Insulin Pump Fares Well in UCI Study
- Share via
Dave Stenger, a laboratory assistant at UC Irvine, is 37 years old and has been a diabetic for 32 of those years.
Six years ago, Stenger began using an insulin pump to supply him with the insulin he needs to stabilize the level of glucose in his blood. Four years earlier, he had lost vision in one of his eyes as a result of his diabetes.
A study by UCI medical researchers to be presented later this month at a meeting of the International Diabetes Federation in Madrid, Spain, should, the researchers say, increase the credibility of the pump for diabetics and doctors alike.
Size of Pocket Calculator
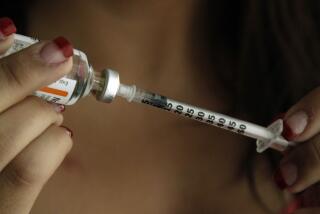
The pump, about the size of a pocket calculator, is worn by patients and administers insulin through a small tube buried beneath the skin of the abdomen. Unlike the periodic injections of insulin traditionally used by diabetics, the pump regulates the flow of insulin throughout a diabetic’s day.
“I’m a firm believer in the pump,” Stenger says. “If I weren’t on one I would probably have lost all my vision by now.”
Not everyone is as firm a believer as Stenger. Critics within the medical community have contended that the pump contributes to low levels of blood sugar, or hypoglycemia, and a concurrent rise in the blood’s levels of acid--a potentially lethal condition called ketoacidosis.
But UCI’s study concluded that the pump itself does not increase hypoglycemic episodes.
Supervised by Dr. M. Arthur Charles and Dr. Harvey Eichner, the study analyzed the effect of the pump on 46 Type I diabetics over a five-year period. Type I diabetics are those whose bodies do not manufacture enough insulin to maintain the correct level of glucose in the blood.
Charles, clinical director of the university’s Focused Research Program in Diabetes, said that the results of the study are “pretty spectacular.”
In the five years prior to receiving their pumps, the patients in the study had an average total of three hypoglycemic episodes requiring treatment by paramedics or hospitalization.
“A lot of people are afraid to go on a pump because they think the pump will cause more hypoglycemia,” Charles said.
Number of Attacks Reduced
But in their study, Charles and Eichner found that use of the pump reduced the incidence of severe hypoglycemic attacks from three in the previous five years to 0.2 in the five years of the study.
Charles stressed that use of the pump helps normalize the level of blood sugars which, in turn, can help a diabetic avoid suffering from the many complications associated with the disease.
Diabetes, Charles said, is the leading cause of blindness, kidney failure and kidney transplantation in the United States. Excluding accidents, it is the leading cause of amputations of the feet and legs and, excluding alcoholism, the leading cause of peripheral nerve disease.
“No one with diabetes has a normal life span,” he said. “Most of them really don’t know what’s in store for them.”
‘Will Convince Some’
Eichner said he feels that the findings of the study will “convince some people who are skeptical about the insulin pump to use it more frequently.”
Both he and Charles also cited the convenience of the pump for a diabetic.
” You have more flexibility with the pump,” Eichner said. “You’re free of the problems of injection.”
“It really can facilitate a diabetic’s life style,” Charles said. “And patients generally become more aware of diabetes when they have this machine hanging on their body.”
But the pump is not a fail-safe means of diabetes treatment.
“Like any drug or device,” Charles said, “if it’s not used properly, it’s dangerous.”
Ketoacidosis Is Problem
There are other problems, too. Charles said the biggest problem with portable insulin units like the pump is ketoacidosis. When the level of sugar in the blood is not normal, the body turns to other sources, including body fats. Acids within the fats are released into the blood, causing ketoacidosis.
Charles said that studies done in the United State and other countries show as much as a 17 times higher incidence of ketoacidosis episodes in pump users compared to non-pump users. Although the UCI study showed no increase in the level of ketoacidosis episodes among those patients it studied, the number of episodes did not decrease, either.
“The number of episodes is too high and that is one aspect of the study we’re not happy about,” Charles said. “But we’re working on it.”
Charles said that UCI, which helped develop the technology for the pocket-sized pump, also is helping develop pumps that can be implanted underneath the skin of the abdomen. He estimates that the medical center will be implanting such pumps in humans by the end of the year.