Benefits of HPV vaccine can be seen in high school girls, study says
- Share via
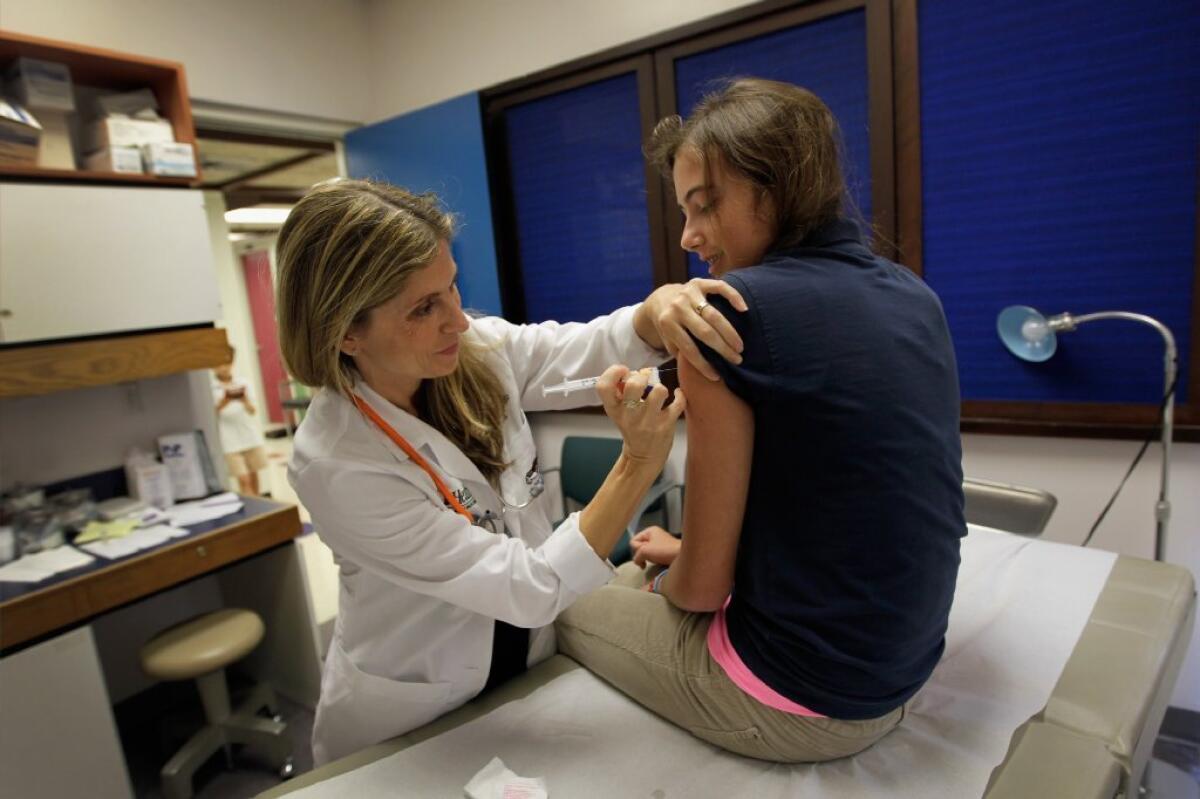
Years before the HPV vaccine prevents women from getting cervical cancer, it protects them against genital warts and cervical dysplasia, new research suggests.
A study of more than 260,000 teen girls in Ontario, Canada, finds that those who received all three doses of Gardasil were 44% less likely than their unvaccinated peers to be diagnosed with cervical dysplasia during their high school years. It also appears that the vaccine reduced the risk of genital warts by 43%, researchers reported Monday in the journal Pediatrics.
------------
FOR THE RECORD
An earlier version of this post said the study included information on more than 26,000 teen girls.
------------
Gardasil is billed as a vaccine against cervical cancer, a disease that typically strikes women in their 40s or 50s. (The median age at diagnosis is 48, according to the U.S. Centers for Disease Control and Prevention.) The CDC recommends that girls (and boys) get vaccinated when they are 11 or 12 – before they become sexually active and are exposed to the human papillomavirus.
But for many parents, there’s no sense of urgency about the vaccine. In 2013, only 57% of girls between the ages of 13 and 17 had received even one dose, and only 38% got all three, a CDC report found.
The authors of the new study emphasized that parents who believe there’s no harm in delaying the vaccine are putting their daughters’ health at risk. By targeting the four most dangerous strains of HPV, Gardasil can prevent a variety of medical conditions – including some that may lead to cervical cancer.
As the study results show, the protection kicks in fast.
“The fact that these benefits were observed in such a young age group strengthens current recommendations that vaccination should occur at an early age,” the study authors wrote.
The researchers, from McGill University and elsewhere in Canada, used national health records to identify girls in Ontario who were eligible for a free course of Gardasil while they were in the eighth and ninth grades and another group of girls who finished those grades before the province made the vaccine available for free. The researchers tracked the girls during 10th, 11th and most of 12th grade to see whether they were diagnosed with cervical dysplasia and genital warts, both of which are caused by HPV.
Fewer than 1% of girls who weren’t offered the vaccine for free went ahead and got it anyway, according to the study. Even among the girls who didn’t have to pay, only 50.6% got all three doses.
Still, the difference between the two groups of girls was striking, the researchers reported. For every 1,000 girls, there were 2.32 fewer cases of cervical dysplasia among those who were offered the vaccine than among those who weren’t. Cervical dysplasia is a condition characterized by abnormal cells that can lead to cervical cancer.
When the researchers focused on girls who were actually vaccinated, the gap more than doubled, to 5.7 fewer cases per 1,000 girls. That means that one case of cervical dysplasia was averted for every 175 girls who were vaccinated, the researchers calculated.
The story was similar for genital warts, which are also caused by HPV. For every 1,000 girls, there were 0.34 fewer cases of the warts among those eligible for the free vaccine than among those who weren’t. In addition, girls who followed through with vaccination experienced 0.83 fewer cases per 1,000 compared with girls who didn’t.
However, since genital warts were less common than cervical dysplasia (400 cases of the former compared with 2,436 cases of the latter), the benefits of the vaccine weren’t large enough to be statistically significant.
Still, the study results offer “new, strong evidence of the positive health impact” of the Gardasil vaccine on teens between the ages of 14 and 17. (Two similar vaccines are also approved for use in the United States – Cervarix, which targets two strains of HPV, and a new version of Gardasil that targets nine strains of the virus.)
“Policy makers and physicians can use these findings to substantiate arguments that delaying vaccination may result in missed opportunities for prevention,” the study authors concluded.
For more medical news, follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.