Obama to drug-resistant superbugs: We are coming after you
- Share via
The Obama administration is taking fresh aim at antibiotic-resistant superbugs, a growing cadre of microscopic foes that threatens to undermine public health and economic security throughout the world.
The White House on Friday unveiled a five-year plan to fight these deadly pathogens. Part of the strategy depends on slowing the spread of these bacteria by being more judicious in prescribing and using antibiotics. It also counts on scientists to develop new drugs that can replace antibiotics that are no longer effective.
Each year, more than 2 million Americans are sickened by these superbugs and about 23,000 die as a result, according to the Centers for Disease Control and Prevention. The World Health Organization has warned that drug-resistant bacteria are on the rise in every part of the globe.
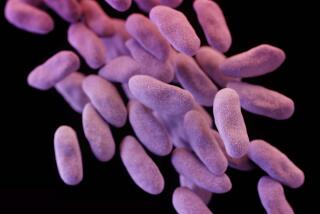
The recent outbreak of carbapenem-resistant Enterobacteriaceae, or CRE, tied to contaminated duodenoscopes at Ronald Reagan UCLA Medical Center is just one example of the problem. As many as half of people infected with CRE may die.
“Antibiotic resistance is one of the most pressing public health issues facing the world today,” President Obama said in an interview with WebMD. “Effective antibiotics are vital to our national security. … They are, quite simply, essential to the health of our people and people everywhere. So we should do everything in our power to ensure that antibiotics remain effective.”
The White House has signaled its seriousness about shoring up antibiotics before. In September, the president signed an executive order calling drug-resistant bacteria an urgent threat and directing the secretaries of Defense, Agriculture, and Health and Human Services to come up with a plan to fight them. And the administration’s proposed budget for 2016 would double federal funding for efforts aimed at fighting antibiotic resistance.
The 62-page National Action Plan for Combating Antibiotic-Resistant Bacteria released Friday lays out five prongs to the assault. These are:
Getting smarter about using antibiotics. Up to half of all antibiotics taken by Americans should never have been prescribed in the first place, the CDC says. In agriculture, antibiotics are routinely used to speed the growth of livestock. Both of these practices must change, according to the report.
Agricultural use of medically important antibiotics for growth promotion should be eliminated by 2020, the plan states. In people, inappropriate antibiotic use should be cut by 20% in hospitals and by 50% in other medical settings by the same target date.
To keep better tabs on the scope of the problem, all 50 states should establish antibiotic resistance prevention programs that will monitor the spread of superbugs within their borders and assist healthcare facilities in fighting them.
Step up surveillance efforts. The administration will establish a network of regional laboratories that test bacteria for antibiotic resistance and create a repository of specimens that are. Hospitals that treat Medicare patients or are operated by the federal government through the Department of Veterans Affairs or the Department of Defense will share data on antibiotic resistance through the CDC’s National Health Safety Network.
In addition, antibiotic resistance among pathogens in animals will be tracked by members of the National Animal Health Laboratory Network and the Veterinary Laboratory Investigation and Response Network.
Recognize bacteria — and especially superbugs — more quickly. By 2020, scientists should come up with tests that can very quickly determine whether a patient’s infection is caused by bacteria or a virus. That will help doctors cut way back on inappropriate antibiotic prescriptions, which are of no help to patients and which help fuel drug resistance. These tests should be deployed by 2020, according to the plan.
Scientists should also develop tests that can rapidly establish whether bacteria are resistant to any antibiotics.
Accelerate research on new antibiotics. It has been decades since a new antibiotic has joined the medical arsenal. In January, researchers announced the discovery of a microbe that lives in dirt and produces a compound capable of killing methicillin-resistant Staphylococcus aureus (MRSA), tuberculosis and other bacteria that are no longer susceptible to some of the most powerful drugs in use today. Still, even if all goes well, it could take two years to begin clinical trials and five years to get it to pharmacy shelves, the researchers said.
In the next five years, at least two new antibiotic candidates — or potential alternatives such as probiotics or vaccines — should be ready for clinical trials to see whether they are safe and effective in people, the plan says. To help make this a reality, the federal government will create a biopharmaceutical incubator to promote collaboration between universities and private companies.
Cooperate more with international partners. The U.S. will forge stronger ties with health ministries and institutions around the world to keep better tabs on superbugs. That includes detecting them, tracking their spread and analyzing their evolution, especially in ways that allow them to thwart antibiotics.
As part of this effort, the U.S. will work with low- and middle-income countries to help them develop their own plans to fight antibiotic resistance, the plan says.
“There are parts of this plan that we can implement on our own right now, and wherever we can act without Congress, we will,” Obama said in the WebMD interview. “But to get the whole job done, we need Congress to step up.”
For more medical news, follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.