholesterol. The drug is approved for people with inherited forms of very high cholesterol and certain kinds of cardiovascular disease.
Repatha, which is injected, can reduce LDL by 54% to 77%, according to Amgen. LDL is a significant risk factor for heart attack and stroke. The FDA said Repatha should be used as an addition to diet and other LDL-lowering treatments. The move marks a new option for patients who might have cholesterol levels as high as 400.
Express Scripts Holding Co., the nation’s largest manager of prescription drug benefits, said in a statement that up to 10 million people are affected by these levels of high cholesterol, and the new class of drugs to treat them has “the potential to grow over the next several years to become the costliest therapy class our country has seen.”
Analysts expect the actual price of Repatha to decrease once rebates and other discounts are taken into account. Amgen acknowledged concerns about the drug’s cost, saying that the company would work with payers to provide “innovative pricing programs.”
Amgen has big hopes for Repatha, which one analyst estimated could reach $4 billion per year in annual sales. That would be a huge boost for Amgen, which reported about $20 billion of revenue last year. Its top-selling drugs were arthritis drug Enbrel, with $4.7 billion in sales, and Neulasta, which boosts infection-fighting white blood cells, at $4.6 billion. Repatha has already been approved in the European Union for patients with uncontrolled cholesterol.
In July, the FDA approved a similar treatment called Praluent from French drug company Sanofi and Regeneron Pharmaceuticals, its New York partner. Both drugs are an alternative to statins — including the former blockbuster Lipitor — which are cheap and effective but can cause side effects. Last year, Amgen sued its two rivals, alleging that Praluent infringed Amgen’s patent. The lawsuit is pending.
Makers of both drugs are conducting clinical trials to determine whether the drugs will reduce heart attacks and strokes.
Some health-policy experts are worried about the long-term costs of these new drugs and the financial effect on the nation’s $3-trillion healthcare system.
In June, FDA advisory panels recommended both Repatha and Praluent for patients with familial hypercholesterolemia, a condition that affects an estimated 600,000 people in the U.S. But the drugs also may benefit patients who can’t reduce their LDL with statins, or who can’t take statins because of side effects. That means as many as 3.5 million more Americans may qualify initially for these new medications, according to analysts.
And the patient population could grow substantially over time if the drugs were recommended for people with a history of coronary artery disease, potentially expanding the number of people by many millions more.
For now, health insurers and pharmacy-benefit managers probably will require doctors and patients to exhaust other options first or obtain additional lab tests before getting a prescription. Repatha is administered once every two weeks.
“Given the number of people potentially eligible for treatment with the PCSK9 inhibitors will number in the millions, the potential overall expenditures by payers are huge,” officials at CVS Caremark, a pharmacy benefit manager and drugstore chain, warned in a medical journal earlier this year. “The healthcare system has never seen a challenge like this to our resilience in absorbing costs.”
There are also concerns because it can take longer to develop cheaper, generic versions of these biologic drugs.
Many in the field think the drug will be narrowly prescribed for extremely high-risk patients at least until 2017, when a series of trials will test whether there’s a benefit to treating emergency room heart attack patients with both a statin and the new drugs like Repatha. If the studies show positive results, there could be a much wider adoption of the new drug, said Dr. Ethan Weiss, a cardiologist at UC San Francisco.
There’s no indication that the pharmaceutical companies are touting drugs like Repatha as a statin replacement, only an addition, which will keep prescription numbers lower, he said.
The price of Repatha is similar to the $40-per-day cost of Praluent. Both are available to Express Scripts patients only through a medical exception process until the organization makes a decision next month on whether to cover the products.
Amgen shares closed up $1.74, or about 1%, at $155.72 before the announcement, which came after hours.
stuart.pfeifer@latimes.com
samantha.masunaga@latimes.com
Times staff writer Chad Terhune contributed to this report.
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.