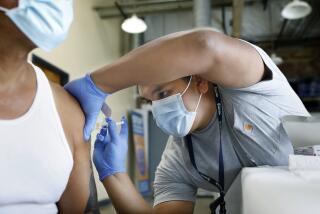
L.A. County’s tracing team repeatedly failed to detect coronavirus outbreaks at workplaces

- Share via
One by one workers at the Farmer John pork processing plant began getting sick with the coronavirus in March.
Public health officials had created a system to help contain such outbreaks: The county’s fast-expanding army of contact tracers would be notified within 24 hours of people who tested positive for the virus. The county workers would call the patients, make sure they were isolated and determine who else they may have infected.
But the tracers never found the epidemic in the plant, famed for making Dodger Dogs.
By the time the county began an investigation in May, at least 116 workers were infected in what had become one of the region’s biggest outbreaks.
It’s been a grim pattern since the pandemic began. The county’s contact tracing system has repeatedly failed to find workplace outbreaks before they spread widely, placing an ever-expanding circle of employees, their families and others at risk.
Los Angeles County has long been the California epicenter of coronavirus, but in the last two months, the region has seen rapid spread in workplaces as the economy reopened. That prompted officials to scale back reopenings, a wrenching blow to a city suffering 20% unemployment.
And many experts agree that economic life is not going to get back to normal until contract tracing dramatically improves and officials gain a better sense of how COVID-19 is spreading.
The county’s program, designed for swift identification of those swept up by the pandemic, has been throttled time and again by slow turnaround times for test results from labs, language barriers, uncooperative employers, as well patients who provide inaccurate or incomplete information, most significantly about their workplaces, officials said. Many of those getting sick are low-wage workers who fear financial ruin if they stop working and are too afraid of retaliation to report unsafe work conditions.
The number of people testing positive who tracers have been able to reach has fallen to 68% in recent weeks, down from 75% earlier in the pandemic, according to officials. And only 40% of those people have been willing to disclose who they may have exposed.
“We believe this is because people are fearful of losing their housing, their jobs and their relationships,” said Los Angeles County Public Health Director Barbara Ferrer.
Getting information has been so difficult that the county recently began offering $20 gift cards to people who agree to be interviewed.
To compensate for the system’s weaknesses, the county now requires employers to report outbreaks when three or more workers test positive. But so far officials have done little to enforce that reporting requirement, and some companies have failed to comply. Last week, officials said they would begin imposing financial penalties on employers not following the county directives — but not until the end of August.
The consequences of the contact tracing failures are playing out in real time. This month, county officials blamed workplace outbreaks for playing a major role in the recent surge in infections. They said the county was receiving an average of nearly 3,000 cases of positive test results a day — about twice as many as the month before.
In an interview, Ferrer acknowledged her staff has scrambled to keep up as they race to respond to hundreds of outbreaks across the county from a virus that scientists are only still learning about. She called contact tracing “a valuable tool for slowing the spread of COVID-19” but said it “cannot and should not be expected to singlehandedly stop outbreaks in the workplace.”
Many, especially those backed by labor unions, push back against returning to their workplaces, citing employers’ failures to prevent COVID-19 outbreaks.
Ferrer added that the recent surge of cases had made the work of trying to pinpoint the source of infections even more difficult. “With this many new daily cases, it is not possible to connect all of the dots,” she said.
In some places, like South Korea and Germany, however, aggressive use of contact tracing has helped to corral the coronavirus. American public health departments have used the technique for decades to control outbreaks of measles, tuberculosis and sexually transmitted diseases. And experts across the country have heralded it as a key to ending the pandemic.
The county rapidly boosted its core force of 250 contact tracers to 1,600 by reassigning and retraining other government employees, according to county documents. They included librarians, who are already skilled at interacting with the public, a key to gaining patients’ trust. With infections surging anew, the county is continuing to add tracers, with 900 more in training.
The workers are aided by a county health order in March that required doctors to immediately report each positive test result to the county, with the person’s name, contact information and occupation.
The tracking is essentially a race against the clock. People who contract COVID-19 are most infectious two days before they first experience symptoms to ten days after, according to federal health officials.
“Ideally, contact tracing is initiated within 48 hours,” said Susan Donelan, an infectious disease expert at Stony Brook Medicine in New York, referring generally to how speed is needed to make the technique most effective. “You try to break the chain of transmission.”
Most of the county’s contact tracers work from home. And it’s unclear whether the county is able to monitor the information on employers that the tracers obtain in their interviews of patients for clusters of infections that could be outbreaks. County officials declined to answer questions about whether a new software system installed in early April to help contact tracers record the interview information could be used to search for outbreaks.
Officials described the contact tracing data system that was in place before the upgrade in April as one that was “paper based.”
Up to 70% of new cases of coronavirus in California’s fertile San Joaquin Valley may be Latino workers, but advocates say they lack testing and access to care.
The failures have many demanding answers.
“I want to know where this is happening,” said Supervisor Janice Hahn in late June. “Where are people getting this? Is it the grocery store? Is it in the churches? Is it the restaurants? Is it at the beaches? Is it riding Metro? Is it at the bars? And that’s more difficult to ascertain. Apparently contact tracing is a difficult procedure to gather all the information you’d like to have.”
Meat-packing workers wait weeks for assistance
The hesitation of patients to reveal their employer to contact tracers is one reason the county did not get an early warning as the coronavirus swept through the Farmer John plant this spring, officials say.
“Many people are very worried about their security at work,” Ferrer said. “It’s just one of the questions that we oftentimes don’t get a complete answer.”
Ferrer also pointed out that her staff had initially decided that officials with the small city of Vernon, where the plant is located, should take responsibility for trying to stop the infections.
The county had learned about the outbreak on April 17, about a month after the first known infections, when Farmer John managers called the city of Vernon to report that six workers had tested positive. Vernon city officials toured the plant and told the county that the company had installed safety measures to stop more infections.
But the cases continued to spread unchecked, according to county documents. And the county’s contact tracers still didn’t find them.
It was another month later, on May 18, that Vernon officials notified the county that the infections had greatly multiplied. By the time county officials sent a press release on May 24 to warn nearby communities, at least 153 workers had tested positive. Dozens of other workers were also infected at eight other nearby food processing plants in Vernon, a small industrial city that has few residents of its own.
Keira Lombardo, an executive at Smithfield Foods, the company that owns the plant, said managers had worked closely with government officials “to help ensure COVID-19 cases among our employees are quickly reported.”
“Everyone with whom they have had close contact ... are notified as soon as possible,” Lombardo said.
The plant’s outbreak has now expanded to 220 workers, according to county documents.
Darryl Blackwell, who works in the plant’s ham-deboning department, where the first employees tested positive, said he and his colleagues initially received little information about the spreading infections. Blackwell said he had wondered why government officials weren’t responding to the outbreak and ensuring employees were safe.
“A lot of people were afraid,” he said. “They fear they will carry it back home to their families.”
Virus spreads with construction of NFL stadium
The county’s contact tracers also failed for months to discover an outbreak at the construction site of SoFi Stadium in Inglewood, where the Rams and Chargers will play.
The first construction worker at the 298-acre stadium site tested positive in late March.
The county health department did not start an investigation until mid-June, and only after Times reporters had asked repeated questions about continuing infections at the site.
The county says that 55 workers have now tested positive, with most of the cases reported in June and July.
Sharon Balter, director of county’s acute communicable disease control program, said the SoFi case showed how contact tracing cannot pinpoint an outbreak at a sprawling work site like the stadium, where 3,000 construction workers are employed by a myriad of subcontractors.
“It’s going to be complicated for us to detect this outbreak until someone reports it to us,” she said.
Chris McFadden, a spokesman for Turner AECOM Hunt, the joint venture overseeing the construction, declined to say whether the joint venture had reported the workers’ infections to the county. Instead he said that the site’s management continued to “meet or exceed” the county’s guidelines.
He said the joint venture has measures in place to keep people safe. He said the site has enhanced cleaning and disinfection and requires workers to keep six feet away from each other. Workers must also have their temperatures checked before entering the site, he said.
If a worker tests positive or has symptoms, McFadden said, “we launch our own investigation to determine who they may have had close contact with.”
Workers die before county learns of outbreak
At the bustling Los Angeles Apparel garment factory in South L.A., infections began in May and surged in June.
But contact tracers didn’t detect the outbreak, which has been the largest in the county so far. A medical professional who became aware of conditions at the plant through a patient notified public health officials on June 19.
The county immediately began investigating, but by then three people had died. More than 150 workers tested positive that same week.
By July 10, when the county alerted the public through a press release detailing the company’s “flagrant” violations of safety rules, more than 300 workers had tested positive and a fourth had died.
Asked why the county’s contact tracers had not found the outbreak, Ferrer repeated her staff’s findings that many people testing positive are afraid to tell the government who they may have exposed.
She said the factory’s managers had put “their employees and their families greatly at risk” by not reporting the outbreak until 150 had tested positive.
But Dov Charney, the founder of L.A. Apparel, said he believes the county’s contact tracers should have been able to detect the outbreak earlier.
“If they were doing contact tracing, they would have found out by case 12,” he said.
Charney said he had repeatedly arranged for his staff to be tested. And under the county’s system, each of those test results would have been quickly sent to government contact tracers.
“When they saw elevated numbers, they should have come in right away,” he said. “They didn’t show up.”
Charney said he had not tried to hide information about the infections.
“Maybe our record keeping wasn’t there initially,” he said, “but it took a while to figure out what they wanted.”
He said the county’s policy of requiring employers to report outbreaks had been confusing. First the county told employers that a cluster of five cases should be reported. More recently, he said, the county had changed the rules, saying that a reportable outbreak was three infections.
“Their directives are not clear,” he said, “and they are buried on a website,” making them hard to find.
Marissa Nuncio, director of the Garment Worker Center, said she began hearing from employees concerned about the infections and unsafe conditions at the factory in May.
By the end of that month, she said, at least one worker was hospitalized.
Nuncio said that some workers testing positive may have been hesitant to disclose their employer to the contact tracers because of concerns of losing their jobs. The factory’s workers also include some who speak Indigenous languages, she said, which could have made communication with the county workers more difficult.
Other employees may have not returned the county’s calls, she said, because of their immigration status. “There can be fear in workers about going to the government if they’re undocumented,” Nuncio said.
Last week, the county announced the creation of a new call center to make it easier for those testing positive to reach the contact tracers, who now work seven days a week from 8 a.m. to 8:30 p.m. The center’s number is 1-833-540-0473.
Ferrer also encouraged employees who see unsafe practices at their worksite to report them anonymously by calling 1-888-700-9995.
“We are doing the best job we can,” Ferrer said.
Staff writers Jaclyn Cosgrove, Dorany Pineda and Nathan Fenno contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.