How doctors are using a patient’s own immune systems to combat cancer
- Share via
Chimeric antigen receptor T cell (CAR-T) therapy involves removing some of a patient’s immune system cells, known as T-cells, and genetically reprogramming them in a laboratory to attack cancer cells.
White blood cells, including T-cells, are filtered out of a patient’s blood.
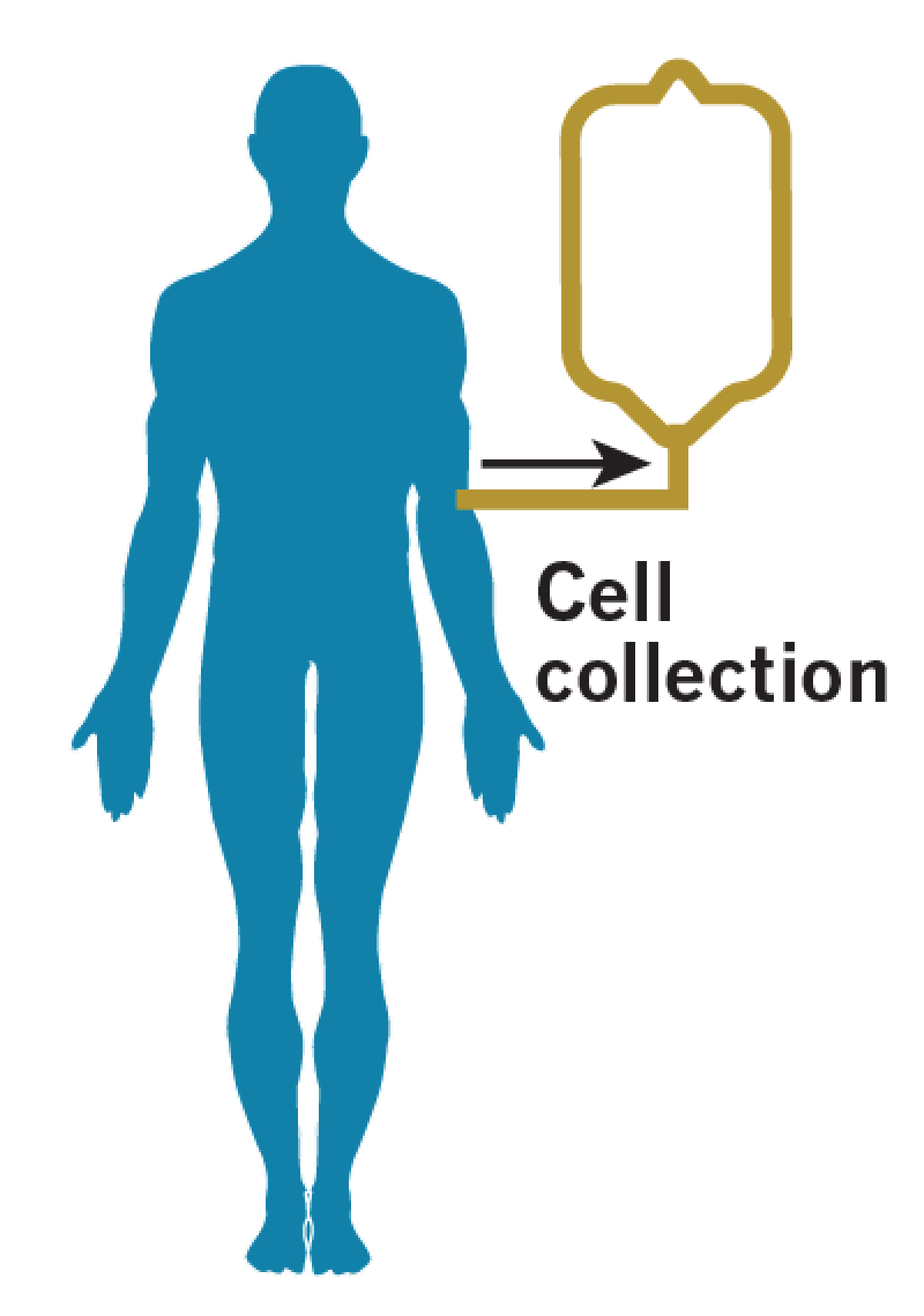
T-cells are frozen and sent to a lab, where they are genetically reprogrammed to help them recognize and target cancer cells
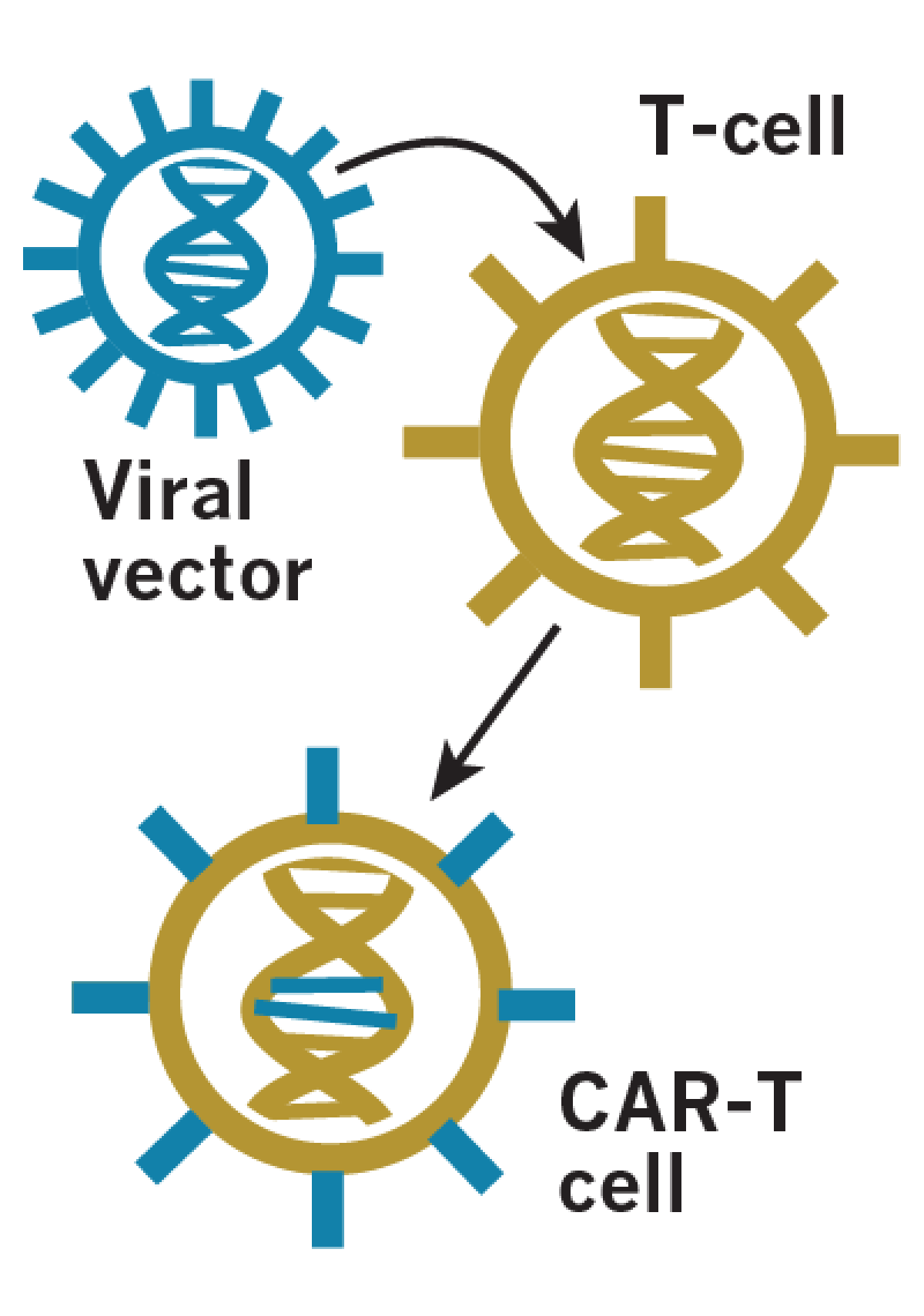
The newly created CAR-T cells are copied millions of times, then quality-checked before being sent back to the patient.
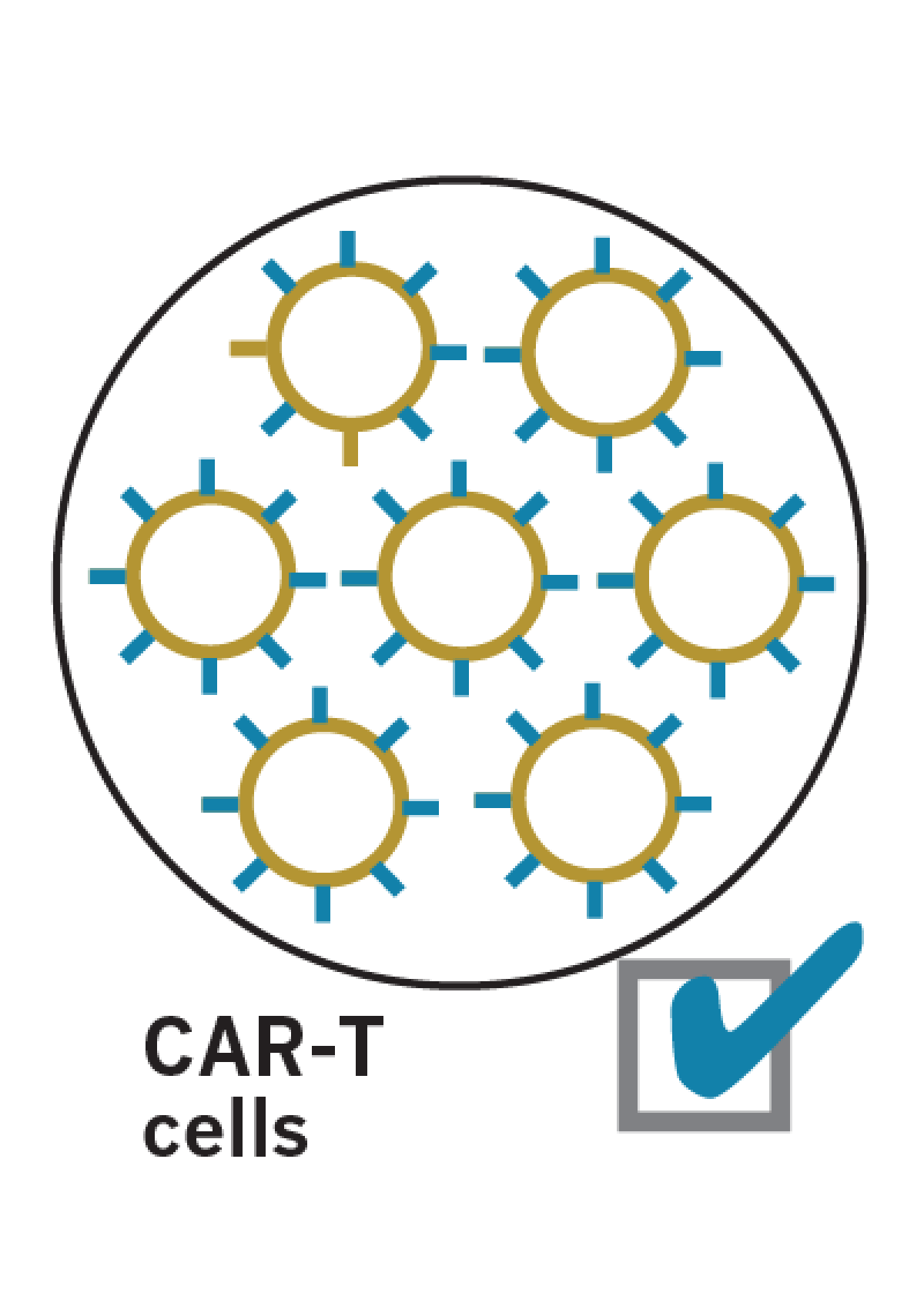
The patient receives chemotherapy to reduce the patient’s regular white blood cells and make him or her more receptive to the reprogrammed CAR-T cells.
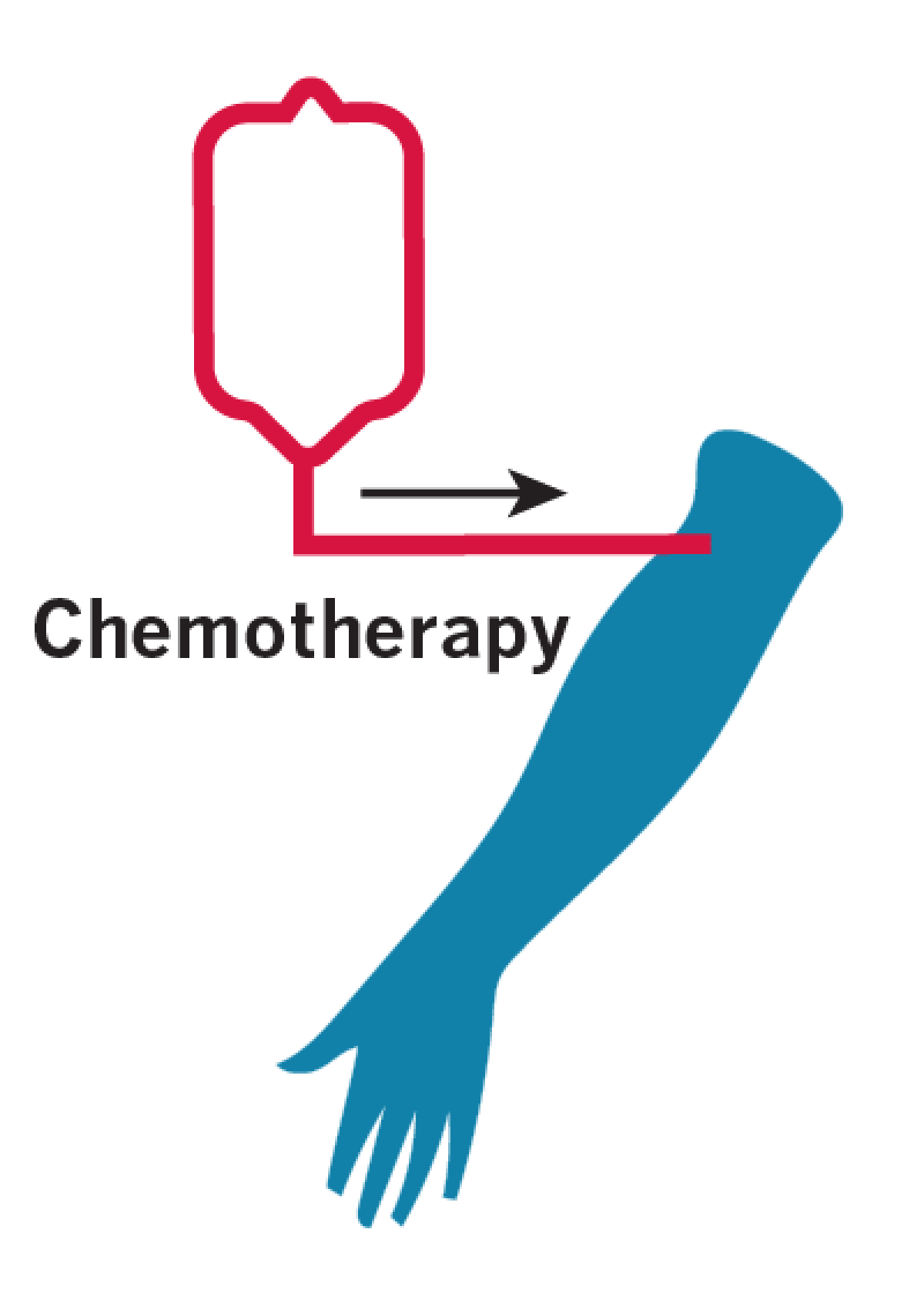
The patient receives a transfusion of the reprogrammed CAR-T cells.
In the body, CAR-T cells recognize the patient’s cancer cells by looking for a specific antigen on the surface. Once found, they attach to them and induce self-destruction.
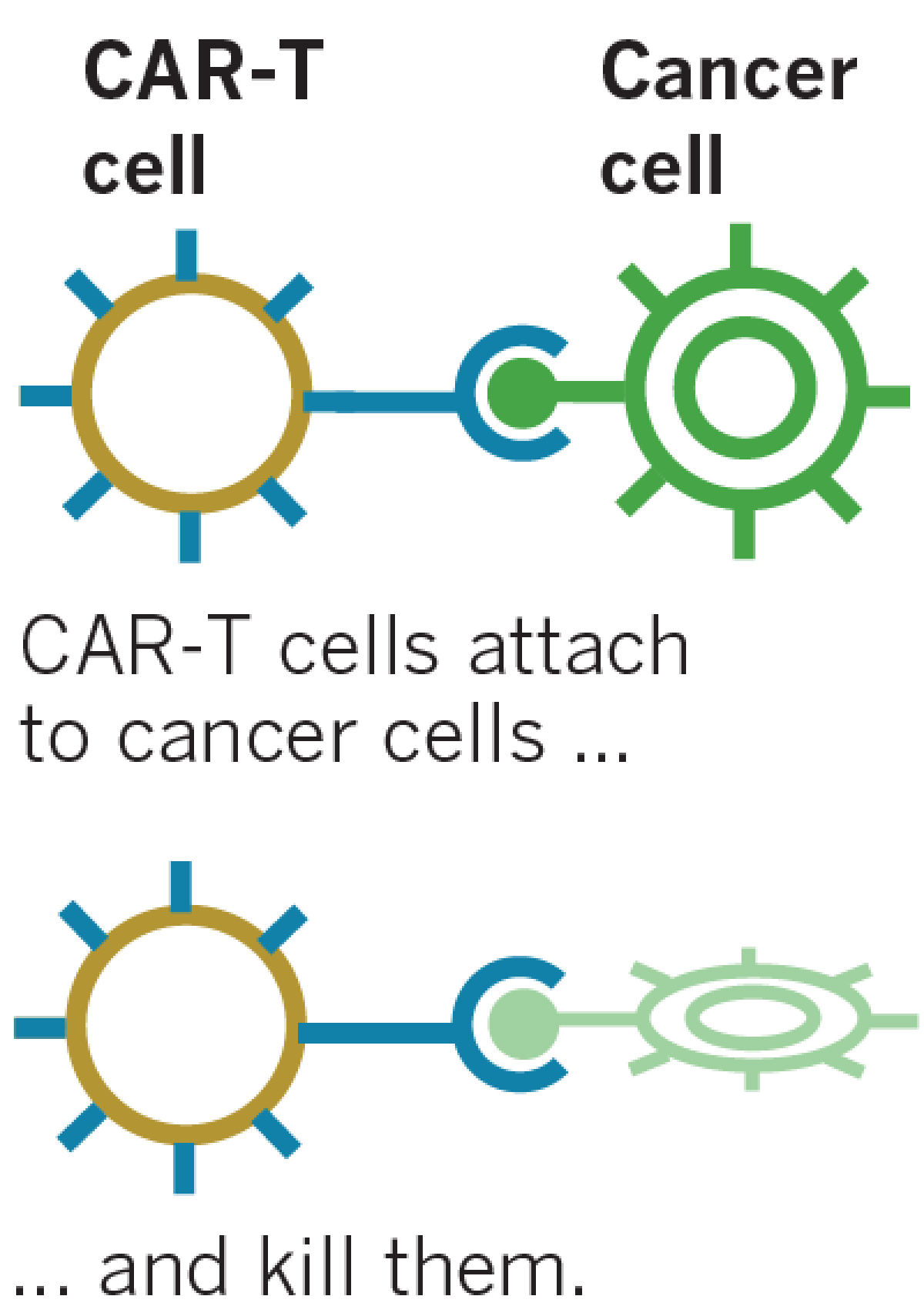
Sources: Novartis, NPR, Times reporting




