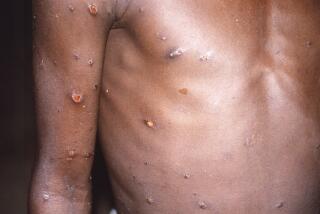
Experimental Ebola medication ZMapp saves infected monkeys
- Share via
In speedy testing conducted as West Africa’s Ebola epidemic began to mushroom, researchers have found that ZMapp, the experimental drug that has been used in seven infected human patients to date, prompted the recovery of 18 macaque monkeys infected with the virus.
Even when treatment with ZMapp was initiated five days after infection -- a point at which researchers describe the sick monkeys as being “three days away from death” -- the experimental biologic therapy reversed the bleeding, rashes and elevated liver enzymes that are Ebola’s hallmark symptoms, and drove the virus to insignificant levels.
Three infected macaques that did not get ZMapp were dead within eight days.
The trial of the drug in non-human primates -- the second yet conducted -- was performed in April and May by Gary P. Kobinger of the Canadian Public Health Agency’s national laboratory for zoonotic diseases and special pathogens. In the time the research was performed, the World Health Organization estimated that deaths from the “rapidly evolving outbreak” rose from 29 in Guinea alone to more than 200 in Liberia, Sierra Leone and Guinea.
In authoring the study, Kobinger was joined by a number of scientists from the San Diego-based biotechnology company, MappBio, that designed and developed ZMapp.
The study, published Friday in the British journal Nature, was conducted using a strain of the Ebola virus different from that circulating in West Africa today.
But Kobinger said the cloned antibodies at the heart of ZMapp appear to recognize and bind to both strains of the virus, and predicted it would work in those infected with either strain. In a preliminary test of the medicine against the circulating strain, said Kobinger, ZMapp “performed as well if not better” than it did on the version of the virus found earlier in Zaire.
In a call with reporters Friday morning, Kobinger called the results “fantastic news.” The finding “strongly supports” the hope that the experimental serum will rescue humans as well, even days after they have fallen ill. The progression of Ebola infection in macaques appears to be “extremely close to what we think is happening in humans,” added Kobinger.
“The evidence presented here suggests that ZMapp offers the best option of the experimental therapeutics currently in development for treating EBO-V-infected patients,” the authors concluded. “We hope that initial safety tests in humans will be undertaken soon, preferably within the next few months, to enable the compassionate use of ZMapp as soon as possible,” they added.
The latest experiment used a slightly altered form of ZMapp than was used in a published 2012 study, and higher doses of the ZMapp medication than have been seen in earlier animal experiments: Six animals started a nine-day, three-dose course of the medication three days after being infected with Ebola. And two other groups of six started the same three-dose course on post-infection day four and five.
Most of the monkeys were evidently ill as early as three days after infection -- they had begun to eat and drink less and become feverish, and the virus was detectable in their blood. By day five, their symptoms were “more pronounced,” said Kobinger.
In humans infected with Ebola, the average progression of the disease from infection to death has been 12 to 14 days, Kobinger said. While it’s difficult to infer a timeline for humans from that seen in macaques, he speculated that animals getting the medication five days after infection might be at a similar stage in the illness’s progression as humans at nine to 11 days after they had been exposed.
In macaques, the treatment showed no signs of causing harmful or bothersome side effects. But the Nature study did report that, in preliminary animal testing, infected macaques whose infection had progressed to the point where it was present in the central nervous system, were not rescued by ZMapp.
Thomas Geisbert, a professor of microbiology and immunology at the University of Texas Medical Branch at Galveston, called the drug’s success at treating gravely ill monkeys “a monumental achievement.”
But it remains unknown whether ZMapp was responsible for the recovery of two U.S. aid workers who received it in Liberia, Geisbert wrote in a commentary published with the study. So far, about 45% of patients stricken with Ebola have survived even without ZMapp, and two others who got the drug have died, he noted.
Given the extreme supply limitations of the ZMapp medication, Kobinger said the next urgent question for researchers will be whether smaller, or fewer doses--or doses that are tailored to a patient’s viral load--might work to reverse infection with the Ebola virus. MappBio says that its stocks are completely exhausted and Kobinger said it may be months before more is available.
But Kobinger said Friday he “would not expect” a single dose to lead to recovery. The antibodies in ZMapp “are really buying time,” he said, allowing the immune system to catch up with and overtake the Ebola virus’ replication. “In many cases, we need the second dose,” he added.