Demystifying the cardiac stress test
- Share via
Dr. Marc Wallack routinely passed his cardiac exercise stress test with flying colors. He was, after all, a veteran marathon runner with respectable cholesterol and blood pressure numbers.
But as many heart disease patients discover, a treadmill analysis often isn’t enough. Six months after a “normal” stress test, surgeons cracked open Wallack’s chest for quadruple bypass surgery. An artery was 95% blocked.
“I thought I understood heart disease,” said Wallack, a New York City surgical oncologist who has a strong family history of the illness. But his most recent stress test looked fine. So like many men, he convinced himself that the chest pain was merely heartburn.
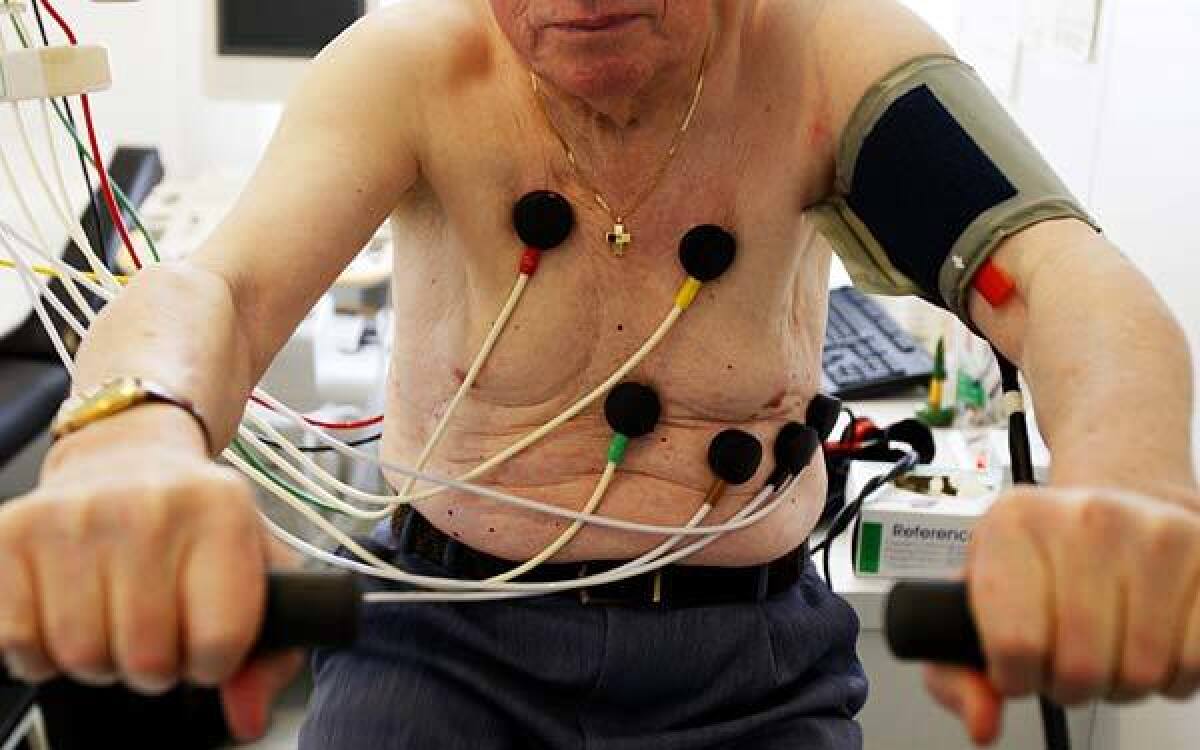
Cardiac stress tests, also called exercise or treadmill tests, are commonly used to find evidence of blockages in the arteries of the heart. They’re noninvasive — require no surgery or needles — are as easy as walking up a slight hill on a treadmill or riding a stationary bike and can be done in a doctor’s office.
For people with chest pain, a positive result can determine whether the problem is heart-related. Stress tests can also evaluate heart risk before a surgery or after a heart attack. And doctors use them to jump-start exercise programs for sedentary patients.
But accuracy is a concern. Exercise stress tests are only about 60% effective, meaning they miss 40% of the problems, said cardiothoracic surgeon Kathy Magliato, director of cardiac services at St. John’s Health Center in Santa Monica.
They’re even less accurate for women than for men, possibly because when women have heart disease, the smaller branches of the blood vessels are often affected, Magliato said. Breast tissue can trigger false negatives. Other factors, including sex or stress hormones or estrogen’s effect on the cells of the heart muscles, can also come into play.
“We don’t have the perfect test for heart disease,” Magliato said.
The dilemma
The high rate of false positive and false negative results doesn’t just add to a patient’s anxiety; it often leads to more invasive procedures and the unnecessary use of medications, said Dr. Michael LeFevre, a professor of family and community medicine at the University of Missouri School of Medicine in Columbia. The wrong results can also give people a false sense of security or lead to a delay in treatment.
As a result, the U.S. Preventive Service Task Force does not recommend treadmill testing for those with a low risk. For high-risk populations, there’s not enough evidence for — or against —- screening adults with treadmill testing, the agency said.
After someone has taken a stress test, “a cascade of things can happen, and we don’t have the information that people lived longer or better because we initiated the cascade,” said LeFevre, who helped write the task force’s 2004 guidelines.
Stress tests can effectively show whether the heart’s arteries are 70% narrowed or more. But heart attacks can arise from arteries that are less than 50% blocked. This seems counterintuitive: Doesn’t the artery gradually narrow because of progressive fat deposits that block the artery until blood is cut off?
Not always. Heart attacks arise from what cardiologists call a “vulnerable plaque,” which can be thought of as a pimple in the artery. These pimples can suddenly erupt — no one knows why — releasing chemicals from the artery that trigger a blood clot. “It’s possible for a plaque to evolve from a 20% narrowing to a complete blood clot — causing a heart attack — in a matter of minutes,” said preventive cardiologist Steve Devries, an associate professor at Northwestern Memorial Hospital in Chicago.
The only way to uncover the pimples or large fat deposits in the arteries is through an invasive procedure called an angiogram, in which a thin ultrasound tube is inserted into the artery of the heart. But even this procedure isn’t foolproof; moreover, it would never be given to a runner without symptoms.
Your best bet
Given the shortcomings of the treadmill test, the task force, which is reviewing the current guidelines, says prevention is a key strategy. That means reducing the risk factors, including high blood pressure, obesity, diabetes and high cholesterol.
It’s also critical to know the symptoms: chest pain, pressure, tightness or unusual shortness of breath that lasts more than five to 10 minutes. If the symptoms occur when you exercise and dissipate when you stop, it’s a sign something is wrong.
For 50% of women with heart disease, however, chest pain never appears. Instead, they’re fatigued or have indigestion or upper abdominal or jaw pain.
Wallack, who ran a marathon after his open-heart surgery, still gets his annual stress test. But it’s even more important to pick the right cardiologist, he said. “If you have a heart history, are hypertensive or have high cholesterol or diabetes, choose carefully,” he said. “A cardiologist becomes a key person in your life.”



