FDA approves much-debated Alzheimer’s drug panned by experts

- Share via
WASHINGTON — In a decision based as much on hope as on science, the Food and Drug Administration on Monday approved a drug designed to treat Alzheimer’s disease despite scant evidence that it improved the symptoms of patients who tested it.
The lack of a clear clinical benefit after two late-stage clinical trials prompted an FDA advisory panel to urge that the drug, called aducanumab, be rejected. The agency acknowledged the uncertainties about the medication but said its approval was justified by the seriousness of the disease and the dearth of options for treating it.
“We are extremely aware of the gradual and cumulative devastation that Alzheimer’s disease causes,” Dr. Patrizia Cavazzoni, director of the FDA Center for Drug Evaluation and Research, explained in a statement. “The need for treatments is urgent: right now, more than 6 million Americans are living with Alzheimer’s disease and this number is expected to grow as the population ages.”
The drug, to be marketed by Biogen Inc. under the brand name Aduhelm, reduces the amyloid beta plaques that build up in the brains of people with Alzheimer’s. That “is reasonably likely” to offer “important benefits to patients,” Cavazzoni said.
However, other experimental drugs have helped clear those plaques but not made any difference in patients’ ability to think, care for themselves or live independently.
Dr. Marsel Mesulam, director of the Cognitive Neurology and Alzheimer’s Disease Center at Northwestern University’s Feinberg School of Medicine, said he didn’t envy the federal regulators who had to make the call to approve aducanumab. Now that they have, he said, “we all hope that this was the right decision and ... that the drug is going to surprise us on the upside.”
Researchers may have found a tiny culprit — human herpes virus -- in the progressive loss of memory, thinking ability and identity that comes with Alzheimer’s disease.
Many scientists expect that Alzheimer’s patients will ultimately need a combination of drugs to successfully treat their disease. The approval of aducanumab could hasten their progress toward that goal by reinvigorating a field that hadn’t produced an FDA-approved drug since 2003.
“It will be the start of more investments, more attention, more focus on disease-modifying therapies directed at changing the course of Alzheimer’s disease,” said Dr. Zaldy Tan, medical director of the Jona Goldrich Center for Alzheimer’s and Memory Disorders at Cedars-Sinai Medical Center. “And perhaps one day, we will find a really effective and safe medication for Alzheimer’s disease.”
That sentiment was shared by Dr. Douglas Scharre, director of the division of cognitive neurology at Ohio State University Wexner Medical Center.
“It’s not a cure by any means or a reversal or anything of that sort, but it represents a key step that we’re finally getting somewhere,” said Scharre, who helped test the drug.
Researchers don’t fully understand what causes Alzheimer’s, but there’s broad agreement that plaques in the brain are just one factor, along with genetics, education and chronic health conditions such as diabetes and heart disease. The disease gradually attacks areas of the brain needed for memory, reasoning, communication and basic daily tasks.
Aducanumab is made from living cells and must be delivered via an infusion every four weeks. It was tested against a placebo in two clinical trials that each enrolled about 1,650 patients. Both studies were stopped early because the drug didn’t seem to reverse patients’ mental decline.
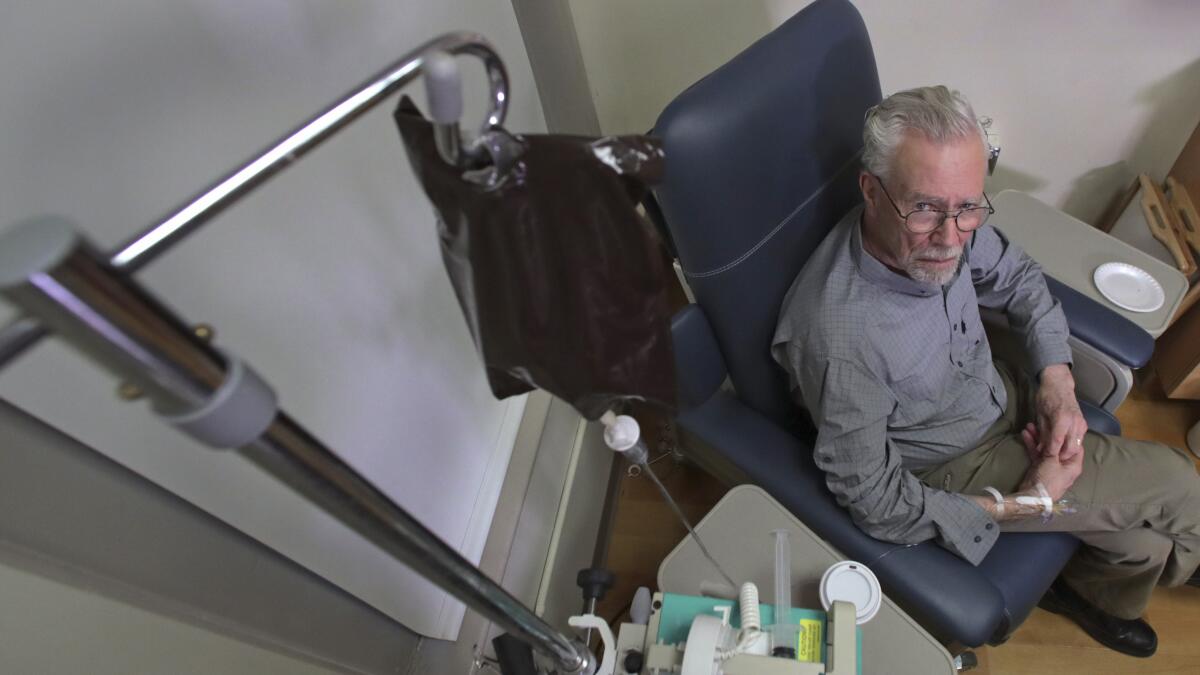
Biogen, which developed the drug with the Japanese pharmaceutical firm Eisai Co., later said that a new analysis of one of the studies showed the drug worked at higher doses. The initial trial results were poor because the dose given to some patients was too low, the company said.
That after-the-fact analysis was met with skepticism by many experts, including the neurological experts on the FDA’s advisory panel who voted not to recommend the drug for approval.
Patients taking aducanumab saw their thinking skills decline 22% more slowly than patients taking a placebo. But that meant a difference of just 0.39 on an 18-point scale of cognitive and functional ability. It’s unclear how such metrics translate into practical benefits, such as greater independence or ability to recall important details.
Also unclear is whether the drug’s small possible benefit will justify its hefty price. Biogen said the drug would cost approximately $56,000 for a typical year’s worth of treatment, though most patients won’t pay anywhere near that thanks to insurance coverage and other discounts.
The nonprofit Institute for Clinical and Economic Review, which studies drug value, estimated that a fair price for a drug with aducanumab’s modest benefits would be in the range of $2,500 to $8,300 a year. “Only a hypothetical drug that halts dementia entirely would merit” a list price of $56,000, the group said.
About 900 U.S. medical facilities are ready to begin prescribing the drug, according to Biogen, with many more expected in coming months. The company’s shares jumped 38% in trading Monday on the news, with analysts forecasting billions in future sales.
The often-discouraging search for ways to prevent or treat Alzheimer’s disease may have flickered to life this week with a bright new idea — and a buzzy new soundtrack as well.
Aducanumab got the green light under the FDA’s so-called accelerated approval pathway. That means Biogen will have to conduct a follow-up study to determine whether the drug works for patients in the real world, outside the parameters of a clinical trial. The company said it aimed to complete a follow-up trial by 2030.
If the results are poor, the FDA could rescind its approval and pull the drug from the market, though that rarely happens.
“Hopefully this is something that will work in the long run,” said Dr. Verna R. Porter, director of dementia, Alzheimer’s disease and neurocognitive disorders at Providence Saint John’s Health Center in Santa Monica. “But in terms of is this the right decision by the FDA, I think, only time will tell us.”
The approval makes aducanumab the only treatment that U.S. regulators have said can probably address the underlying disease, rather than manage symptoms such as anxiety and insomnia.
It was tested in people with mild dementia or early-stage Alzheimer’s, but the FDA label allows the drug to be prescribed to anyone with Alzheimer’s.
The label also says patients should get a brain scan before the seventh and 12th infusions to check for signs of swelling in the brain, a possible side effect that could cause headaches, confusion and dizziness. Other side effects include allergic reactions, diarrhea and disorientation.
The Associated Press was used in compiling this report.









