His first coronavirus test was negative. Now, this 39-year-old city leader is on life support
- Share via
The coronavirus so ruthlessly attacked Gerardo Hernandez’s lungs that he now needs a ventilator to breathe for him. A tube delivers food to his stomach. His kidneys no longer function on their own.
The 39-year-old has spent the last three weeks lying unconscious in a hospital bed, barely clinging to life.
But when Hernandez was first tested for the coronavirus, when he showed up at an emergency room gasping for breath, he got a false negative and had to be retested. In the meantime, he began rapidly deteriorating and was moved into the hospital’s intensive care unit.
Hernandez, who is mayor pro tem of Adelanto, a small city in the Mojave Desert, is among the first wave of patients nationwide severely affected by COVID-19, a status that has brought challenges beyond the disease itself. His family and others like them are confronting a maze of issues around testing and treatment as the U.S. struggles to catch up with the virus that is devastating cities across America, yet remains poorly understood by doctors and scientists.
His wife, Tracy, and their three daughters cannot get tested for the virus because they don’t have severe symptoms. His 19-year-old niece, who also lives with them, has been tested twice for COVID-19 during two recent ER visits for coughing and shortness of breath, but the results have been negative. She has pneumonia that keeps getting worse.
“It’s overwhelming,” said Tracy, 38. The virus seemed serious when she and Gerardo saw it on the news, but it felt like they were peering at the threat through a window, that it was happening in the distance. “And then it hit him.”
::
In late February, Hernandez began coughing and sneezing, complaining of itchy eyes and a scratchy throat. He wrote it off as allergies or asthma, which he has had since childhood, his wife said.
The two married in 2013 and live in Adelanto with Gerardo’s mother, as well as their daughters and niece. Hernandez was elected to the City Council in 2018.
As March wore on, his symptoms worsened. He spiked a fever and began complaining that he was constantly tired, Tracy said. On March 18, an ambulance raced him to the hospital because he was so short of breath he couldn’t talk. His lips became tinged with blue.
Doctors at St. Mary’s Medical Center in Apple Valley diagnosed him with pneumonia, but he tested negative for the flu and other common illnesses.
In our effort to cover this pandemic as thoroughly as possible, we’d like to hear from the loved ones of people who have died from the coronavirus.
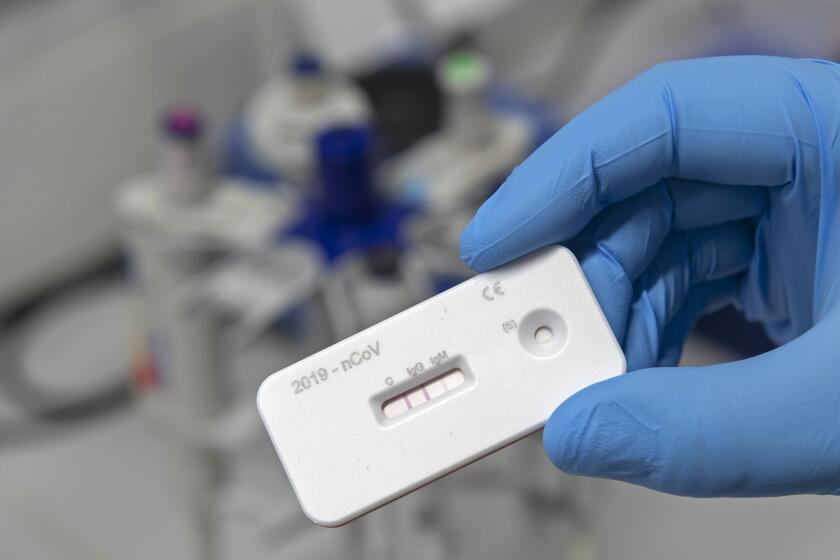
A bottleneck in processing lab tests delayed his COVID-19 test results, so they weren’t received until eight days after admission, a frustrating experience for Tracy, who desperately wanted to know if he had the virus. Then the test came back negative, followed by a second swab that came back positive.
The delays and false negative caused confusion and prevented doctors from moving quickly to start him on experimental medicines that may have helped his condition, Tracy said.
Several doctors have raised concerns that patients who almost certainly have COVID-19, including the characteristic pneumonia visible on a CT scan, are testing negative for the virus. A paper from China that was released before it was peer reviewed found that as many as 27% of patients with COVID-19 tested negative for the virus with a nasal swab test.
“The old dictum that we were taught in medical school is that clinical suspicion prevails. I don’t think that’s going to fail us ever,” said Dr. Neha Nanda, USC infectious disease specialist. “The sensitivity [of the test] is just a little bit up in the air.”
Repeat testing sometimes yields positives, perhaps because there is more virus in the patient’s body as symptoms become more severe, experts say. But for patients like Hernandez who are severely ill, doctors typically continue to treat patients as though they have COVID-19 even if the results are negative. There are not yet medicines proven to work for COVID-19, so doctors are mostly addressing the symptoms regardless.
False negatives can be more dangerous for milder cases when people, like health care workers, return to work or are told that they don’t have the virus and will recover on their own, experts say.
Tracy believes that has happened to her niece Christina. Since Gerardo was admitted to the hospital, his 72-year-old mother, Salome, has also fallen ill and is now also hospitalized for COVID-19. Christina, a sophomore at UC Riverside, had been caring for her grandmother as she became sick. The teenager has pneumonia, but has tested negative for the virus twice.
Experts say that when patients are tested for the virus, the swabs may not be getting shoved far enough back in the nose to get an adequate sample. Scientists also say the nasal cavity, compared with say the lungs, may not contain as much virus for the swab to capture.
“Seventy percent of testing errors, whether it be a false negative, a false positive are actually due to things before the sample is tested,” said Nam Tran, senior director of clinical pathology at UC Davis. The way the test is designed makes it much less likely to yield a false positive, experts say.
On March 21, Hernandez’s lungs filled up with so much fluid that doctors had to put him on a ventilator. He went into septic shock and multiple organ failure. They tried some experimental medicines, including the malaria medication hydroxychloroquine, but it didn’t seem to help and doctors tapered him off, Tracy said.
On Sunday, physicians told Tracy they did not believe he would make it through the night.
“He is one of the most critical patients they have on their ward right now,” Tracy said. “He is on life support ... that’s the scariest thing. I never knew in my entire life I would have to say that about my husband, but he is literally fighting for his life right now.”
A new L.A. County study will use blood tests for antibodies to the coronavirus to give officials a better sense of how COVID-19 has spread, how deadly it is and whether social distancing is working.
Nanda, of USC Keck, said the data from China and Italy showed that it was almost exclusively older people who died from the virus; but the American statistics have been different, with younger people getting extremely sick as well. It appears that asthma and obesity, not typically considered the most high-risk conditions, could be making people more vulnerable to serious illness, but physicians’ understanding evolves daily, she said.
“What I say in the morning often changes by 4 p.m.,” said Nanda, an infectious disease doctor. “We definitely have a lot to learn in terms of predisposing factors for patients who would succumb to this virus ... these are trying times.”
Tracy keeps detailed notes in a journal about her husband’s status, his blood pressure, his medication regimen, anything the nurses tell her. She plans to show Gerardo everything when he wakes up.
“I can say look, ‘This is the journey you’ve gone through,’” she said.
The two were in the same graduating class at San Gorgonio High School in San Bernardino decades ago. Tracy doesn’t remember him, but Gerardo told her years later that he said hi to her during a passing period and she laughed at him. They reconnected in 2012, and were married a year later.
Their seventh wedding anniversary was on March 19, the day Gerardo was admitted to the hospital. That was the last time Tracy saw him in person.
Gerardo continued to text her from the hospital until he was intubated and given a sedative to sleep. In the last text, he said he felt terrible and would call her when he woke up. Then he sent a string of kiss emojis and turned his phone off.
Tracy, often sitting alone in the bedroom she typically shares with him, still texts him regularly, though she knows he isn’t reading the messages.
On March 26, she wished him a happy birthday, along with a picture of their daughters celebrating with a strawberry cake.
In one text, she told him to dream of the farm they plan to own in Texas together when they retire. She has messaged him to say how she’s feeling. And videos of the girls.
She says he’ll read them when he wakes up.
Times staff writers Harriet Ryan and Emily Baumgaertner contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.