Nation’s first MPX case in healthcare worker exposed on the job is reported in L.A. County
- Share via
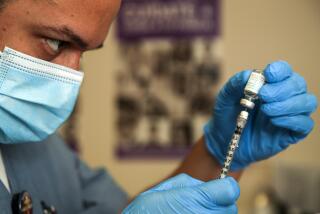
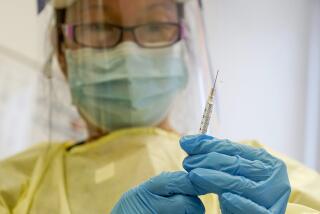
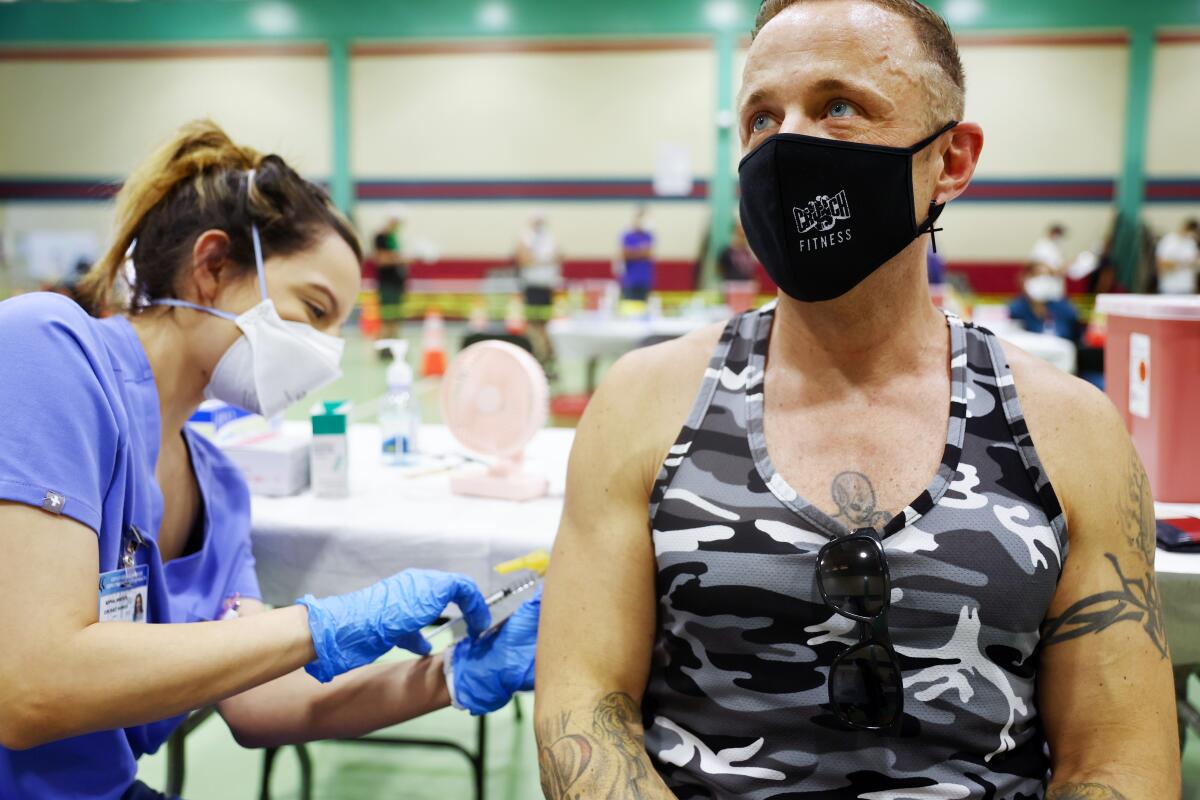
The first U.S. healthcare worker to be infected with MPX while on the job has been reported in Los Angeles County, public health officials said Tuesday, the day after the county confirmed the nation’s first MPX death.
“We have identified a healthcare worker with monkeypox who appears to have been exposed to the virus at their worksite,” Dr. Rita Singhal, chief medical officer for the L.A. County Department of Public Health, said in a presentation to the Board of Supervisors. “This is the first case of monkeypox in a healthcare worker in the United States that has been linked to a worksite exposure.”
Singhal said the county has consulted about the case with Centers for Disease Control and Prevention officials, but the risk of MPX for healthcare workers “remains very low.”
Dr. Rochelle Walensky, the CDC director, told the Senate Health Committee on Wednesday that the lone reported case of an infected healthcare worker was the result of a “needle stick injury.” Walensky did not specifically say she was referring to the L.A. County case.
Walensky expressed confidence that wearing personal protective equipment keeps healthcare workers protected against exposure.
The L.A. County Department of Public Health declined to answer additional questions Wednesday about whether Walensky was talking about the local case reported this week or elaborate on the healthcare worker’s condition.
On Thursday, Singhal said at a news briefing that there have been about eight healthcare workers worldwide who have contracted MPX from workplace exposure, some of whom were infected because of a needle stick injury. “Locally for us here, it was not directly a needle stick injury, but it was an exposure at the work site,” she said.
Spread of the MPX virus to healthcare employees from work site exposures is rare.
Before this year’s outbreak, there was a single documented case of MPX transmission in Britain, in 2018, in which a healthcare assistant was infected after changing “presumably contaminated bedding” without wearing a mask or respirator. The worker came into contact with the sheets at a time when the patient had skin lesions but had not yet been diagnosed with MPX and placed under isolation, according to medical journals.
Editor's Note:
In light of widespread concerns that the name “monkeypox” is racist and stigmatizing, the World Health Organization has renamed the disease “mpox.”
Health leaders in California recently started to use the name MPX, pronounced mpox, because of widespread concerns the virus’ original name is stigmatizing and racist. The World Health Organization is in the process of formally renaming the disease, which will take several months.
MPX — unlike the coronavirus — is not easily transmitted, typically requiring close skin-to-skin contact with an infectious lesion. Cases in this outbreak have been confirmed primarily among men who have sex with men, as well as transgender people, as the virus can spread easily during sexual encounters — though not exclusively.
In L.A. County, 97% of MPX cases have been confirmed in men, and of cases for which sexual orientation is known, more than 90% have identified as gay or bisexual, according to the Department of Public Health.
While MPX case counts reached a total of 1,914 in L.A. County as of Wednesday, the number of new cases week-to-week has recently started to fall, a sign public health leaders across the nation are hopeful indicates reduced transmission and a sustained decline in cases. There are 4,453 confirmed or suspected cases across California.
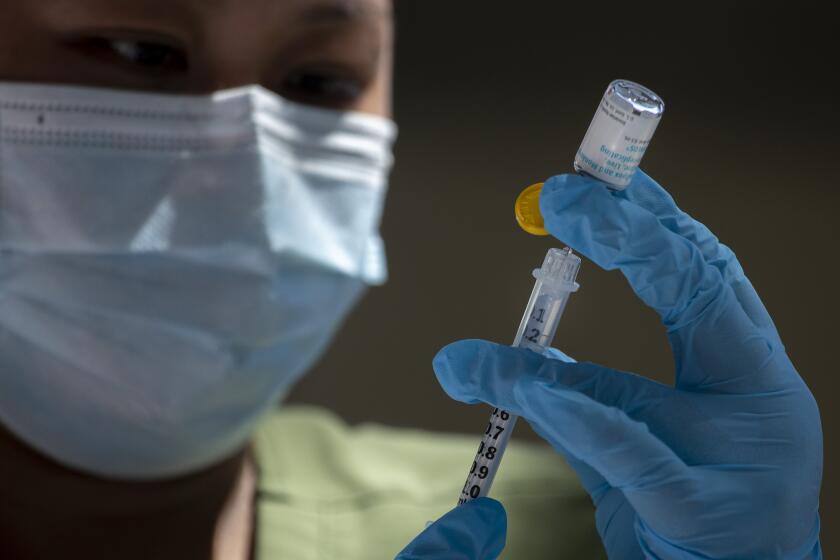
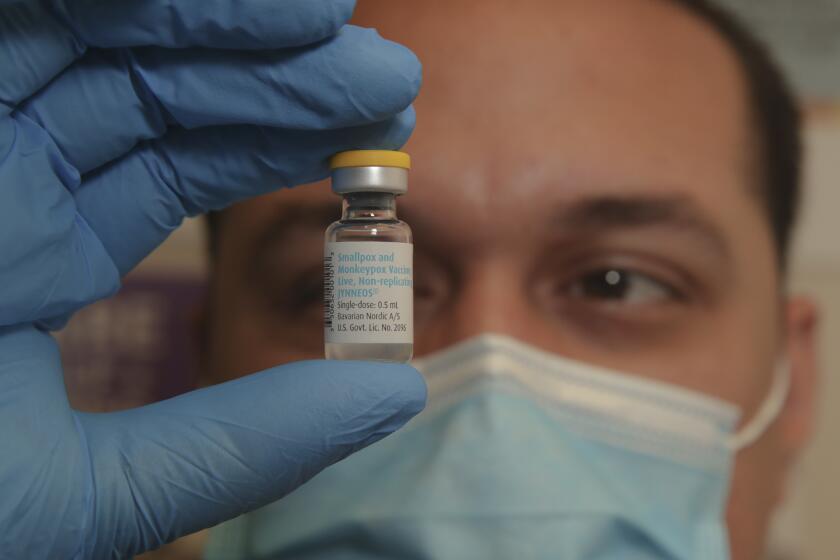
But even as the rate of new cases slows, Singhal said disparities are growing among who is catching the virus and receiving the two-dose Jynneos vaccine.
A Los Angeles County resident has died due to monkeypox, also known as MPX — the nation’s first confirmed fatality linked to the disease.
In July — at the beginning of the local outbreak — white Angelenos made up more than 55% of new weekly MPX cases, according to data from the Public Health Department shared Tuesday. But by early September, Latino residents made up the largest proportion of MPX cases in the county, with about 55% of all new weekly cases. White residents’ share had shrunk to about 20% of new weekly cases in early September, while Black residents’ share had almost doubled in two months, to about 10%.
Accounting for population, county officials found that Black Angelenos had the highest rate of cumulative MPX infections, at 26 cases for every 100,000 Black residents, while Latino residents and white residents had similar case rates, at 16 and 17 per 100,000, respectively.
Using the Healthy Places Index, or HPI — a measure that accounts for the overall public health level of a community, such as poverty and access to housing and education — county officials found that neighborhoods with the least resources have accounted for a larger share of the county’s total MPX cases: about 70% as of early September.
New monkeypox cases are starting to flatten in Los Angeles County, echoing a trend seen elsewhere as more vaccination doses are distributed and some people are reducing riskier sexual activity.
“Over time, a higher proportion of cases have been in the two lowest HPI quartiles, or the least healthy communities,” Singhal said. At the beginning of the outbreak, people living in communities with fewer resources for optimal public health made up roughly 30% of MPX cases, while those in communities with greater resources were initially more likely to contract the virus. But that flipped about two months later.
People of color have also disproportionately not received a vaccine against MPX, despite making up a majority of current cases, according to county data from last week. Latino residents make up 44% of MPX cases but only 32% of first-dose recipients; similarly, 12% of county cases are among Black residents, but only 9% of the administered first doses have gone to that demographic.
White Angelenos make up 40% of the county’s first-dose recipients, though they account for less than 30% cases, the data show.
“To address the disparities in monkeypox case and vaccination rates among Latinx and Black populations, [the Department of] Public Health is working with community-based organizations to further define messaging and outreach for these populations,” Singhal said. “We are meeting with stakeholders on a weekly basis to hear feedback from focus groups on how best to reach these populations.”
Singhal also noted that only one-third of those eligible for a second dose of the MPX vaccine have received it, and she strongly encouraged people to get both shots to “optimize their immune response.”
Barbara Ferrer, the county’s public health director, said she is hopeful the agency’s recent expansion of vaccine eligibility to include people who self-attest they may be at “risk for future exposure” will also help bring more people in for a shot.
How monkeypox spreads, how to get a vaccine and more: Your frequently asked questions about monkeypox, and answers from experts.
Due to an initial shortage of doses, the county limited doses to those considered most at-risk to the virus — primarily gay and bisexual men or transgender people with certain sexually transmitted infections or multiple sexual partners — which she acknowledged could have been stigmatizing. Vaccine availability has since drastically increased, though officials are still not recommending widespread inoculations.
“We’ve changed our eligibility guidance to really make that much easier to people,” Ferrer said Tuesday. “We’re trying desperately to listen to concerns residents are raising. ... We do have disproportionality; we need to pay a lot of attention to what people in our communities are saying would help reduce the barriers to getting vaccinated.”
Singhal also reported two MPX cases that have been confirmed in county jails and 81 among people experiencing homelessness, including seven in congregate housing, but she said there is “no evidence of spread in those settings.” There have been six cases in children under the age of 18.
Throughout the entire outbreak, 66 people have been hospitalized for MPX, Singhal said, or about 4% of total cases. The person who recently died of MPX in L.A. County was “severely immunocompromised and had been hospitalized,” Singhal said, and she urged those with MPX to seek medical care and treatment early, when possible.
Times staff writer Rong-Gong Lin II contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.