New staffing law, old struggles bedevil California nursing homes

- Share via
The 93-year-old dementia patient was getting anxious in her wheelchair.
The woman, a resident of the Californian-Pasadena nursing home, wanted to see her husband but had forgotten he was at a nearby hospital.
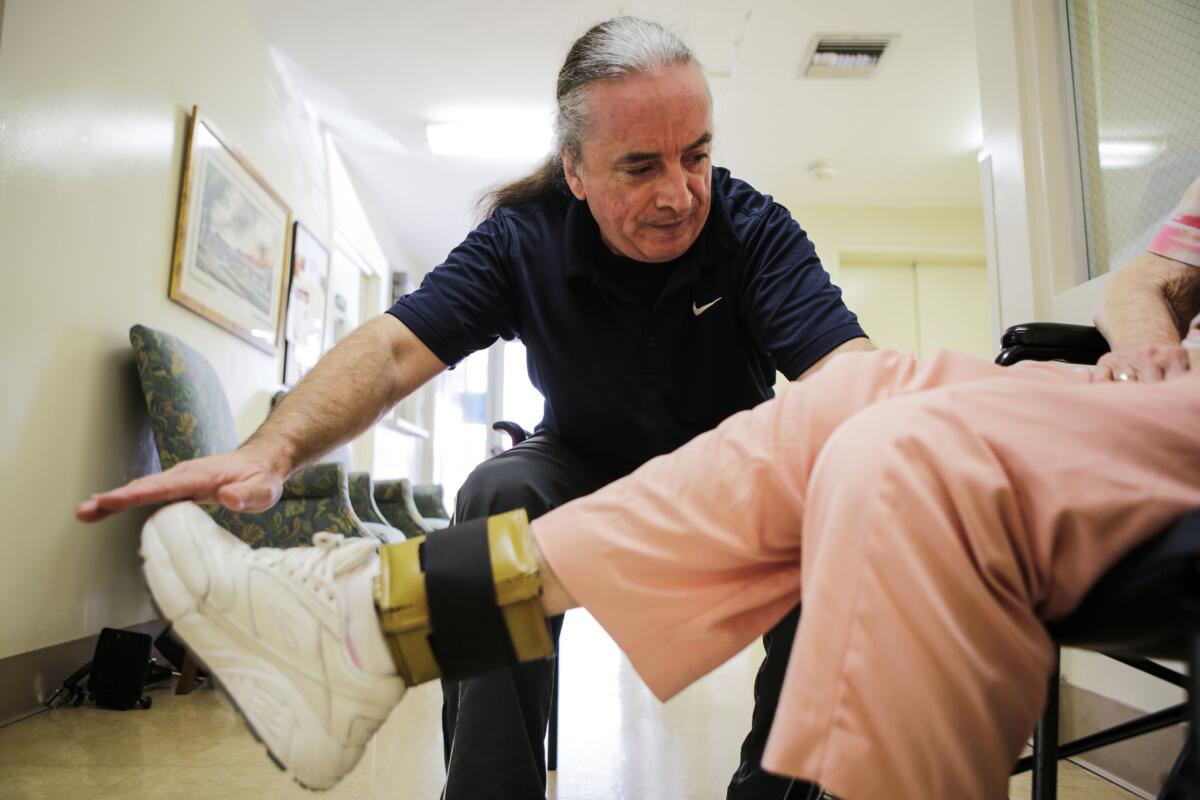
Holding the chair steady was a composed Gabby Carrillo, a certified nursing assistant who had witnessed this behavior before.
“We try to see things in their shoes,” said Carrillo, a CNA for more than three years. “Doing this job can be exhausting, not just physically but mentally too. Over time, you learn to cope with it.”
Despite the challenges, the 27-year-old professes a love for her job, which involves bathing, feeding and attending to other daily needs of patients. But the stressful work — coupled with low wages and a booming economy — has made it more difficult than ever for nursing homes to fill the position.
Now, state legislation that went into effect July 1 is putting even more pressure on the state’s 1,000-plus nursing homes, which some in the industry say could be forced to turn away or even discharge patients as a result.
The law, championed by organized labor and patient advocates, tightened staffing requirements for direct caregivers and added new ones specifically for certified nursing assistants.

The Service Employees International Union, which pushed for the law and represents nursing assistants, acknowledges that nursing homes face a challenge, but said there is an overriding health-and-safety issue.
“There must be enough direct care staff to meet the quality care needs of nursing home residents and ensure a healthy workload for every caregiver,” said an SEIU local representative who declined to be identified.
Quality-of-care concerns have long plagued nursing homes and are well documented, most recently in a May report by California State Auditor Elaine Howle.
The report dinged the California Department of Public Health for its oversight of nursing homes. And it found a one-third increase from 2006 to 2015 in violations of federal regulations that were likely to cause serious injuries or death.
“We are at rock bottom,” said Patricia McGinnis, director of California Advocates for Nursing Home Reform, a patient advocacy group. “I don’t ever want to go to a nursing home, and I don’t know anyone who would.
The new law requires facilities to provide 3.5 hours of direct patient care each day, up from 3.2 hours. But the primary worry for nursing home operators is a first-ever requirement that 2.4 of those hours must be filled by CNAs.
The department will begin enforcing the law July 1, 2019, and homes that fail state audits face penalties of $15,000 to $30,000.
We are at rock bottom. I don’t ever want to go to a nursing home, and I don’t know anyone who would.
— Patricia McGinnis, director of California Advocates for Nursing Home Reform
Citing a lack of trained personnel, an industry trade group is warning that close to half of California homes won’t meet the requirement.
“We’ve got an access-to-care issue,” said Matt Robinson, legislative director of the California Assn. of Healthcare Facilities. “If the bodies aren’t there, this is empty legislation.”
There are roughly 32,000 certified nursing assistants in California serving some 100,000 patients admitted annually. While the job’s responsibilities include personal care, CNAs also provide medical services such as taking vitals and helping treat pain.
But the average certified nursing assistant in California made only $13.96 per hour in 2016, according to state data. That’s just a few dollars above the minimum wage and less than what some retailers are now paying to attract sales clerks — who unlike CNAs don’t need to spend extra time and money to get licensed.
In addition to low wages and a high-stress working environment, retaining CNAs is a challenge for the industry, said Ken Merchant, a Sacramento-area nursing home consultant.
The job requires prospective CNAs to take 100 hours of clinical training and 60 hours of classroom instruction.
Training is offered through about 700 programs across the state, many at community colleges, adult education programs and for-profit schools, with most charging several hundred dollars.
However, the number of nursing homes offering in-house training — often provided for free to recruit workers — has plummeted to 48 as of this year from more than 300 in 2001. The nursing home industry cites tighter budgets.
In May, the California Department of Public Health granted the healthcare facilities association $2.4 million to establish more in-house training programs, but they have yet to open. The Legislature also is considering a bill that would allow CNAs to receive their classroom training online.
Many homes plan to seek waivers, which are allowed for by the law as long as a facility hasn’t been cited in the last three years for health and safety violations that injured or killed a patient.
There are two waivers available, according to the Public Health Department: one for facilities that can’t meet the requirement due to a workforce shortage and another for facilities that meet patients’ needs and reach the 3.5-hour ratio but not the 2.4-hour requirement.
Homes have until Sept. 1 to seek a waiver with the department, which expects to reach decisions on the applications by Jan. 30. The workforce-shortage waiver is limited to two consecutive years; details of the other waiver are still being worked out.
Half of California’s counties are designated by the Public Health Department as having a CNA worker shortage. That includes many of the least-populated, rural counties. Those tend to have fewer resources and money, making it more difficult to recruit and retain a CNA, said Robinson of the industry trade association.
A lot of us need a second job to maintain ourselves. Some of us are full-time students and part-time CNAs on top of that
— Gabby Carrillo, certified nursing assistant
Still, even those homes are not guaranteed waivers.
Julianne Williams is the co-founder and chief executive of Dycora Transitional Health & Living, which operates 19 homes, many in Fresno and Tulare counties.
Dycora, based in Fresno, employs about 2,100 people in California, including about 900 certified nursing assistants.
Williams said a majority of her facilities are already compliant with the 3.5-hour requirement but will not be able to meet the CNA ratio and will need waivers.
Dycora already has taken steps to attract workers by using Eleos, a CNA training program to feed more workers into its homes.
“It’s where we get a lot of our CNAs, and they’re trained well,” said Williams, a former CNA herself. “[Eleos] is helpful and we want to bring in as much staff as possible, but we have to be realistic.”
She said that if the state does not give the industry more time to meet the requirement through the waiver process, she and other operators might have to start turning away new patients.
“We’re not going to make that decision right now, but if it comes to the point that we cannot meet the staffing expectation, what we would do is limit admission so our occupancy would go down as people discharged,” Williams said.
Robinson goes so far as to warn that facilities might start removing beds and discharging admitted patients.
“If a facility doesn’t have a waiver and isn’t compliant with the 3.5- and 2.4-hour ratios, there wouldn’t be another way to make sure they can comply,” he said.
McGinnis, the patient advocate, strongly supports the ratios and discounts such talk as fear mongering.

Of course, not all nursing homes are in the same predicament.
Among those is the Californian-Pasadena, which provides about 3.1 hours of CNA care per patient per day, according to data from the Office of Statewide Health Planning and Development.
With about 58 patients a day, the facility adjacent to Huntington Hospital is upscale and smaller than the typical nursing home. Nearly half its income comes from private pay, with most of the rest coming from Medicare.
The majority of nursing homes in California, by contrast, draw more than half their revenue from Medi-Cal, the state program that provides health services to low-income residents, which the industry complains doesn’t cover the cost of care.
You’re looking for angels falling out of the sky to fill these shortages.
— Luis Pages, administrator at the Californian-Pasadena
The healthcare facilities association estimates that in 2015, Medi-Cal on average reimbursed facilities about $206 for each day a patient was admitted, while the average cost per patient day was $289.
With its richer income stream, the Californian-Pasadena pays its CNAs as much as $15 an hour, making it a competitive employer in a city where the minimum wage was raised July 1 to $13.25.
“We tend to fare better because we are more robust than most in Pasadena,” said Luis Pages, the home’s administrator. “Others in the industry would probably look at our model and say it was ridiculous.”
Still, Carrillo said the wage isn’t enough to live on, making the job desirable really only to people who like to serve the frail and elderly.
“A lot of us need a second job to maintain ourselves,” she said. “Some of us are full-time students and part-time CNAs on top of that.”
Pages agreed the pay isn’t high enough across the industry, calling it “a bit shameful.”
“You’re looking for angels falling out of the sky to fill these shortages,” he said.
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.










