Antivirals may aid H1N1 if misused
- Share via
Indiscriminate use of antiviral medications to prevent and treat influenza could ease the way for drug-resistant strains of the novel H1N1 virus, or swine flu, to emerge, public health officials warn -- making the fight against a pandemic that much harder.
Already, a handful of cases of Tamiflu-resistant H1N1 have been reported this summer, and there is no shortage of examples of misuse of the antiviral medications, experts say.
People often fail to complete a full course of the drug, according to a recent British report -- a scenario also likely to be occurring in the U.S. and one that encourages resistance. Stockpiling is rife, and some U.S. summer camps have given Tamiflu prophylactically to healthy kids and staff, and have even told campers to bring the drug to camp. Experts anticipate more problems in the fall as children return to school and normal flu season draws nearer.
“Influenza viruses mutate frequently and any viral resistance could be acquired easily,” said Dr. Anne Schuchat, director of the National Center on Immunization and Respiratory Disease at the Centers for Disease Control and Prevention in Atlanta. “It won’t surprise us if we see resistance emerge as a bigger problem in the fall or in the years ahead.”
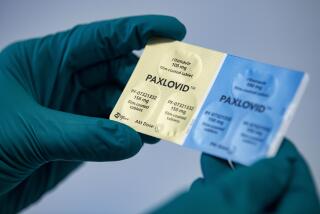
Prescribed in pill form, Tamiflu (oseltamivir) works by preventing the flu virus from leaving infected cells and spreading to new ones. Because a vaccine against pandemic H1N1 influenza will not be widely available for several months, Tamiflu and to a lesser extent Relenza (zanamivir), an antiviral that acts similarly, are key medical tools for fighting the pandemic in the meantime.
On Friday, however, the World Health Organization advised doctors that even those who are sickened with swine flu do not need to be given Tamiflu or Relenza if they are only mildly or moderately sick and are not in a high-risk group (such as children under 5, pregnant women and those with an underlying health condition).
Both drugs can help prevent illness in people exposed to the virus and reduce illness severity in people already sickened with it. On Aug. 14, after U.S. national soccer team forward Landon Donovan was diagnosed with H1N1 flu, players, coaches and support staff of the U.S. and Galaxy teams were advised to take Tamiflu as a preventive measure.
Tamiflu was chosen a few years ago for stockpiling by the federal government to deal with future pandemics.
Health authorities in the United States and elsewhere are keeping a sharp eye on prescriptions of the drug as they prepare for a surge of H1N1 cases in the fall. The U.S. government has issued detailed guidelines on prescribing antivirals. But health professionals may not follow the recommendations or may give in to patients who pester them for prescriptions that are ill-advised, said Dr. Robert Schechter, acting chief of the immunization branch of the California Department of Public Health.
“These medicines can be very helpful to those who could get very sick,” Schechter said. “But excessive use will accelerate the development of resistance and lead to the lack of a medication for everybody.”
Anxiety over indiscriminate use is growing, and taking the medications cavalierly is not without consequence. British health authorities reported Aug. 2 that cases of side effects from Tamiflu had doubled in the prior week, coinciding with the July 24 launch of a program in England to provide antivirals to anyone with H1N1 influenza who requests it over the phone or online.
In the first three days of the program, 150,000 packets of Tamiflu were dispensed and 293 cases of side effects were reported. Tamiflu can cause vomiting, diarrhea and mild neuropsychiatric effects.
Some U.S. health authorities have also expressed concern over misuse of the medications. Last month, the CDC urged directors of summer camps to stop handing out Tamiflu to healthy campers.
Americans are known to hoard antivirals: A 2006 study showed that heightened anxiety over a possible avian flu pandemic caused Tamiflu prescriptions to soar 300% in 2004 and 2005.
Just as with antibiotics, of central importance to antivirals’ success is taking them properly, including completing the recommended course.
However, a study published in late July found poor adherence among children in London who took Tamiflu for prevention of pandemic H1N1 in the spring.
Less than half of the grade-school-age children and only 76% of the 13- and 14-year-old students completed a full course of medication.
More than half of the children reported side effects, such as nausea, stomach cramps and trouble sleeping. Almost one in five reported a neuropsychiatric side effect, such as poor concentration, confusion or bad dreams, even though the U.S. Food and Drug Administration says neuropsychiatric side effects are rare.
Moreover, a study published this week found that Tamiflu and Relenza are unlikely to prevent complications, such as asthma flare-ups or ear infections, in children who have seasonal influenza. But they do increase the risk of vomiting.
The authors of the study, published in the British Medical Journal, said they don’t know if their findings can be generalized to the pandemic flu strain.
Antiviral drugs can be underutilized as well as overused, Schechter said. Some Californians who have died from novel H1N1 influenza did not receive antivirals.
“I’m afraid the medications are not being used in some instances where they should,” he said. “But there are also international reports of resistance developing. Both of those extremes are concerning.”
A handful of resistant H1N1 cases have been reported worldwide among people who had taken Tamiflu preventively: three in Japan, and one each in Canada, Hong Kong and Denmark.
Those cases are not surprising nor of great concern to health authorities, said Dr. Tim Uyeki, a medical epidemiologist with the CDC. They are cropping up sporadically and don’t seem to be spreading from person to person.
“The most important question for public health is not whether sporadic cases occur but whether there is ongoing transmission of oseltamivir-resistant strains,” Uyeki said.
The most perplexing case of Tamiflu resistance arose in June when a San Francisco teen who had flown to Hong Kong was found by authorities there to be ill with pandemic H1N1 flu. The girl, who recovered, had never taken Tamiflu.
A state investigation of people who were in close contact with the girl, as well as tests of 251 H1N1 virus samples from sick patients in California, has not turned up evidence of a resistant strain circulating here, Schechter said.
But nothing, in theory, would stop such a strain from developing, then circulating. In recent years, several strains of regular, seasonal H1N1 influenza have developed resistance to antiviral medications.
And a study published in March on the spread of the H5N1 avian flu, which has been circulating worldwide in bird flocks in recent years and has killed 262 people, showed the virus rapidly developed resistance to a different class of antiviral drugs, adamantanes.
“With bird flu, we found some resistance started in China and spread throughout the world in a few years,” said study author Daniel Janies, an evolutionary biologist at Ohio State University. “Overuse contributes to resistance. Basic natural selection predicts it. We can demonstrate why you should not use these drugs unless you have to.”
Other antiviral drugs exist, but the pandemic H1N1 virus is resistant to the adamantane class. If it develops resistance to Tamiflu also, only Relenza would be left to treat the illness, barring the development of new antiviral medications.
Relenza, Schechter said, is indicated only for ages 5 and older. Used less commonly than Tamiflu, it is inhaled as a powder, and people who are seriously ill or have difficulties with breathing cannot take it.
“The more choices you have, the better for treatment,” Schechter said. “To lose any one of those options would pose great challenges for treatment of those who are most vulnerable or likely to die.”
--
Grahame L. Jones contributed to this story.
grahame.jones@latimes.com
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.