Surprise! You’re covered for the hospital, not the doctors
- Share via
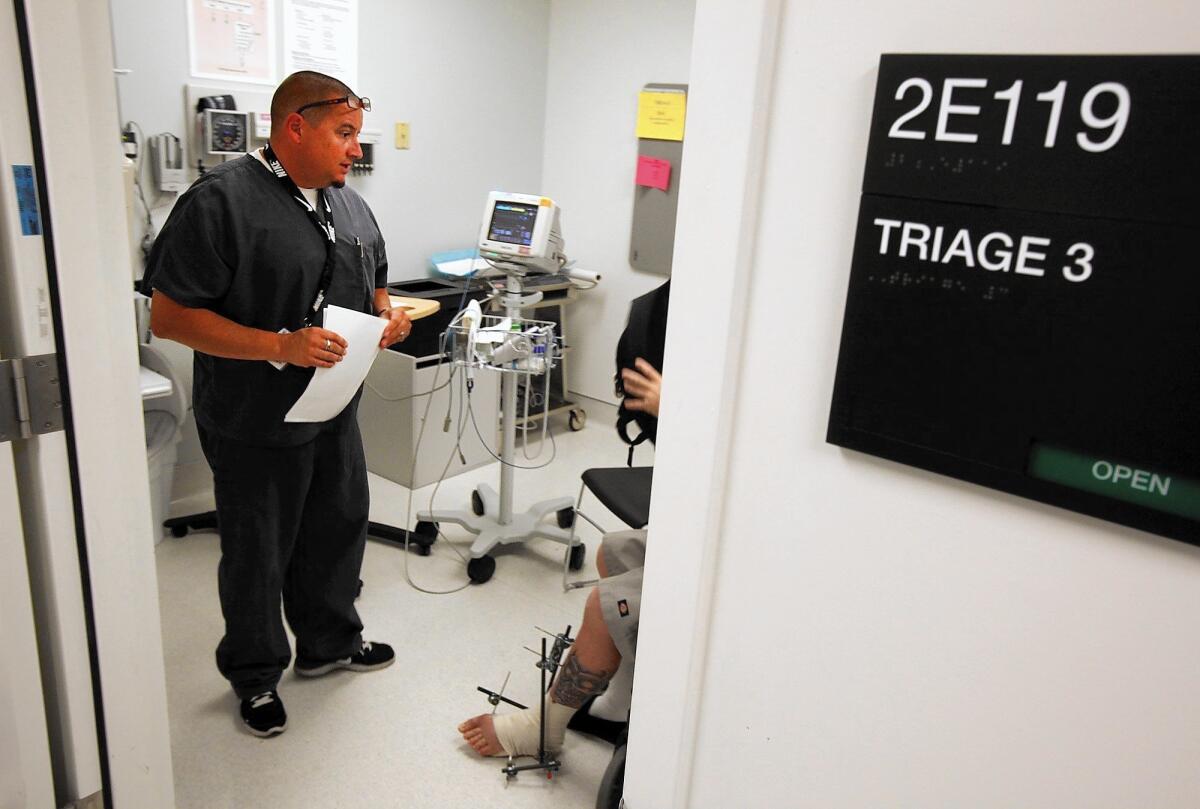
After Dave Connors’ teenage son broke his leg, he was rushed to an Orange County hospital that Connors knew was in his insurer’s coverage network.
It was only after the bills recently started arriving that he learned the doctors and anesthesiologist in the operating room were out of network, requiring him to pay thousands of dollars more.
“When you’re at a hospital that you know is in-network, who would think to ask individual people if they’re also in-network?” Connors said. “Especially when your son is being operated on.”
This wasn’t an isolated example of our patient-unfriendly, for-profit healthcare system.
Nearly a quarter of Californians who had hospital visits since 2013 were surprised to find that at least some charges at in-network hospitals were at out-of-network rates, according to a survey last year by the Consumer Reports National Research Center.
A bill — AB 533 — is pending in Sacramento that would fix this. However, it’s facing heavy opposition by doctors’ groups that say they’re fighting “a hostile act against the medical profession.” But they’re really just protecting higher fees.
Gerald Kominski, director of the UCLA Center for Health Policy Research, said it’s unreasonable to think that any patient or family member would inquire about the network status of healthcare practitioners at an in-network facility.
“No one would have the presence of mind to ask such questions amid the mayhem of a medical emergency,” he said. “It’s unconscionable.”
Connors’ 16-year-old son, a high school junior, broke his left femur during wrestling practice in January. He was rushed by ambulance to Hoag Hospital in Newport Beach for emergency care and then transferred to Hoag Orthopedic Institute in Irvine for surgery to install a metal brace.
Both facilities are in-network for Connors’ Anthem Blue Cross plan, purchased through Covered California, the state’s Obamacare exchange. He pays nearly $1,000 a month to insure himself and his family. The policy comes with a hefty $6,500 deductible.
Connors, a Costa Mesa resident, emphasized that he had “zero complaints” about the quality of care his son received.
The multiple bills he received were another matter.
Hoag sent Connors a bill for almost $46,000, including nearly $19,300 in “operating room services.” Anthem covered roughly 90% of that.
However, the two out-of-network surgeons submitted a bill for about $6,200 that wasn’t covered at all by the insurer. The out-of-network anesthesiologist submitted a bill for just over $3,100, of which Anthem paid a third.
“Apparently someone at Anthem thinks it was my responsibility to question them all,” Connors said. “I couldn’t have even gotten to the anesthesiologist unless I interrupted the operation.”
I contacted the doctors’ practice and found out that they do have a contract with Anthem but only for group plans typically offered through an employer. They have no contract for individual Anthem plans, such as those purchased through Covered California.
UCLA’s Kominski said understaffed hospitals routinely affiliate with outside doctors’ groups to help provide medical care. He said many such groups deliberately choose not to sign contracts with insurers for patients with individual insurance plans.
“That way these patients are always out of network, and the doctors can always bill full charge,” Kominski said. “It’s a market failure. It allows doctors to exploit the monopoly power that they have.”
Paul Ginsburg, director of USC’s Leonard D. Schaeffer Initiative for Innovation in Health Policy, said the onus should be on doctors and other medical practitioners to disclose their out-of-network insurance status to patients before treatment is delivered.
“The scope of insurance coverage is determined almost as soon as the patient arrives at the hospital,” he said. “It’s clear who’s in-network and who isn’t. There’s an ethical obligation for doctors to alert people if they’re out of network.”
Hoag Orthopedic Institute said in a statement that “we understand and empathize with the frustration and confusion medical bills often pose to families during what are already stressful times, especially when they receive several bills from a number of different entities involved in their care.”
Nevertheless, it said, hospitals can’t “dictate to physicians and other healthcare providers which insurance plans they must accept.”
That’s where AB 533 comes in. It wouldn’t impose any such requirement on medical professionals. But it would allow patients to pay only in-network rates at an in-network facility, regardless of the insurance status of individual doctors.
Assemblyman Rob Bonta (D-Alameda), the bill’s author, said the legislation already has been approved by Assembly and Senate committees, and he’s hopeful it will soon reach the governor’s desk.
I told him about Connors’ experience.
“These people did everything right,” Bonta responded. “They had insurance. They went to an in-network facility. They shouldn’t be required to pay out-of-network fees.”
Connors’ son is on the mend, and he’s grateful for that. But when I asked him to describe what he’s learned about our health insurance system, two words came to mind.
“Unfair” was one. “Insane” was the other.
That about sums it up.
David Lazarus’ column runs Tuesdays and Fridays. He also can be seen daily on KTLA-TV Channel 5 and followed on Twitter @Davidlaz. Send your tips or feedback to david.lazarus@latimes.com.
ALSO
3 dead in ‘horrific’ killings in Santa Barbara County hillside home
Olympus sought price hike for UCLA amid superbug outbreak
Graphic video appears to show Israeli soldier shooting Palestinian man in the head
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.











