Back pain: Doctors increasingly ignore clinical guidelines
- Share via
Doctors have increasingly ignored clinical guidelines for the treatment of routine back pain by prescribing powerful and addictive narcotics instead of other recommended painkillers and by recommending unwarranted diagnostic imagery, according to a new study.
Researchers at Massachusetts’ Beth Israel Deaconess Medical Center and Harvard Medical School based their conclusion on an examination of roughly 24,000 cases of spine problems in national databases from 1999 to 2010. Their findings appeared online Monday in JAMA Internal Medicine.
“Well-established guidelines for routine back pain stress conservative management, including use of nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen and physical therapy,” wrote lead author Dr. John Mafi and his colleagues.
Despite these guidelines, researchers found that doctors were doing much the opposite.
Although physical therapy referrals remained steady during the study period, prescriptions for narcotic painkillers jumped 51%. Simultaneously, prescriptions for non-opiate drugs had fallen by the same amount.
Study authors noted that a 2007 analysis found that narcotics provided little to no benefit in cases of acute back pain and that they had also failed to prove effective in cases of chronic back pain.
The jump in narcotic prescriptions therefore raised “significant concerns,” the authors wrote, and may be linked to a larger national crisis involving prescription drug deaths.
“Although we lack adequate data to make firm recommendations on narcotic medications, which may be indicated in certain instances, such increases in narcotic prescriptions may be contributing to a current crisis in public health: The rapid increase in narcotic overdose deaths parallels a reported 300% increase in the U.S. sales of prescription narcotics since the 1990s.”
Researchers also identified “an inappropriate increase” in the use of “low value” diagnostic imaging that could lead to future cancer in patients because of exposure to ionizing radiation.
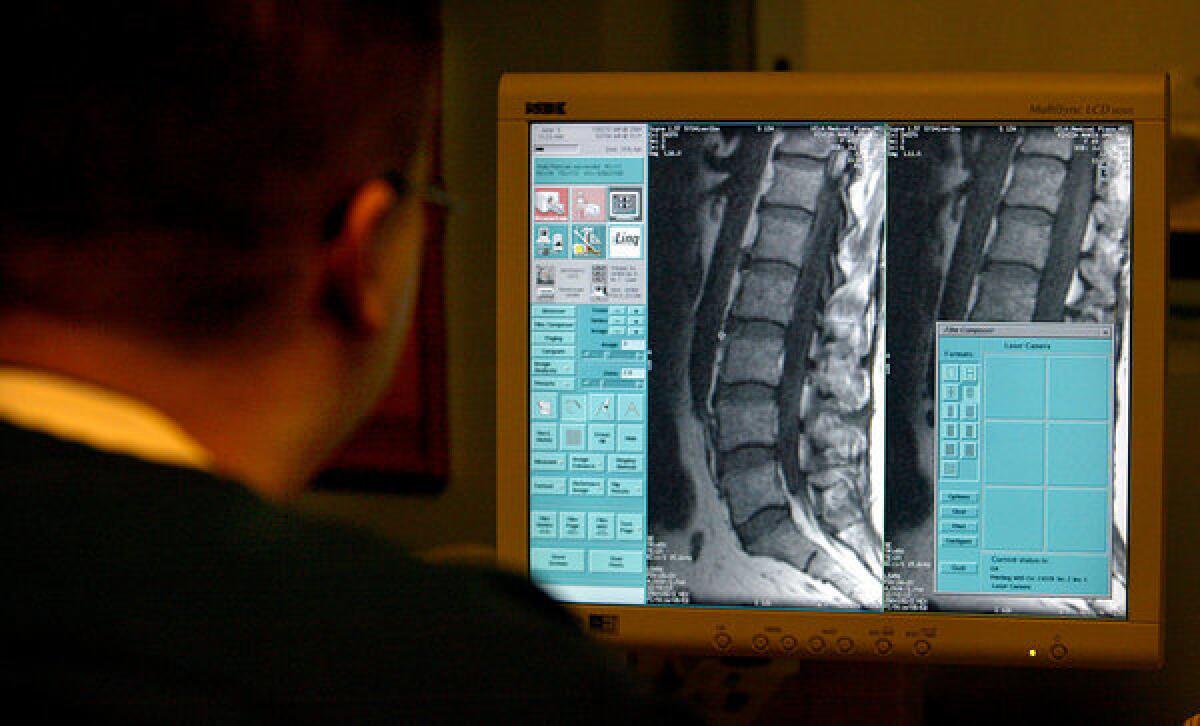
While medical guidelines recommended that doctors avoid early imaging or other aggressive treatments, except in rare cases, researchers found that the use of computed tomography (CT) or magnetic resonance imaging (MRI) had increased by 57%.
Researchers say that such scans have proved to be of little benefit to patients who lack “red-flag symptoms” and that overuse of the technology has been identified in previous studies as well.
“In 2007, a projected 1,200 additional future cancers were created by the 2.2 million lumbar CTs performed in the United States,” the authors wrote.
The authors say that under established treatment guidelines, routine back pain will usually improve within 3 months.
However, referral rates to other doctors, presumably for surgery, had doubled during the study period. (Early MRI for acute back pain was associated with an eight-fold increased risk of surgery, researchers found.)
“The 106% increase in referrals to other physicians is a previously unrecognized and important finding because such referrals likely contributed to the recent increase in costly, morbid and often ineffective outpatient spine operations observed in other studies,” the authors wrote.
Nationally, back and neck problems are responsible for more than 10% of all visits to primary care physicians and account for $86 billion in healthcare spending every year.
According to study authors, spending on these conditions has increased more rapidly than overall health expenditures from 1997 to 2005.
“With healthcare costs soaring, improvements in the management of back pain represent an area of potential cost savings for the healthcare system while also improving the quality of care,” the authors concluded.
Return to Science Now blog.
Follow me on Twitter @montemorin




