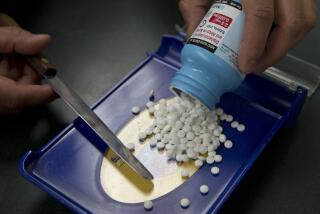
Gilead’s Research Goes to Front Lines
- Share via
FOSTER CITY, Calif. — John C. Martin is a rarity in post-Enron America: The Gilead Sciences Inc. boss actually wants to spend time in jail.
Right now, he’s arranging a trip to New York’s municipal lockup on Rikers Island. He already has visited Chicago’s vast Cook County Jail, submitting to pat-downs and metal detectors.
For Martin, it’s about getting to know his customers: people infected with human immunodeficiency virus who use Gilead’s drugs. The mission has taken the 52-year-old Martin, a chemist by training, to the front lines of the deadly AIDS epidemic -- crowded prisons and clinics in tough urban neighborhoods.
The face-to-face meetings with hard-luck patients have been eye-openers. At Cook County Jail, he learned that detainees often stop taking their medications drugs once they are released. Martin said he was considering a pilot program to address the problem.
“The system doesn’t serve them very well,” he said.
But Martin’s jail tours serve the bottom line: After he met with Dr. Kirby Cunningham, who treats HIV-infected patients at the jail in Chicago, Gilead assigned salespeople to the correctional system.
Martin’s visit “showed him corrections has special needs,” Cunningham said. “And it’s a big market.”
The chief executive’s hands-on style is an important reason that Foster City, Calif.-based Gilead has emerged as a leader in HIV medications. Though the company is little known outside that niche, Gilead’s market value exceeds $13 billion, higher than that of Sears, Roebuck & Co. or Southwest Airlines Co. The company, which turned profitable in 2002, is expected to report strong quarterly earnings today.
Sales of the flagship product Viread should exceed $500 million this year. And this month Gilead launched its second HIV drug, Emtriva. With it, the company hopes to steal significant sales from the industry giant, GlaxoSmithKline.
On Wednesday, Gilead’s shares closed at $68.79, down $1.20, on Nasdaq.
“The company is firing on all burners,” said Bear, Stearns & Co. analyst Ronald C. Renaud.
Launched in 2001, Viread is one of the few once-daily medications available to HIV patients. The convenience offered by the drug, which works by blocking an enzyme that HIV needs to replicate in human cells, is a big part of its success.
People infected with HIV must follow complicated treatment regimens to prevent development of full-blown acquired immune deficiency syndrome.
Each day, San Franciscan Ross Woodall, 50, takes 14 oral medications in 32 pills, downing the pale-blue Viread pill with a late-night snack -- and with a sense of relief. Just a few years ago, Woodall consumed 68 pills each day; to stay on schedule, he toted a satchel with his medications, a water bottle and snacks.
“It may seem insignificant, a once-a-day pill,” Woodall said. “But I look forward to taking it. It is the only time that day I have to think about this pill.”
Moving to leverage its success, Gilead plans a once-daily tablet combining the company’s two HIV drugs into a pill aimed at Glaxo’s top-selling twice-a-day Combivir. The combo drug won’t be ready until 2005 -- but the Gilead brass already is bad-mouthing Combivir, which had worldwide sales of $882 million in 2002.
Martin noted that Combivir contains AZT, which can cause severe anemia. “Patients on AZT have to take EPO,” he said, referring to the costly injectable drug that improves blood counts.
A Glaxo spokeswoman responded that “Combivir is the cornerstone of the 10 most prescribed regimens” for HIV patients, adding, “I think that speaks for itself.”
Gilead was founded in 1987 to find drugs to control disease-causing genes. The research was cutting-edge, backed by such savvy financiers as Benno Schmidt of venture capital firm J.H. Whitney & Co., who was chairman of the President’s War on Cancer under Nixon, Carter and Ford.
Early on, none of Gilead’s experimental drugs worked outside the laboratory. “We were never able to show any effects in animals,” former Gilead scientist Jeff Bird said. “It was a tough nut to crack.”
In 1989, the merger of two New Jersey drug firms set in motion events that would transform Gilead. After the $12-billion acquisition of Squibb Corp. that year, Bristol-Myers Squibb Co. trimmed the HIV drug program run by the former Bristol-Myers Co. Martin, then head of Bristol-Myers’ antiviral research unit, resigned and jumped to Gilead to run its research and development. He became CEO in 1996.
Martin, the rare scientist with a businessman’s eye, aggressively pruned Gilead’s research programs and focused the company on AIDS.
From afar, the decision looked risky. Gilead’s competitors were the largest drug makers in the world, including Martin’s former employer. Bristol had developed Zerit, which in 2002 was the world’s fifth-best-selling HIV drug.
That didn’t deter Martin.
“We had the professional athletes of the business,” said Martin, an Oakland Raiders fan. His team included the co-inventor of a widely used organ transplant drug, a chemist who had determined the structure of the HIV protease enzyme and a founding scientist of Genetics Institute, which now is part of Wyeth.
Martin was no slouch either. Early in his career at Syntex Corp., now part of Roche, he was co-inventor of the antiviral drug ganciclovir, which treats a type of herpes infection that caused blindness in AIDS patients. Later at Bristol, he worked on Zerit and another HIV drug, Videx.
Thanks to Martin, Gilead had obtained a license to experimental antiviral drugs that Bristol abandoned after the Squibb acquisition. The license covered a library of chemicals invented by two European scientists that mimicked natural nucleotides, the building blocks of DNA. HIV needs these building blocks to make copies of itself.
Martin believed that HIV could be tricked into accepting useless synthetic nucleotides. If the virus did so, he reasoned, it would be unable to replicate. (Think of a key that fits into a lock but can’t turn the bolt.)
Conventional wisdom held that synthetic nucleotides couldn’t get inside human cells, where HIV lurks. Bristol’s decision to abandon the work added to the pessimism.
Gilead had an early success with Vistide, an intravenous herpes medication similar to Syntex’s ganciclovir, familiar territory for Martin. Though the market for Vistide was small, to the businessman in Martin it was the basis of a broader virus-fighting franchise. He planned to develop it as a vaginal cream for genital herpes and as eyedrops for other viral infections.
But Vistide, which required hours-long infusion, was found to cause severe kidney damage -- too risky for widespread use beyond the herpes cytomegalovirus responsible for AIDS-related blindness. Martin’s spinoff projects were dropped.
The next drug culled from Gilead’s chemical portfolio, adefovir, also harmed patients’ kidneys. Some AIDS patients who took it in clinical trials died.
Gilead nonetheless sought regulatory approval in late 1999 for adefovir. Respected clinicians urged the Food and Drug Administration to approve adefovir for AIDS patients who had few treatment options.
AIDS activists attending a public hearing urged the FDA to reject the drug -- “I wouldn’t give it to my cat,” said one -- and an agency panel voted it down.
Wall Street reacted furiously to the FDA panel decision, driving Gilead’s shares down by nearly 25%.(The FDA approved a lower dose of adefovir for hepatitis B last year.)
Martin shifted the company’s attention to a third nucleotide drug called tenofovir, which already was in human tests. It became Viread.
The drug first drew attention in late 1995, when a paper in the prestigious journal Science reported that intravenous tenofovir prevented HIV infection in 25 monkeys. At a conference in Japan the next spring, research chief Norbert Bischofberger reported that tenofovir gel prevented vaginal infection in six monkeys.
“Our stock went up $6,” Martin recalled.
Gilead scientists re-engineered tenofovir into a once-daily pill. Then, lacking a global sales force, Martin bought one.
In 1998, Gilead acquired a small Colorado company called NexStar Pharmaceuticals, which had an international sales team and a cash cow in an anti-fungal drug, Ambisome, with annual sales of $100 million.
Over time, Martin dismantled what remained of NexStar. That “broke my heart,” said former Chairman Larry M. Gold. But NexStar, like many small biotechnology firms, had burned through millions of dollars on scattered research projects and didn’t survive. Gold said he admired Martin’s unwavering focus on antiviral drugs and HIV.
Martin “has this singular vision,” Gold said. “He refuses to get distracted. I think that’s a big part of their success.”
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.