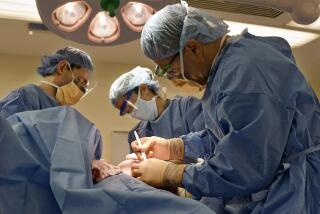
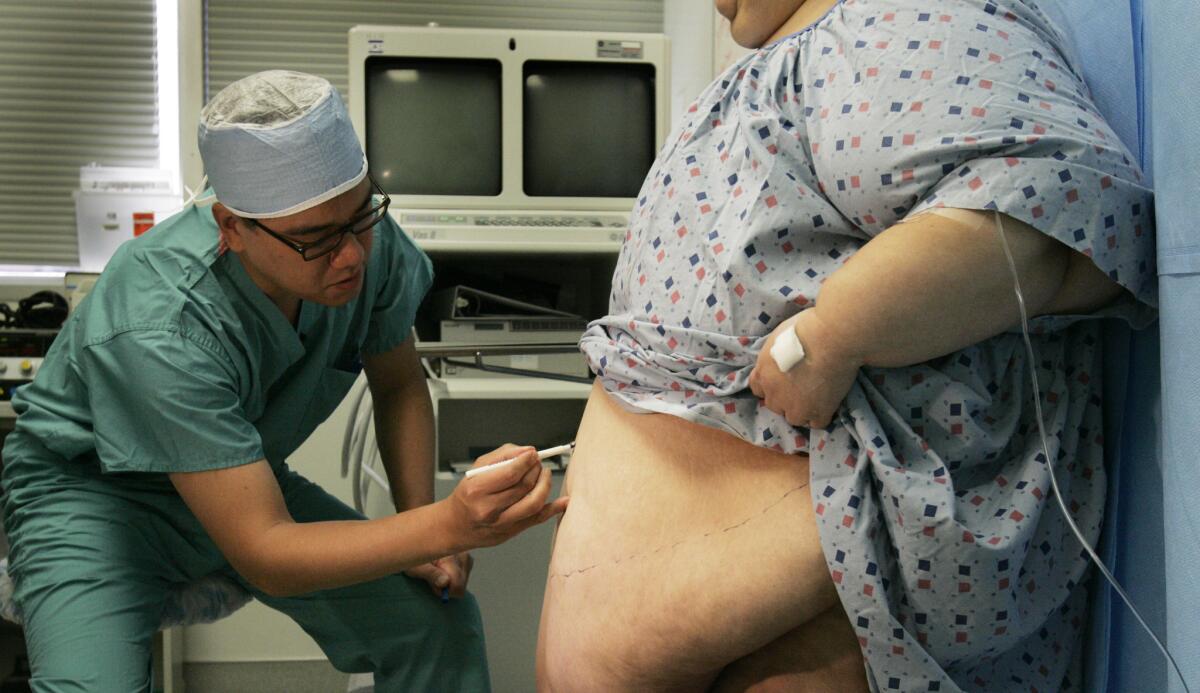
Obese patients lived longer if they had weight loss surgery, study finds
- Share via
Bariatric surgery has become the medical profession’s go-to solution for meaningful weight loss, and new research shows why: It saves lives.
In a retrospective study of close to 34,000 Israeli patients with obesity, the 8,385 who got one of three surgical procedures were roughly two times less likely to die over the next four years than were obese patients whose doctors gave them only weight-loss advice and encouragement.
It didn’t matter whether patients opted for gastric bypass surgery, laparoscopic banding or laparoscopic sleeve gastrectomy. All three procedures were associated with a lower risk of death compared with nonsurgical treatment.
The results were published Tuesday in the Journal of the American Medical Assn.
For every 1,000 “person-years” lived by the Israeli patients while they were part of the study, the ones who had surgery experienced 2.51 fewer deaths than the ones who didn’t.
After accounting for such factors as the patient’s age, sex and pre-surgical body mass index — along with whether they had diabetes, high blood pressure, cardiovascular disease or other medical issues — the study authors found that the risk of death during the four-year study period was twice as high for patients who avoided surgery than for those who got it.
When considering each type of surgery on its own, the researchers found that the risk of death for nonsurgical patients was 2 times higher than for patients who had laparoscopic banding, 2.65 times higher than for patients who had gastric bypass and 1.6 times higher than for patients who had laparoscopic sleeve gastrectomy. The differences among these three bariatric procedures weren’t large enough to be considered statistically significant.
Two related studies found that sleeve gastrectomy — a form of weight-loss surgery that has surged in recent years — is roughly as effective as gastric bypass, a forerunner that is more complex to perform.
In one of those studies, Swiss researchers found that five years after surgery, subjects who got sleeve gastrectomy and those who had the more complicated gastric bypass procedure lost essentially the same percentage of their excess weight — 25% for the former group and 28.6% for the latter.
The second study, conducted in Finland, found that gastric bypass resulted in slightly greater weight loss after five years. However, both procedures reduced patients’ need for diabetes, blood pressure and cholesterol medications at rates that were not significantly different from each other.
On the important subject of surgical complications, the studies found that sleeve gastrectomy and gastric bypass surgery each come with distinct risks. Sleeve gastrectomy patients were roughly 32% more likely than those getting gastric bypass to suffer a worsening of gastric reflux symptoms. But patients who got gastric bypass surgery were somewhat more likely to need to return for corrective surgery (22.1% vs. 15.8%) in the five years following their procedure.
In an editorial commenting on the findings, an obesity researcher and a bariatric surgeon acknowledged that, in embracing sleeve gastrectomy, the medical profession has not misplaced its bets.
“Collectively, these studies provide reassuring data to suggest that the rapid switch from Roux-en-Y gastric bypass to sleeve gastrectomy in the last decade has not been a therapeutic misadventure similar to the rise and fall of the adjustable gastric band,” wrote obesity specialists Dr. David Arterburn and Dr. Anirban Gupta, both of whom are based in the Seattle area. This surgery, better known as lap-band, “has been all but abandoned after being the most frequently performed bariatric procedure in 2008,” they wrote.
MORE IN SCIENCE
Even without nudging blood pressure up, high-salt diet hobbles the brain
Erosion is revealing surprising amounts of water ice on Mars