Suicides have increased by more than 30% since 1999 in half the states, CDC says
- Share via
More than a decade of steadily rising rates have made suicide the nation’s 10th leading cause of death and one of only three causes of death — including Alzheimer’s disease and drug overdoses — that are increasing in the United States, according to the Centers for Disease Control and Prevention.
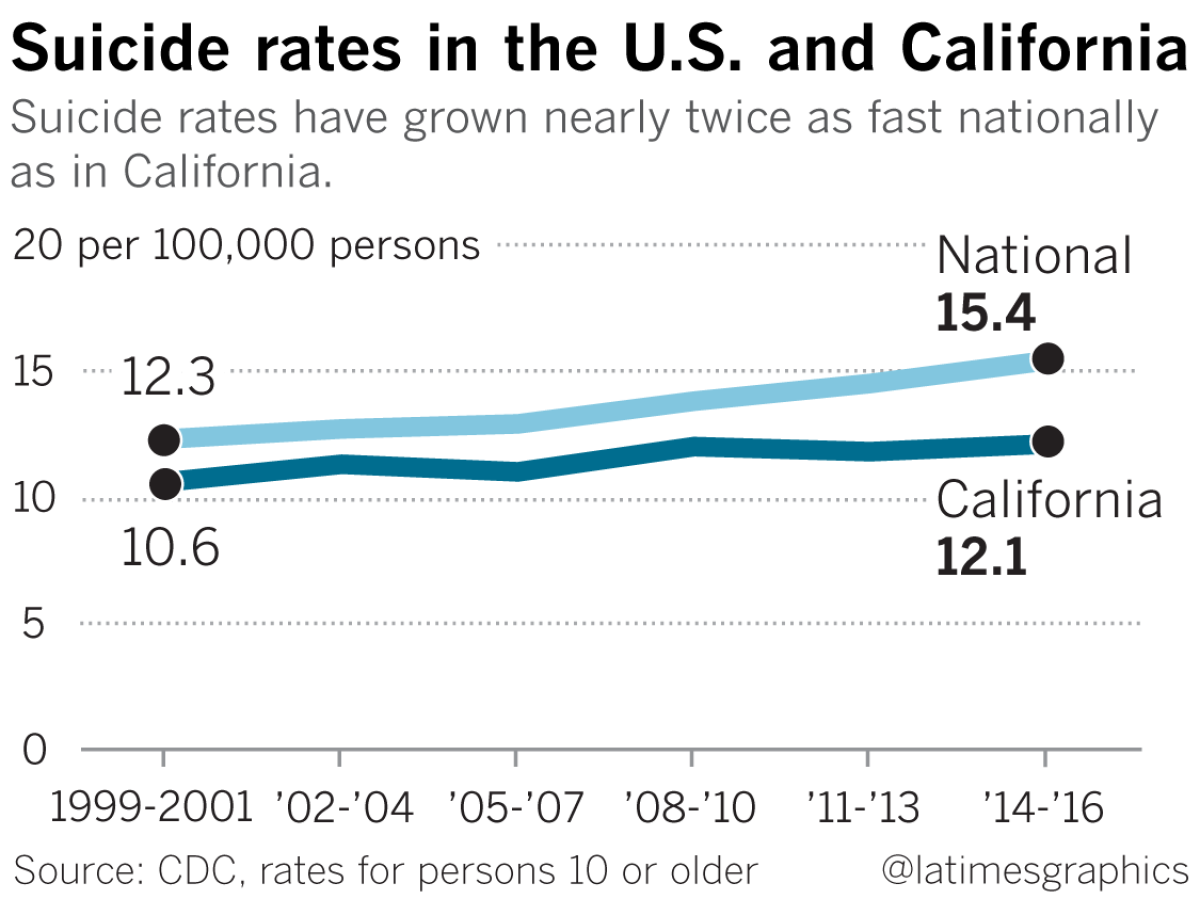
In a report that examines trends in suicide at the state level from 1999 to 2016, the CDC reports that suicide rates have increased in nearly all states. In half of the states, the agency found the rate at which people took their own lives rose more than 30%.
In releasing the report, one day after fashion designer Kate Spade was found dead by suicide in New York, CDC officials underscored that more than half the people who died by suicide — 54% — did not have a known diagnosed mental health condition at the time of their death.
A study that examined suicide trends in 27 states found that in many cases, victims acted after experiencing relationship problems or loss; substance misuse; physical health problems; or job, money, legal or housing stress.
“Our data suggests suicide is more than a mental health issue,” said Deborah M. Stone, the lead author of the new study.
Noting that suicide is “very rare” among those with chronic depression, Stone added that while depression sufferers should “get the care they need,” friends, families and co-workers should not overlook the risk of self-harm among those who have never been diagnosed with mental illness.
On Thursday, public health officials urged people with suicidal thoughts to seek help by contacting the National Suicide Prevention Lifeline: (800) 273-8255. They also stressed that Americans should learn the warning signs of suicide so they can recognize those at risk of harming themselves.
Among the agency’s recommendations: Reduce access to lethal means of ending a life — such as medications and firearms — among people at risk.
“From individuals and communities to employers and healthcare professionals, everyone can play a role in efforts to help save lives and reverse this troubling rise in suicide,” said Dr. Anne Schuchat, the CDC’s principal deputy director.
In 2016, nearly 45,000 Americans 10 or older died by suicide. The increases were particularly stark in the states in the intermountain West, including Idaho, Montana, Wyoming, Utah, North and South Dakota, Kansas, Minnesota and Oklahoma. Between 1999 and 2016, suicide rates in these states (as well as in Vermont, New Hampshire and South Carolina) rose between 38% and 58%.
Roughly half of the suicides in 2016 were carried out with a gun, a number that remained steady across the period studied. Suffocation, including hanging, was the next most common method of suicide, followed by poisoning.
Opioids were present in 31% of individuals who died by suicide. While Stone acknowledged that a person’s intentions are not always clear when drugs of abuse are present, these were deemed to be suicides in which self-inflicted poisoning was considered the cause of death.
In a closer look at suicides in 2015, CDC researchers found that 29.4% took place within two weeks of a crisis — most commonly a breakup or other problem related to an intimate-partner relationship. Among the less-common factors presumed to have contributed to the suicides studied were physical health problems, legal difficulties, a family relationship issue or a job-related problem.
In a 2016 report, the CDC found that suicide rates in the United States jumped 24% in the years between 1999 and 2014. That rise was driven by stark increases in the numbers of white women and Native Americans who are taking their own lives.
In the age group of greatest vulnerability for suicide — between 45 and 64 — that report found that rates of suicide among women in 2014 vaulted 80% over 1999’s rates. That trend has begun to close a longstanding gender gap in suicide, in which men were far more likely than women to take their own lives.
Dr. Steven H. Woolf, a Virginia Commonwealth University physician who has studied suicide in the U.S., says the trend of rising self-harm is, by now, well established.
“We really have to focus on what’s going on in people’s lives that’s driving so many to such desperate acts,” said Woolf, who chronicled what has become known as America’s “epidemic of despair” — rising death rates due to drug overdoses, suicide and diseases related to substance abuse — in a recent essay in the journal BMJ.
Woolf said that while depression remains a major risk factor for suicide and other forms of self-harm, scant access to mental healthcare has driven down diagnoses even as it allows despair to fester.
“But our research shows something more alarming — these increases are occurring in places that have been struggling for many years: places where incomes have been stagnant and poverty rates have been high. The pressures on middle-class and low-income families are considerable and have been a persistent problem for some years now, and it’s taking its toll.”
To address these problems, Woolf said, “the answer is not suicide hotlines. We need to focus on things that reduce stress on American families, and that includes economic assistance, jobs and access to education.”
The CDC report urges states to take a “comprehensive public health approach” to suicide prevention and address the range of factors contributing to suicide.
First among the strategies that the CDC has recommended to states in a 2017 “technical report” is to “strengthen economic supports,” including bolstering household financial security and adopting policies that stabilize housing.
The report also encouraged initiatives to strengthen access to mental health care and programs to improve problem-solving and coping skills in parents and schoolchildren.
MORE IN SCIENCE
‘I have definitely hit the jackpot.’ Advanced breast cancer disappears after new immunotherapy
For many lung cancer patients, Keytruda is a better initial treatment than chemotherapy, study finds
On Thanksgiving, partisan politics cost Americans nearly 74 million hours with family and friends
UPDATES:
3:40 p.m.: This article was updated with more details on and analysis of U.S. suicide trends.
This article was originally published at 11:20 a.m.







