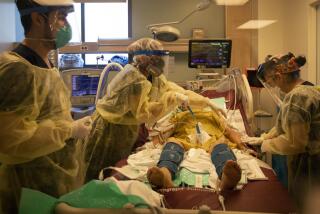
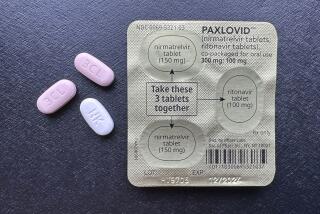
Evaluating risk and medical treatment in the time of coronavirus

- Share via
In 1939, at the outset of World War II, the British writer and theologian C.S. Lewis (1898-1963) delivered a speech titled, “Learning in wartime,” where he said, “War creates no absolutely new situation: it simply aggravates the permanent human situation so that we can no longer ignore it.”
We believe the same is true about the current pandemic in relation to many core philosophical issues in medicine.
The pandemic is making it harder to ignore conceptual complexities such as the evaluation of risk and the inherent uncertainties in diagnosis and treatment assessment. These issues have always operated behind the scenes of our medical system of diagnostic classifications and treatment protocols, but the public and medical personnel may be unfamiliar with the concepts behind the algorithms.
Risk guides much of our medical care system. We describe diagnostic and treatment options in terms of balancing risks and benefits. Insurance structures are built on a foundation of risk-pools. People with preexisting conditions are thought of as high-risk. The concept of risk is used with little reflection on its meaning. Many view risk as a form of “risky”: some activities are risky (binge alcohol consumption), and others are not (walking leisurely). Patients are often categorized in terms of risk; for example, some people are considered at-risk for diabetes. Yet, risk is merely a probability and as COVID-19 is showing us, unless we have developed immunity, we are all at-risk.
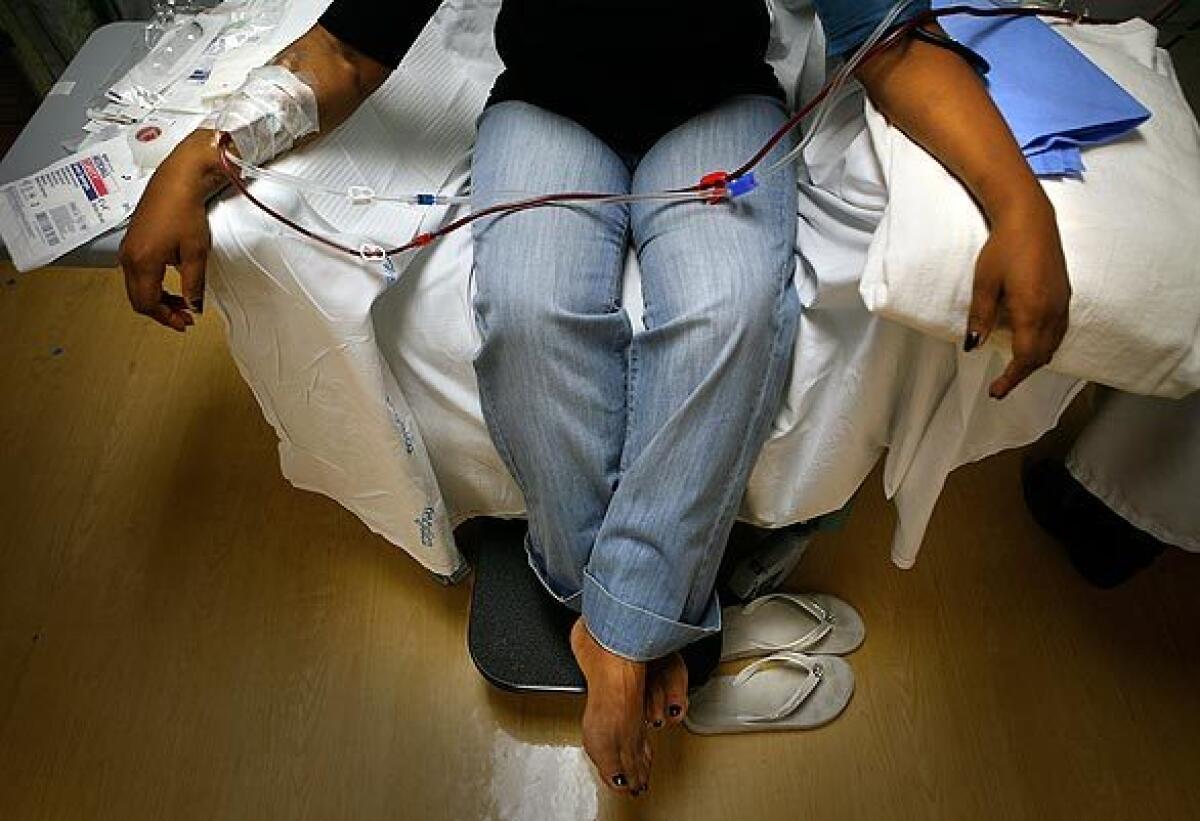
Our current medical protocols are based on risks for well-researched conditions such as cardiovascular disease. Insurance companies pay for clinical visits and laboratory evaluations when a person is categorized as at-risk for cardiovascular disease, for example after a screening test detects elevated cholesterol. Now, we are faced with reassessing the urgency for diagnosing and treating these established conditions given that COVID-19 appears to have a greater effect on life expectancy, at least in the short term. The contagious nature of the virus adds further disruption as travel to clinics or pharmacies for previously routine needs may put someone at greater risk for harm than if they had stayed at home. Clinics are actively discouraging visits to the office, seemingly destroying the previous protocols of care.
The importance of any test must be viewed in the context of risk tolerance. If one tested positive for something that had no effect on quality or quantity of life, then it would be unimportant. When it comes to COVID-19, what is our risk tolerance for recommending the main treatment at this time, quarantine? A random person on the streets of New York City today is at higher risk for coronavirus infection than a person in Minneapolis. Given that both are at-risk, what is an acceptable level of risk, and does this risk vary based on one’s community?
When should our recommendation for restrictions on movement be increased, such as avoiding grocery stores, or decreased, such as allowing visitation with extended family members? Acceptable risk is a judgment call anchored in the assessment of risk. When the pandemic began, we might have determined a risk of 1% too high to go out in public.
Now, a few months into the pandemic, a 1% risk may be viewed as lower than average and tolerable for someone to run errands. Judgment of risk may change when we know family, friends or colleagues who are suffering from the virus. As the virus spreads, behaviors that seemed atypical, such as wearing masks, may become commonplace.
The concept of risk determination requires us to face the reality of uncertainty. Tests are rarely 100% accurate. Existing tests for COVID-19 appear to be falsely negative in many who have the disease. Unfortunately, we don’t have independent knowledge of who does or does not have the condition; we only know who tests positive or negative. Determining the probability of illness given a test result requires some estimates, such as the probability of the condition prior to the test (which is never known precisely), and a calculation that seems to be difficult for many, including clinicians. Any test operates under the assumption of a gold standard to determine who has or does not have the condition. For immunity, is the gold standard the level of a specific antibody or the neutralizing ability of the antibodies?
There’s also uncertainty in the determination of treatment effectiveness. We can never be certain of proving effectiveness, but when studies are repeated with similar findings, we become more convinced. With COVID-19, there are not long-standing studies to repeat and the studies being done have few patients, so the debates about assessing treatment effectiveness are especially relevant. Scientists around the world are conducting studies on patients at various stages of illness, and we may soon be more certain of the effectiveness of treatments beyond quarantine.
Our previous medical structure was built upon disease conditions backed by decades of research. Now we are struggling with a new condition lacking previous research, and the public is witnessing decision-making based on the probability of illness, the accuracy of diagnostic tests and the likely results of treatment.
Will we learn anything from our struggle to combat COVID-19, either to help us prevent another pandemic or to better address everyday medical issues? It is our fervent hope that we are, as C.S. Lewis aptly put it, “learning in wartime.”

Clinicians and others in public health need more training to help them understand conceptual issues behind their protocols. This will lead to better science and patient care. Furthermore, the public and our governmental leaders must recognize that medical solutions take time: Interpretations of risk include a value judgment, diagnoses are not always clear, and treatment studies need to be repeated. These lessons are important during normal times, and imperative to help us prepare for future health crises.
The authors are both professors at the University of Minnesota, where they teach an undergraduate course titled, “Conceptual Issues in Medicine: Disease, Diagnosis and Intervention.” Alan C. Love, PhD, is in the Department of Philosophy and director of the Minnesota Center for Philosophy of Science. Steven D. Stovitz, MD, MS, is a physician in the Department of Family Medicine and Community Health.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.