More people are being illegally billed for charges not paid by Medi-Cal
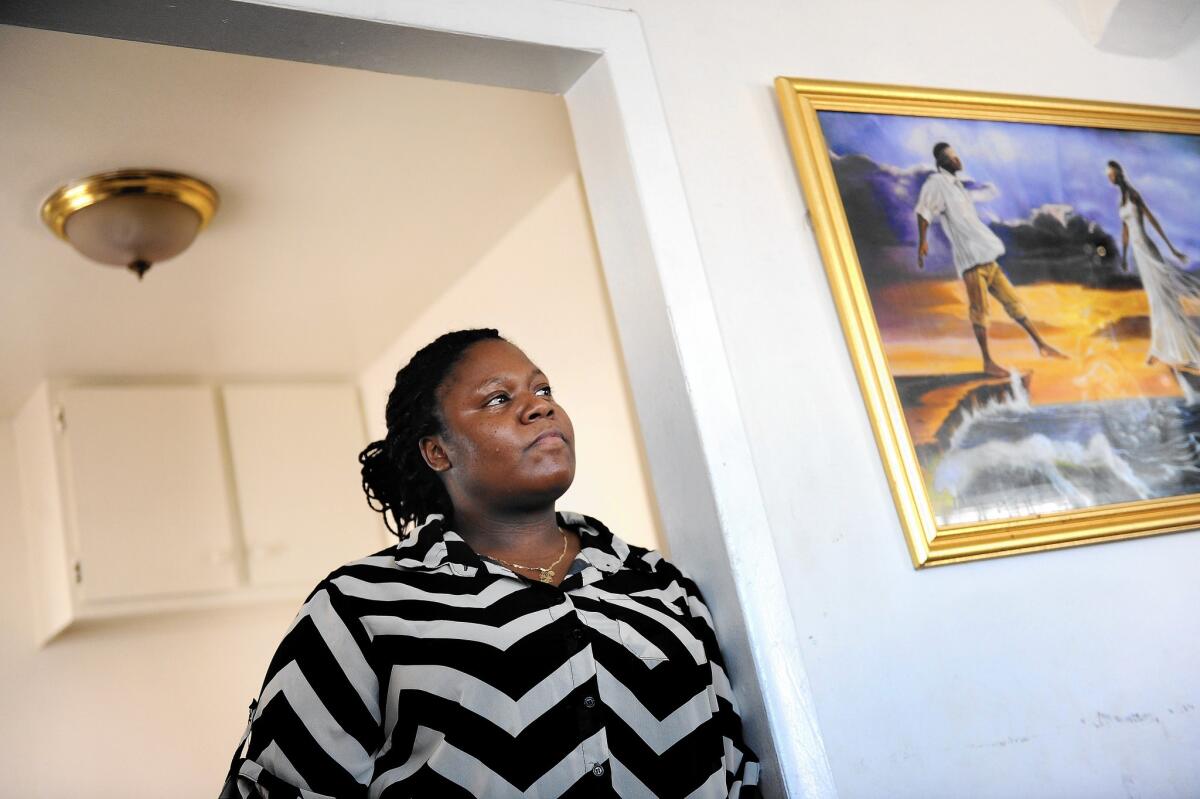
- Share via
Two weeks after her son was hospitalized with pneumonia, Stacy Dorton received a surprise bill saying she owed $700 that her insurance didn’t cover.
“I knew it was a mistake,” said the 31-year-old Los Angeles mother of four.
And she was right.
That’s because Dorton and her son are among the 12.5 million Californians — nearly one-third of the state’s population — covered by Medi-Cal, California’s insurance program for people with low income. Healthcare providers are prohibited by law from billing people with Medi-Cal for charges not covered by their insurance.
Yet, advocates said there has been an increase over the last year in healthcare providers engaging in the practice, commonly referred to as balance billing.
“We get a significant number of people with Medi-Cal being impermissibly balance billed,” said Stephanie Lee, supervising attorney at the Neighborhood Legal Services of Los Angeles County’s health consumer center, which offers free legal advice.
Balance billing is particularly prevalent among a vulnerable subset of Medi-Cal recipients — those who also qualify for Medicare, the federal health program for seniors and disabled people. Folks who qualify for both are referred to as dual eligibles.
A recent report by the federal Centers for Medicare and Medicaid Services revealed a nationwide trend of healthcare providers illegally billing these individuals for charges not covered by either type of insurance.
In California, Lee said, the call volume on her organization’s help line doubled in the last year in large part because of complaints about balance billing among people with Medi-Cal.
“The services these patients get should be free, and then they get a nasty surprise,” Lee said.
The problem stems, in part, from providers and patients who “don’t understand what the protections are,” said Georgia Burke, directing attorney with Justice in Aging, a national organization that works to fight poverty among seniors.
A doctor who agrees to care for a patient covered by Medi-Cal alone is required to accept Medi-Cal’s reimbursement as payment in full. For dual-eligible patients, healthcare providers must accept as payment in full whatever Medicare and Medi-Cal together pay for the service.
But Burke said that doctors who regularly treat patients with Medicare but who don’t take Medi-Cal, will often tell dual-eligible patients, “I don’t take Medi-Cal and I need to be paid.”
What many doctors don’t understand is that even if they aren’t part of the patient’s Medi-Cal plan network, they still should submit bills to the program for balances not paid by Medicare. But doctors can’t charge patients for any remainder still owing after both plans pay.
Eliza Landfair, 72, of Los Angeles has both Medicare and Medi-Cal coverage. In the middle of treatment for lung cancer, her doctor told her he didn’t accept Medi-Cal and charged her $208 for the cost of chemotherapy that Medicare alone didn’t cover.
Despite the fact that she was charged illegally, Landfair borrowed the money from her cousin to pay.
“Frequently beneficiaries pay the bill out of their very limited income,” said Kata Kertesz, policy attorney with the Center for Medicare Advocacy Inc. in Washington. “Some may choose to forgo the care that they need because they are concerned that the bill will go to collections, which is too often the case, and they know that they are unable to pay.”
Landfair had to switch doctors in the middle of cancer treatment and went five months without medical care until she found a new physician.
“It’s very upsetting,” she said.
The California Department of Health Care Services said it is drafting a bulletin that makes the law clearer to doctors.
In the meantime, experts offer suggestions for people with Medi-Cal coverage and what to do if they get a bill.
Show your card upfront. “Make sure you show your Medi-Cal card to your provider ahead of time,” Lee said. Being clear about your coverage upfront can prevent problems in the long run, she said.
Even if you fail to do so, state law protects anyone with Medi-Cal against balance billing. “You shouldn’t be billed,” Burke said.
Call your doctor’s office. If you get a bill, contact your doctor’s office to confirm they have all of your insurance information. “That can resolve it quickly,” Lee said.
Also, be clear that billing Medi-Cal patients for any balance not covered by insurance is a violation of the law.
Don’t ignore bills. Providers regularly send outstanding bills to collections, which can wreak havoc on your credit. Don’t ignore notices.
“When you get something that looks like a bill, address it as quickly as possible. Once it goes to collections it’s harder to deal with,” Lee said.
Get help. If you can’t resolve a billing issue on your own, get help.
The Medi-Cal Ombudsman can help members with billing matters. Call (888) 452-8609 or send email to MMCDOmbudsmanOffice@dhcs.ca.gov
The California Department of Managed Health Care Help Center offers assistance at (888) 466-2219 or online at www.HealthHelp.ca.gov.
Neighborhood Legal Services of Los Angeles County’s Health Consumer Center provides L.A. County residents with free advice and legal services. Attorneys can be reached at (800) 896-3202
Outside of L.A. County, call the Health Consumer Alliance statewide line at (888) 804-3536 or visit Healthconsumer.org.
Dorton worked fast to get her $700 hospital bill dismissed. She could have done without the extra stress while dealing with a sick child. “I went to the hospital thinking he has Medi-Cal. It was supposed to be taken care of.”
Twitter: @lisazamosky
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.










