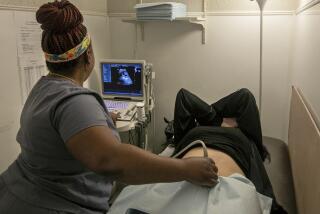
Ultrasound and the Matter of Competency
- Share via
THE PROCEDURES OF perinatology--ultrasound, amniocentesis, chorionic villi sampling, selective termination of pregnancy and in utero surgery--are risky physically, and some require sophisticated interpretation. Yet there are few specific standards applied to their use. The lack of restriction gives a doctor like Dr. Khalil Tabsh the chance to “experiment” and save babies; it could also lead to tragic mistakes.
Ultrasound is perinatology’s backbone, and the situation surrounding guidelines for its use provide an example of the difficulties and importance of regulation.
“There are no standards,” Tabsh says about ultrasound. “Some doctors have good training. And some have almost none. . . . You can teach a resident to do this and to do that. But to be good at it, (he has) to be able to three-dimensionalize (the images on the video screen) and to do a lot of them.”
Even doctors in major medical centers, privy to the latest in research and diagnosis, argue over who should perform ultrasound and what degree of training and experience qualifies a person to perform the procedure. Guidelines were promulgated in recent years by an interdisciplinary panel of the American Institute of Ultrasound in Medicine and the American College of Radiology, but the American College of Obstetricians and Gynecologists (ACOG) refused to endorse them, saying the procedure would be difficult to police. Later, ACOG suggested its own guidelines, but they remain just that--suggestions.
While the arguments and the turf battle rage on, the latest National Institutes of Health surveys suggest that more than half of all pregnant Americans receive ultrasound exams during pregnancy, even though ACOG does not recommend them as routine tests in normal, untroubled cases. At an average cost of $150 per exam, ultrasound has become a $1-billion-a-year business.
The lack of standards has grown so acute that some experts suggest we’re at the precipice of a “medical-legal mine field.” According to a recent article in the American Journal of Obstetrics and Gynecology, misinterpretation of findings is a common charge in malpractice lawsuits involving obstetricians who perform ultrasound exams. A recent study of 120 actual or threatened lawsuits revealed that more than half involved ultrasound misdiagnosis.
“Ultrasound is the worst thing going on in medicine right now, just a real mess,” says Roy A. Filly, professor of radiology and obstetrics and gynecology at UC San Francisco Medical Center. “And it’s getting worse all the time because it’s 90% financially motivated.
“Right now, there’s nothing to stop someone from buying a machine for his office who has zero credentials to use it. Equipment companies go around to private offices, showing doctors fact sheets so they can see what they can earn from using it. That’s why it’s being used. We need regulation.”
Currently, an advisory panel to the U.S. Food and Drug Administration is grappling with the question of ultrasound guidelines for doctors, equipment manufacturers and patients. At the same time, the California Department of Health Services is upgrading its standards, but only for the most highly skilled sonographers, like Tabsh, who are approved to perform exams for state-run prenatal screening programs.
For now, experts caution that even in the best hands, ultrasound technology is imperfect. Tabsh says he once had a patient whose fetus he diagnosed as having hydrocephalus--”water on the brain”--which is linked to mental disability. A second opinion confirmed his diagnosis. Follow-up ultrasound scans showed the same problem, so the patient requested an abortion. But at 22 weeks, Tabsh checked again. This time, the problem had disappeared. The patient gave birth to a healthy baby.
“If you act just based on one scan and terminate the pregnancy,” he says, “you might be terminating a lot of normal babies.”